Staying Hydrated and Healthy in El Paso’s Heat
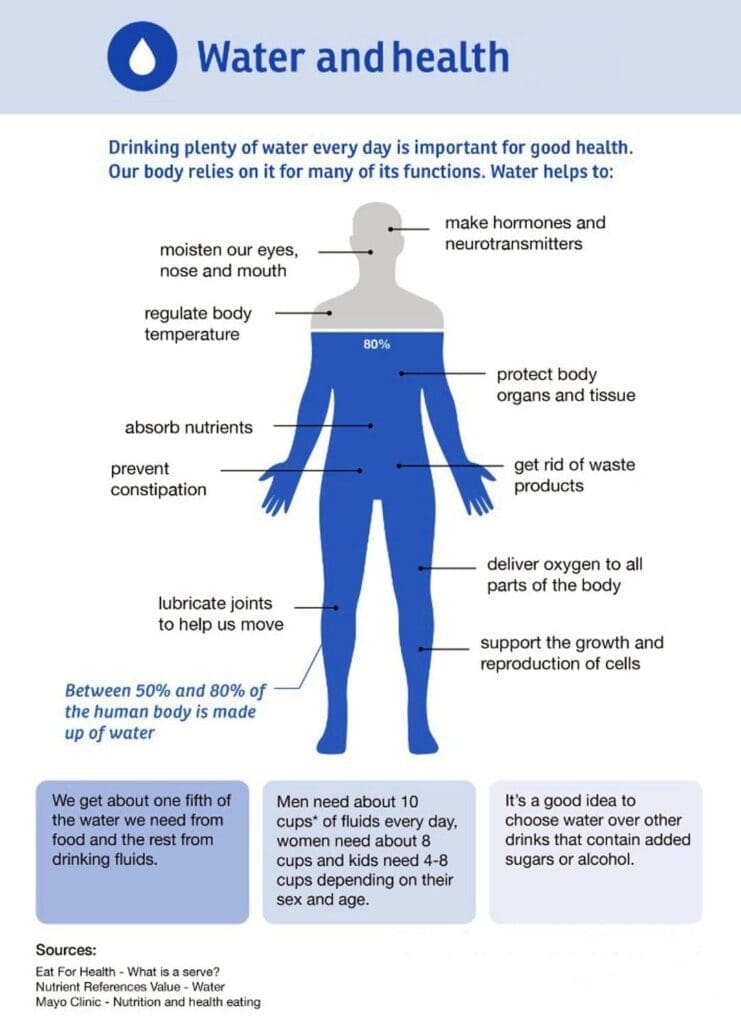
El Paso’s dry desert heat creates real challenges for the body. High temperatures and low humidity cause sweat to evaporate fast, leading to quick loss of water and key minerals. Without proper steps, people can feel tired, get muscle cramps, or struggle to stay comfortable. At ChiroMed Integrated Medicine in El Paso, experts recommend focusing on foods and supplements that boost internal hydration, replace lost electrolytes, and use light proteins that digest easily.
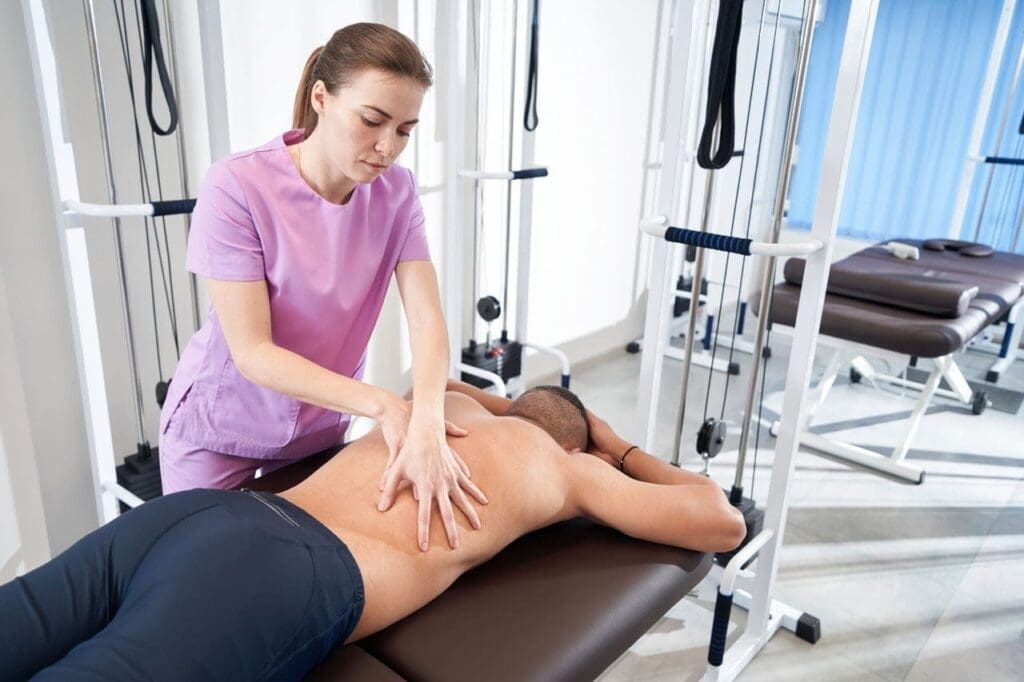
The clinic uses a clear “3-part system” for nutrition in heat: eat water-rich foods, restore minerals with electrolytes, and choose smaller, more frequent meals. This reduces extra internal heat from heavy digestion. Integrative chiropractic care at ChiroMed supports this plan by helping the autonomic nervous system regulate temperature more effectively and keeping spinal discs hydrated. While chiropractic does not directly set body temperature, it strengthens the body’s systems to manage heat stress more effectively.
Why El Paso’s Desert Climate Demands Special Care
In El Paso, the dry air quickly pulls moisture from the skin and body. Even drinking plain water may not fully balance things because sweat removes sodium, potassium, and magnesium. This affects energy, muscles, and comfort. Big meals add warmth inside the body, making the outside heat feel worse. ChiroMed’s approach helps people handle these issues so they can enjoy daily life, work, and outdoor activities more comfortably.
The clinic’s team, led by Dr. Alex Jimenez, DC, APRN, FNP-BC, combines chiropractic, nutrition counseling, and holistic methods. This fits perfectly for locals facing desert conditions year-round.
The 3-Part System for Heat Nutrition at ChiroMed
ChiroMed promotes a simple “3-part system” to help people thrive in El Paso’s heat.
- Water-rich foods provide steady, natural hydration that lasts longer than plain water alone.
- Electrolyte replenishment restores minerals lost in sweat to keep muscles and nerves functioning well.
- Smaller, more frequent meals lower the heat produced during digestion and keep energy levels steady.
These steps work together to improve fluid balance, reduce strain, and enhance overall comfort in dry weather.
Water-Rich Foods for Natural Internal Hydration
High-water-content foods are a top recommendation at ChiroMed for staying cool inside. Watermelon is over 90 percent water and easy to digest, making it ideal for hot days (Kaiser Permanente, n.d.). Cucumbers are nearly 97 percent water, low in sugar, and refreshing (Jefferson Health, n.d.).
Other strong choices include strawberries, oranges, celery, and leafy greens like spinach. These add potassium for muscle support, fiber for smooth digestion, and antioxidants to handle sun exposure. Simple ideas like cucumber slices in water or melon snacks fit easily into daily routines. Fruits and vegetables as meal bases help lower the body’s heat load in El Paso’s climate (Washington Post, 2023).
Restoring Electrolytes to Replace What Sweat Takes Away
Sweat in the desert quickly removes important electrolytes. Sodium helps balance fluids, potassium supports heart and muscle function, and magnesium supports many processes. Low levels can cause weakness or cramps. Natural sources such as bananas, dried apricots, black beans, cashews, almonds, and peanuts provide magnesium and potassium (Physical Dimensions Integrative Health Group, 2024).
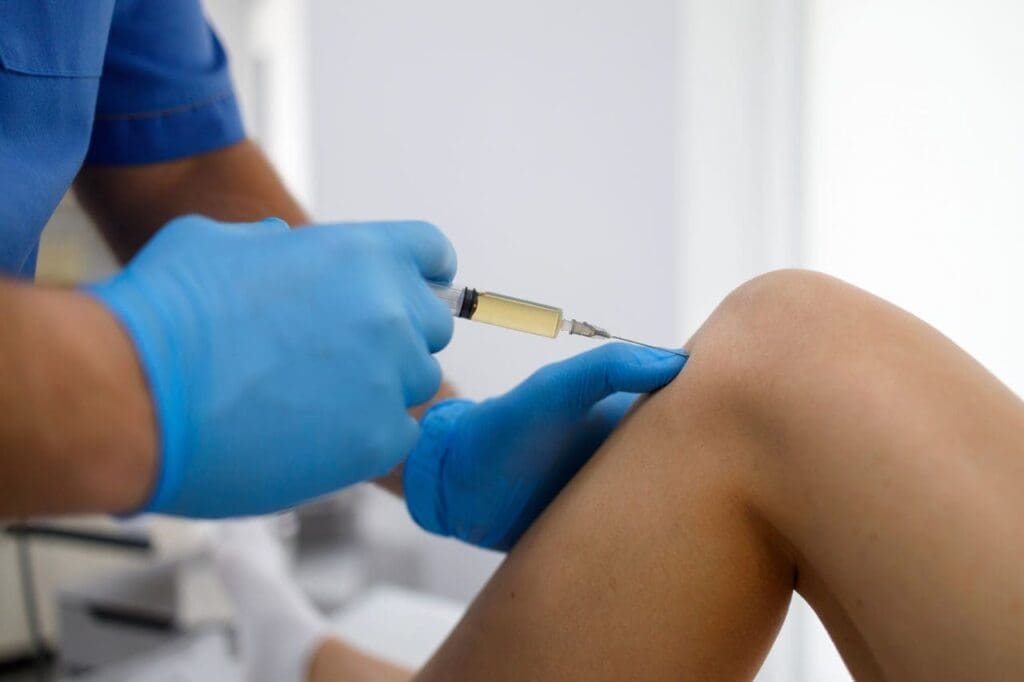
ChiroMed’s nutrition counseling often includes electrolyte supplements for active people. Balanced options without extra sugar help, especially high-sodium ones for heavy outdoor activity (Drinksote, n.d.). Vitamin C supports sweat gland function and heat response (Makers Nutrition, 2022). Combining food sources with targeted supplements helps keep levels stable and prevent heat-related problems.
Smaller Meals and Light Proteins to Reduce Internal Heat
Large meals make the body work hard, creating extra warmth that adds to desert heat. Smaller, spread-out meals ease this burden. Light proteins digest better and avoid overload. Options like grilled chicken, fish, tofu, eggs, or beans pair well with vegetables and fruits.
ChiroMed encourages this eating style to maintain energy without strain. It aligns with the clinic’s focus on nutrition for wellness and recovery.
Practical Recommendations from ChiroMed for El Paso
Here are easy ways to apply the advice:
- Start days with fruit salads or smoothies featuring watermelon and berries.
- Snack on nuts or bananas for quick mineral boosts.
- Use peppermint tea for a cooling sensation.
- Add small amounts of cinnamon or cardamom to aid digestion without heat.
- Carry electrolyte drinks during outdoor time.
Supplements like magnesium, vitamin C, and omega-3s can help reduce heat-induced inflammation. Food comes first, with supplements as support.
How ChiroMed’s Integrative Chiropractic Supports Heat Management
Chiropractic care at ChiroMed supports the autonomic nervous system, which regulates sweating and temperature responses. Spinal adjustments improve nerve signals for better adaptation to heat. They also help maintain spinal disc hydration, which dry air can reduce, thereby reducing stiffness and discomfort.
Improved circulation from care moves heat away from the body’s core more efficiently. It lowers stress, which makes heat harder to handle, and promotes relaxation for better rest on warm nights. Adjustments remove nerve blocks so the body copes with temperature changes with less effort.
Insights from Dr. Alex Jimenez at ChiroMed
Dr. Alex Jimenez, DC, APRN, FNP-BC, leads ChiroMed with dual expertise in chiropractic and family practice. His integrative approach combines adjustments, nutrition, and functional medicine for personalized care. In El Paso, he sees patients improve mobility, energy, and heat tolerance when they follow hydration and mineral plans alongside spinal care.
Dr. Jimenez notes that spinal alignment helps the nervous system respond to environmental stresses like desert heat. His methods address root causes for lasting wellness in challenging climates (ChiroMed, n.d.).
Extra Tips for Summer Comfort in El Paso
- Begin with water-rich breakfasts to set a good start.
- Plan snacks every few hours to stay on the smaller meal track.
- Visit ChiroMed for regular adjustments to support nervous system health.
- Watch for signs of dehydration, such as dark urine or dizziness.
- Combine nutrition counseling with chiropractic for complete support.
These habits build on ChiroMed’s holistic methods.
Choose ChiroMed for El Paso Heat Wellness
El Paso’s dry desert heat need not limit your days. The 3-part nutrition system with water-rich foods, electrolytes, and light meals meets your body’s needs. Supplements fill gaps, and ChiroMed’s integrative chiropractic optimizes how everything works together. Under Dr. Alex Jimenez’s guidance, this combined plan helps locals stay active and comfortable.
Visit ChiroMed Integrated Medicine in El Paso for personalized care that fits the desert climate. Focus on smart food choices, targeted support, and expert adjustments for better health all summer long.
References
ChiroMed. (n.d.). ChiroMed – Integrated Medicine Holistic Healthcare in El Paso, TX. https://chiromed.com/
Drinksote. (n.d.). Best electrolytes for hot weather: Complete guide to summer hydration and heat illness prevention. https://drinksote.com/blogs/blog/best-electrolytes-for-hot-weather-complete-guide-to-summer-hydration-and-heat-illness-prevention
Jefferson Health. (n.d.). 5 hydrating foods to help you beat the summer heat. https://www.jeffersonhealth.org/your-health/living-well/5-hydrating-foods-to-help-you-beat-the-summer-heat
Kaiser Permanente. (n.d.). How to stay cool in the heat: 6 foods that can help. https://healthy.kaiserpermanente.org/health-wellness/healtharticle.6-foods-keep-cool
Makers Nutrition. (2022, June 20). Summertime supplements: Vitamins your customers need as the heat approaches. https://www.makersnutrition.com/news/2022-06-20-summertime-supplements-vitamins-your-customers-need-as-the-heat-approaches
Physical Dimensions Integrative Health Group. (2024, May 29). Summer supplements. https://www.physicaldimensionsihg.com/post/summer-supplements
Washington Post. (2023, July 13). What to eat during a heat wave. https://www.washingtonpost.com/climate-solutions/2023/07/13/what-to-eat-during-heat-wave/