Bioidentical HRT Overview With Integrative Endocrinology
Uncover the role of bioidentical HRT and integrative endocrinology in achieving optimal hormonal balance and vitality.
Abstract
In this post, I walk you through a clear, evidence-based path to understanding hormone optimization and why it is foundational to whole-body health, longevity, and disease prevention. We will explore the physiological roles of key hormones — including estrogen, testosterone, progesterone, thyroid hormones, and vitamin D — and how they influence the brain, heart, bones, metabolism, mood, and pain processing. I will define the difference between treating symptoms and healing root causes, explain the lock-and-key receptor model that distinguishes bioidentical hormones from their synthetic counterparts, and debunk common myths regarding cardiovascular risk and breast cancer. You will see how gut health and the gut-brain axis modulate hormone signaling, why “normal” lab values are not always “optimal,” and how integrative chiropractic care supports the nervous system and the hypothalamic-pituitary-adrenal axis to amplify therapeutic outcomes. Drawing from modern, peer-reviewed findings and my clinical experience, including outcomes documented across my care and education platforms, I present individualized treatment strategies — from transdermal therapy to pellet implantation — and explain exactly when, how, and why each approach is used.
Root-Cause Medicine vs Band-Aid Care: Why Healing Requires Asking “Why”
For decades, I have practiced with a simple guiding principle: “The greatest medicine of all is teaching people how not to need it.” That mindset demands distinguishing treating from healing.
- Treating means quieting a symptom while the underlying cause persists. Pain medication for a recurrent headache may silence the alarm without correcting dehydration, nutrient deficiencies, sleep debt, or stress physiology.
- Healing requires removing the cause so the body can restore balance — like finding the pebble in the shoe rather than numbing the toe. In hormone care, that pebble is often a deficiency, receptor insensitivity, or axis dysregulation that drives seemingly unrelated symptoms.
When patients arrive on antidepressants, anxiolytics, sleep aids, and stimulants, my position is straightforward: you are not deficient in Prozac or Xanax. Those symptoms are signals of deeper dysregulation. When we correct hormone signaling and support the body’s neuroendocrine and metabolic systems, patients don’t just feel less symptomatic — they recover function, resilience, and clarity. That is healing.
Bioidentical vs Synthetic Hormones: The Lock-and-Key Physiology
Cells communicate through precision. Hormones are keys; receptors are locks. The tighter the molecular fit, the richer the downstream signaling.
- Bioidentical hormones have the exact molecular structure your body produces. They fit receptors precisely, triggering entire cascades of gene transcription, enzyme activation, cellular energy production, and repair that extend far beyond stopping a hot flash or improving libido.
- Synthetic hormones are structurally altered analogs. They can wedge into the lock and quiet certain symptoms, but they do not reliably initiate the full spectrum of protective responses. Worse, they can “jam” the lock, producing off-target effects and risks seen in large trials of synthetic progestins and oral conjugated estrogens, including clotting and breast cancer risk signals that differ markedly from those associated with transdermal bioidentical estradiol and natural progesterone.
From a healing perspective, injured tissue resolves with nutrients, proper signaling, and innate intelligence — not force. Restoring the body’s native hormonal environment with bioidenticals aligns with physiology and reduces unintended consequences.
The Essential Hormone Suite: What Matters and Why
Hormones are a symphony, not soloists. The following players conduct everything from mitochondrial firing to synaptic plasticity:
- Testosterone: In both sexes, testosterone maintains muscle protein synthesis, mitochondrial density, dopamine tone, motivation, and vascular integrity. Clinically, optimizing testosterone often restores energy, drive, and emotional steadiness.
- Estrogen: Far beyond reproduction, estrogen modulates lipid profiles, vascular dilation, glucose handling, bone turnover, and neurotransmitter production. It interacts richly with serotonin, GABA, and acetylcholine circuits that govern clarity, memory, and mood stability.
- Progesterone: A natural neurosteroid and anxiolytic, progesterone supports sleep architecture via GABAergic pathways, balances the endometrium, reduces mast cell activation, and supports bone formation and neural repair.
- Vitamin D (as a secosteroid hormone): Through VDR signaling, vitamin D influences immune tolerance, autoimmunity risk, bone mineralization, muscle performance, and mood regulation. Receptor sensitivity and cellular uptake impact how other hormones exert their effects.
- Thyroid hormones (T4/T3): The master metronome of metabolism, thyroid hormones regulate mitochondrial biogenesis, thermogenesis, cholesterol clearance, GI motility, and brain speed. Many patients suffer “normal lab” hypothyroid symptoms due to conversion issues (T4 to T3), inflammation, or stress-axis suppression.
Every intervention we choose respects how these systems interlock.
Finding Hormonal Harmony- Video
When Hormones Drift: The Symptom Constellations I See Every Week
Hormone insufficiency can mimic anxiety disorders, hypothyroidism, chronic fatigue, and fibromyalgia. The pattern recognition is essential:
- In women:
- Emotional volatility with swings into irritability or sadness
- Central weight gain, fluid retention, unwanted hair changes
- Brain fog, slowed processing, decreased multitasking capacity
- Sleep fragmentation and poor restorative sleep
- In men:
- Loss of drive and diminished initiative
- Sarcopenia: shrinking limbs, growing midsection
- Irritability, anxiety, and flat mood
- Delayed recovery after exercise and joint aches
These are not signs of “aging we must accept.” They are flags of declining signal quality across neuroendocrine axes that can be corrected with targeted care.
Estrogen’s Systemic Power: Brain, Heart, Bone, and Beyond
Declining estradiol produces widespread changes:
- Brain and mood: Estrogen modulates serotonin synthesis and receptor sensitivity, supports synaptic density, and reduces neuroinflammation. Because ~80% of serotonin is produced in the gut, estradiol’s influence on mucosal integrity, motility, and microbiome ecology threads directly into mood.
- Cardiovascular protection: Estrogen raises HDL, improves endothelial function, and decreases atherogenic inflammatory signaling. Early postmenopausal initiation of estrogen therapy has been associated with profound reductions in cardiovascular events when personalized and appropriately delivered (see references).
- Bone remodeling: Estrogen reins in osteoclast activity and preserves trabecular architecture. After menopause, unopposed resorption accelerates — prompting bone loss and joint discomfort that often improves with physiologic replacement.
- Urogenital and GI systems: Estrogen maintains urogenital mucosal thickness, reduces susceptibility to UTIs, and supports oral health and the integrity of the colonic epithelium.
In men, a portion of testosterone’s benefits derive from conversion to estradiol via aromatase. Blocking that conversion can backfire — harming bones, vessels, and cognition.
Testosterone: Vital for Both Women and Men
A compelling endocrine fact: across a lifetime, women produce more testosterone than estrogen, yet female testosterone remains underappreciated. In my clinical work and in extensive training settings for medical providers, I find this knowledge gap consistent.
- Common deficiency signs in both sexes:
- Afternoon energy collapse (“2 to 4 PM crash”)
- Brain fog and distractibility
- Sarcopenia, increased fat mass
- Low mood, irritability, and anxiety
- Sleep maintenance challenges
- Decreased libido and diminished sense of well-being
The therapeutic aim is not masculinization for women. As Dr. Rebecca Glaser’s research shows, women thrive at levels in the low hundreds (e.g., 100–200 ng/dL), far below male optimization ranges, and nuisance effects (like faster hair growth) are manageable without inducing male traits (Glaser & Dimitrakakis, 2013).
Progesterone: The Great Balancer in Midlife
Progesterone is typically the first hormone to decline in perimenopause, creating estrogen dominance. Natural progesterone:
- Balances estrogen by protecting the endometrium and normalizing bleeding patterns
- Stabilizes sleep through GABA-A receptor modulation
- Calms anxiety by dampening excitatory stress signals
- Supports metabolism, helping counter central adiposity
- Builds bone by stimulating osteoblast activity
- Prevents migraines in hormonally sensitive cycles via neurovascular stability
I use oral bioidentical progesterone strategically at night to align with sleep physiology and reduce cortisol-driven restlessness.
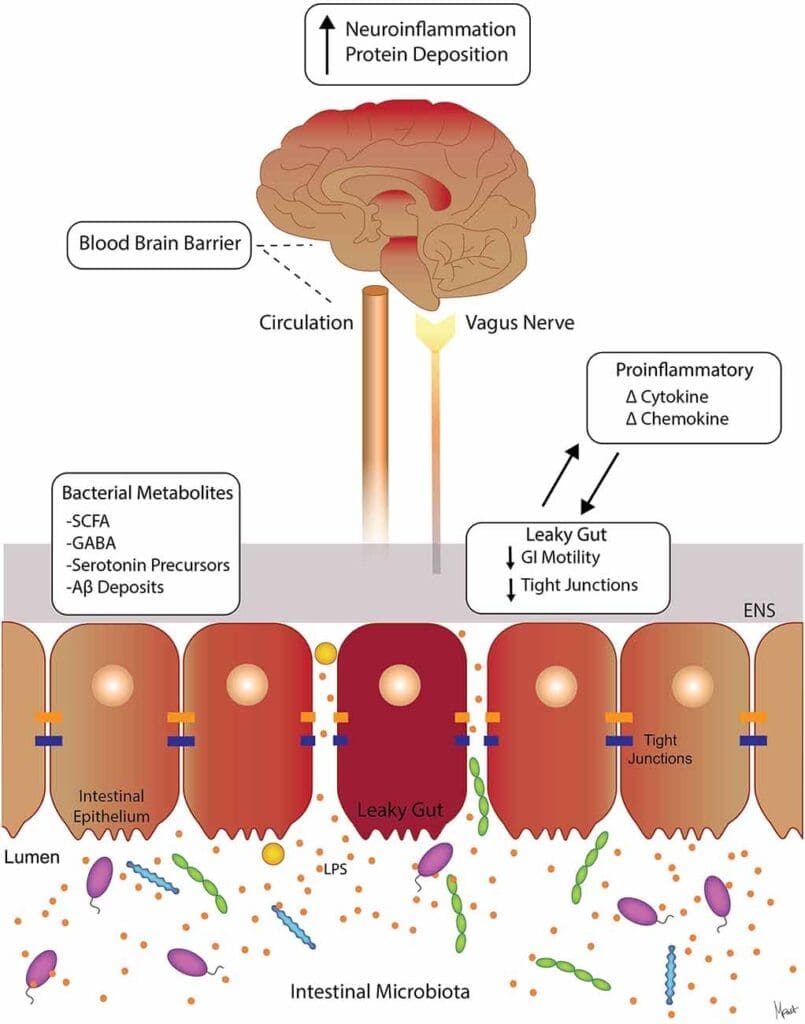
The Gut-Brain Axis: Why Digestion Shapes Hormone Signaling
The gut-brain axis provides a bidirectional highway between microbiome metabolism, mucosal immunity, and central nervous system function. When dysbiosis and leaky gut increase endotoxin exposure, the immune system escalates TNF-alpha and IL-6, which can:
- Suppress thyroid conversion (T4 to T3), slowing metabolism
- Interfere with steroid receptor sensitivity, blunting hormonal “volume.”
- Destabilize serotonin and GABA tone, worsening anxiety and insomnia
- Elevate cortisol, skewing glucose handling and fat distribution
Because hormones ride on the integrity of these networks, I routinely assess and address gut ecology — supporting barrier function, microbial balance, and nutrient repletion — to improve hormone outcomes.
Debunking Myths: Sex Hormones, Heart Disease, and Breast Cancer
Fear-mongering around hormones has caused avoidable suffering. Evidence clarifies:
- Heart disease reality: Cardiovascular disease causes far more deaths in women than breast cancer, especially after estradiol declines. Early, individualized estrogen therapy is associated with significantly reduced cardiac events when delivered as transdermal bioidentical estradiol and combined with natural progesterone if the uterus is intact (Manson et al., 2013; NAMS, 2017).
- WHI interpretation: The increased breast signal in the WHI was tied to synthetic progestin (medroxyprogesterone acetate), not natural progesterone. The Premarin-only arm showed reduced breast cancer incidence in some analyses; clotting risks were linked to oral administration, not transdermal routes. Modern, bioidentical protocols differ materially from those older findings.
- Testosterone’s cardiometabolic protection: Hundreds of studies support testosterone’s role in vascular health, insulin sensitivity, lipid balance, and mood. Some benefits reflect physiologic aromatization to estradiol. Routine estrogen blockade with testosterone therapy risks heart, bone, and brain health.
The narrative that “hormones cause breast cancer” is reductive. The real drivers include chronic inflammation, hyperinsulinemia, and toxic exposures. Optimizing hormones within a comprehensive anti-inflammatory and metabolic framework reduces the risk terrain.
Bone and Brain: Hormones as Structural and Cognitive Protectors
- Bone health: Estrogen and testosterone have synergistic effects — estrogen restrains resorption; testosterone promotes muscle strength and mechanotransduction, stimulating bone formation. Unlike some antiresorptives that create dense but brittle bone, physiologic hormone restoration improves bone quality, reducing fracture risk when combined with vitamin D, calcium, and resistance training.
- Brain health:
- Estrogen exhibits anti-inflammatory and immunomodulatory properties; the brain’s local synthesis of estradiol after injury reflects an innate neuroprotective strategy. Timed delivery of natural estradiol has shown dramatic post-ischemic benefits in experimental contexts.
- Testosterone supports memory, motivation, and synaptic stability; low levels correlate with depression, increased beta-amyloid deposition, cardiometabolic risk, and higher all-cause mortality.
- Pain processing: Both hormones modulate central and peripheral nociceptive pathways. In chronic pain, especially in the context of opioid use, testosterone drops precipitously, compounding pain sensitivity and slowing tissue repair. Optimizing sex hormones often reduces pain perception and accelerates recovery.
Treatment Modalities: How We Choose What to Use and Why
Personalized therapy means aligning the route, dose, and timing to your physiology and preferences.
- Oral bioidenticals:
- Progesterone at night synergizes with sleep architecture and GABAergic calming.
- Estradiol can be oral for some, but I prefer transdermal for clot risk mitigation.
- Sublingual testosterone is an option in select cases; we avoid oral synthetic testosterone due to liver and lipid concerns.
- Transdermal creams and patches:
- Estradiol patches deliver steady levels and circumvent first-pass hepatic metabolism, reducing clot risk and improving cardiovascular safety profiles.
- Creams can work well; absorption is increased in the genital dermis due to vascularity and a thin epithelium, thereby improving pharmacokinetics.
- Injections:
- Effective for testosterone but can cause peaks and troughs, increasing side effects.
- I avoid routine aromatase inhibitors because blocking estradiol harms joint, bone, heart, and brain health.
- Pellet therapy (bioidentical):
- Tiny implants placed in subcutaneous gluteal fat deliver steady, cardiac-output-modulated release for months.
- Advantages include consistency, convenience, and individualized dosing without weekly fluctuations.
- In my clinics, we have safely performed tens of thousands of pellet procedures, achieving robust outcomes in energy, mood, body composition, and relationships.
We select a route based on your clot risk, liver status, absorption patterns, lifestyle, and therapeutic goals, and we adjust iteratively with labs and symptom tracking to reach optimal — not merely normal — levels.
Integrative Chiropractic Care: Optimizing the Neuroendocrine Highway
As a DC and FNP, I integrate chiropractic care because the nervous system is the master regulator of the endocrine system. The spine houses the neural pathways that connect the hypothalamus, pituitary, adrenals, thyroid, gonads, and peripheral tissues.
- Neurological optimization: Spinal misalignments (subluxations) can impede afferent and efferent signaling, disrupting the feedback loops that maintain hormonal balance. Targeted adjustments restore neural conduction and autonomic tone, improving endocrine responsiveness.
- Stress physiology: Adjustments help downregulate sympathetic overdrive and normalize HPA-axis function, lowering chronic cortisol elevations that suppress thyroid conversion, disrupt sex hormone balance, and promote visceral adiposity.
- Whole-system synergy: I assess posture, biomechanics, and neural patterns alongside labs and symptoms. When the “power is on,” hormonal signals transmit efficiently — enhancing the impact of bioidentical therapy, gut repair, and nutrient protocols.
This integrative model accelerates outcomes and deepens durability.
Clinical Observations: Real-World Outcomes and Why They Matter
- “Gas in the tank” but no ignition: An 18-year-old with high-normal testosterone (~1,000 ng/dL) presented with depression, anxiety, and poor focus. The issue was not production; it was receptor sensitivity. By supporting vitamin D (for VDR and steroid receptor modulation), iodine (for thyroid support), and methylated B vitamins (for methylation and neurotransmitter pathways), his symptoms resolved rapidly. He discontinued psychiatric medications and regained function. This underscores that hormones require cofactors and competent receptors to work.
- “Getting her life back at 65”: After synthetic hormones were stopped at age 60 per outdated rules, a patient developed severe depression and withdrawal. Bioidentical pellet therapy restored estradiol, progesterone, and testosterone, and she experienced profound mood and relationship recovery. Her story is emblematic of the shift away from “lowest dose for shortest time” toward individualized, evidence-based longevity care (NAMS, 2017).
My clinical platforms consistently document these transformations across energy, cognition, mood, pain, and relationships, validating the integrated approach.
Why “Normal” Is Not Always “Optimal”
Population-based reference ranges reflect averages — not targets for vitality. Example: a vitamin D level of 35 ng/mL may be “normal,” yet evidence aligns disease prevention and immune optimization with levels typically above 60 ng/mL when individualized and monitored. Similarly, thyroid and testosterone “normalcies” might leave patients foggy, unmotivated, and fatigued.
- We test, treat, and retest — using symptom resolution, functional metrics, and lab optimization to find your personalized sweet spot.
- The goal is not “not sick.” The goal is vibrant.
Putting It All Together: A Practical, Personalized Pathway
Every plan is individualized, but the strategy follows clear physiology:
- Assess and align:
- Detailed history of symptoms, stress, sleep, nutrition, and gut health
- Comprehensive labs: sex hormones, thyroid panel (with free T3), vitamin D, metabolic markers, inflammatory cytokines as indicated
- Chiropractic examination: posture, segmental dysfunction, autonomic balance
- Intervene with precision:
- Bioidentical hormones via optimal route (transdermal, pellets, oral progesterone)
- Gut repair: barrier support, microbiome rebalance, anti-inflammatory nutrition
- Nutrient repletion: vitamin D, omega-3s, magnesium, iodine, B-complex (methylated)
- Chiropractic adjustments to normalize neural signaling and HPA-axis tone
- Lifestyle programming: resistance training for bone and insulin sensitivity, sleep optimization for hormone rhythm, stress practices for cortisol control
- Monitor and refine:
- Follow-up labs and symptom maps
- Dose adjustments to maintain physiologic ranges and minimize side effects
- Ongoing education so you understand the “why” behind each change
This is how we move from treating to healing.
Key Takeaways For Your Health Journey
- Hormone imbalances can occur at any age, affecting mood, energy, muscle function, cognition, and relationships.
- Bioidentical hormones fit receptor locks precisely, unlocking protective cascades in brain, heart, bone, and metabolism.
- Transdermal estradiol and natural progesterone differ materially from older synthetic regimens, shifting risk profiles and outcomes.
- Testosterone is vital for women and men; blocking estrogen in men is typically harmful.
- Gut health and the nervous system set the stage for hormone signaling; repair and alignment amplify results.
- Normal is not optimal; personalization is essential for long-term vitality.
- Integrative chiropractic care enhances neuroendocrine transmission and stress-axis regulation, increasing the efficacy of hormone therapy.
You do not have to live in a fog of fatigue, irritability, and disconnection. With modern, evidence-based, integrative care, you can reclaim clarity, purpose, and a vibrant life.
References
- Menopausal hormone therapy and health outcomes during the intervention and extended poststopping phases of the Women’s Health Initiative randomized trials (Manson, J. E., Chlebowski, R. T., Stefanick, M. L., Aragaki, A. K., Rossouw, J. E., Prentice, R. L., … & Wactawski-Wende, J., 2013). JAMA, 310(13), 1353–1368.
- The 2017 hormone therapy position statement of The North American Menopause Society (The NAMS 2017 Hormone Therapy Position Statement Advisory Panel, 2017). Menopause, 24(7), 728–753.
- Testosterone therapy in women: myths and misconceptions (Glaser, R., & Dimitrakakis, C., 2013). Maturitas, 76(3), 230–234.
SEO Tags: hormone optimization, bioidentical hormones, testosterone therapy for women, estrogen benefits, progesterone sleep support, thyroid optimization, vitamin D hormone, gut-brain axis, integrative chiropractic care, menopause therapy, andropause treatment, pellet hormone therapy, cardiovascular protection, osteoporosis prevention, brain health and hormones, functional medicine, Dr. Alexander Jimenez DC APRN FNP-BC IFMCP, El Paso hormone clinic