Chiropractic Care: A Complete Guide With Calisthenics
Learn the benefits of calisthenics and chiropractic care for athletes looking to improve performance and reduce injury risks.
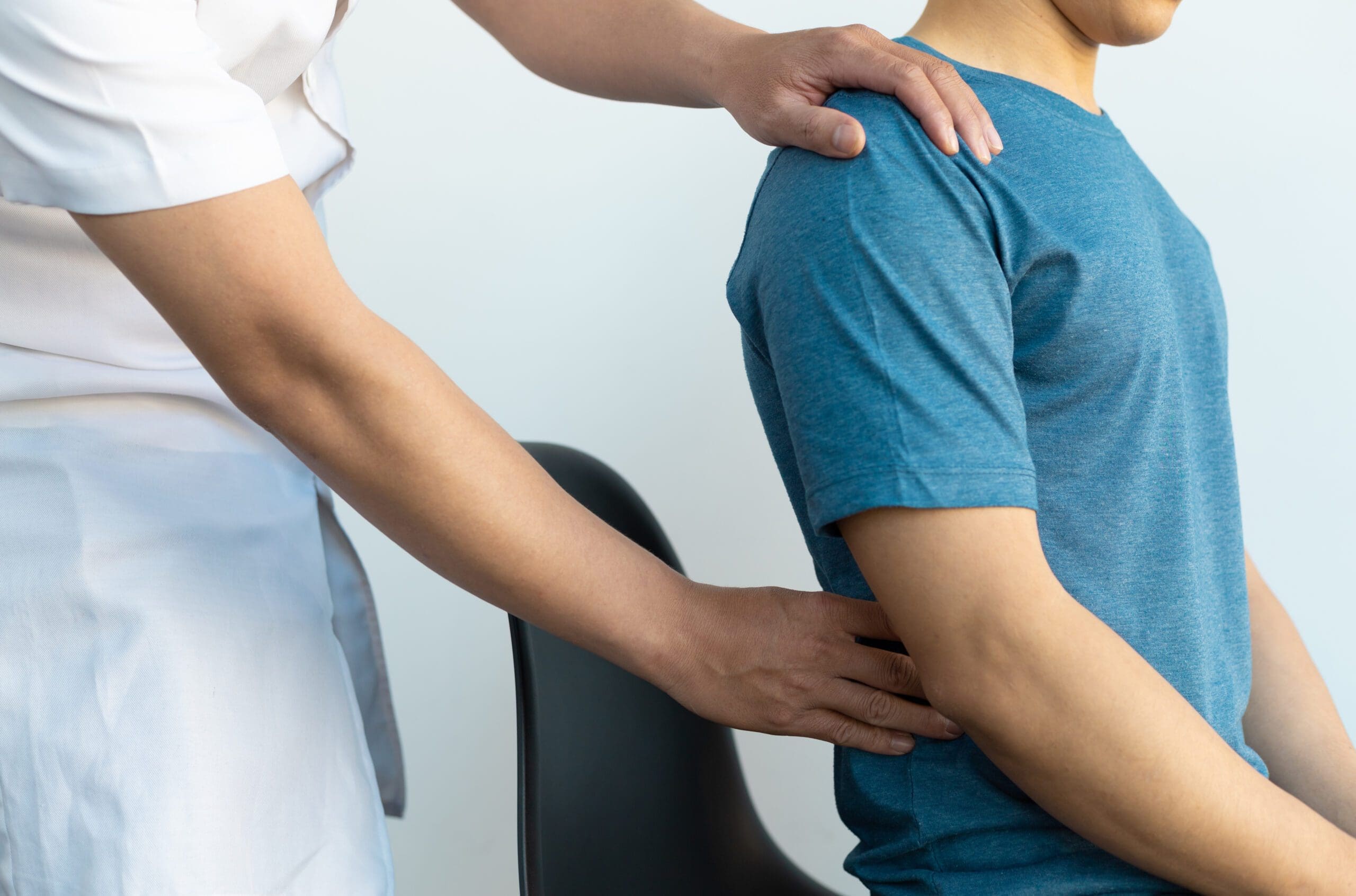
Chiropractic Care and Calisthenics: A Dynamic Duo for Musculoskeletal Pain Relief in El Paso
Musculoskeletal pain is a pesky problem that can turn your daily routine into a real pain in the neck—literally! Whether it’s a nagging backache, a stiff neck, or sore joints, this discomfort can stem from injuries, poor posture, or just sitting at a desk all day, dreaming of tacos. In El Paso, TX, ChiroMed – Integrated Medicine, led by the talented Dr. Alex Jimenez, DC, APRN, FNP-C, offers a game-changing solution by combining chiropractic care with calisthenics, a bodyweight exercise method with roots in ancient Greece. This blog post dives deep into why this combo is a powerhouse for reducing musculoskeletal pain and its overlapping risk factors, provides easy calisthenic exercises you can do anywhere, and highlights Dr. Jimenez’s expertise in personal injury cases. With a dash of humor to keep things light, let’s explore how you can kick pain to the curb and feel like a superhero in no time!
What Is Musculoskeletal Pain and Why Should You Care?
Musculoskeletal pain affects the muscles, bones, joints, ligaments, tendons, or nerves, making everyday tasks like lifting groceries or chasing your dog feel like an Olympic event. It’s a widespread issue, with chronic pain impacting millions and costing billions in healthcare and lost productivity (Gatchel et al., 2020). The causes are as varied as the toppings on an El Paso taco:
- Injuries: Sprains, strains, or trauma from car accidents, sports, or slipping on that sneaky patch of ice.
- Chronic Conditions: Think fibromyalgia, arthritis, or sciatica that just won’t quit.
- Lifestyle Habits: Hours of Netflix binging or slouching at a desk can wreak havoc on your spine.
- Stress and Anxiety: These can tighten muscles faster than you can say “deadline.”
These factors don’t just work alone—they team up like a gang of troublemakers, creating overlapping risk profiles that make pain worse. For example, sitting too long weakens your core, which messes with your posture, which then gets aggravated by stress-induced muscle tension. It’s like a bad sitcom rerun you can’t escape.
The good news? Chiropractic care and calisthenics can break this cycle. Chiropractic adjustments fix spinal misalignments and ease nerve pressure, while calisthenics strengthen muscles and boost mobility. Together, they tackle the root causes of pain and reduce risks like weak muscles, poor posture, and inflammation, helping you move better and feel better.
References
- Gatchel, R. J., Reuben, D. B., Dagenais, S., Turk, D. C., Chou, R., Hershey, A. D., … & Horn, S. D. (2020). Chronic musculoskeletal pain: Nonpharmacologic, noninvasive treatments. American Family Physician, 102(8), 465–472. Retrieved from https://pubmed.ncbi.nlm.nih.gov/33064420/
The Magic of Chiropractic Care
At ChiroMed – Integrated Medicine in El Paso, chiropractic care is the star of the show, and Dr. Alex Jimenez is the director. With over 20 years of experience since graduating from the University of Vermont in 1999, Dr. Jimenez blends chiropractic expertise with his skills as a family nurse practitioner to create personalized treatment plans that mix conventional and alternative medicine (ChiroMed – Integrated Medicine, n.d.).
How Does Chiropractic Care Help?
Chiropractic care focuses on fixing subluxations—misalignments in the spine or joints that irritate nerves, cause muscle tension, and limit movement. Through gentle spinal adjustments and manual therapy, chiropractors like Dr. Jimenez restore proper alignment, which is like hitting the reset button on your body’s control panel. This reduces pain, improves mobility, and helps your body function like a well-tuned machine.
Research backs this up big time. A systematic review found that combining manual therapy (like chiropractic adjustments) with exercise cuts pain and disability in people with nonspecific neck pain (Hidalgo et al., 2021). Here’s how chiropractic care tackles those overlapping risk factors:
- Posture Power-Up: Adjustments correct spinal alignment, reducing strain on muscles and joints.
- Mobility Boost: Restoring joint function makes it easier to move and exercise without wincing.
- Inflammation Tamer: Proper alignment can dial down inflammation, helping your body chill out.
Dr. Jimenez’s Role in Personal Injury Cases
El Paso’s vibrant lifestyle—think hiking, sports, and busy roads—means personal injury cases like car accidents, workplace mishaps, or sports injuries are all too common. Dr. Jimenez shines as a go-to practitioner for these cases, thanks to his dual expertise as a chiropractor and nurse practitioner. His approach is like a superhero team-up, combining:
- Advanced Imaging: Using X-rays, MRIs, or CT scans to spot injuries like herniated discs, whiplash, or soft tissue damage.
- Thorough Diagnostics: Detailed assessments to understand the full extent of injuries and their impact.
- Dual-Scope Care: Blending chiropractic adjustments with medical interventions like pain management or specialist referrals.
- Legal Liaison: Providing clear, detailed medical reports for insurance claims or legal cases, ensuring patients get the care and compensation they need.
For example, if you’re in a fender-bender and end up with neck pain, Dr. Jimenez might use an MRI to diagnose a cervical subluxation, perform adjustments to fix it, and document everything for your lawyer. His work at ChiroMed makes him a trusted ally for El Pasoans navigating the aftermath of injuries (Jimenez, n.d.).
References
- ChiroMed – Integrated Medicine. (n.d.). About us. Retrieved from https://chiromed.com/
- Hidalgo, B., Hall, T., Bossert, J., Dugeny, A., Cagnie, B., & Pitance, L. (2021). The combined effects of manual therapy and exercise on pain and related disability for individuals with nonspecific neck pain: A systematic review with meta-analysis. Journal of Manual & Manipulative Therapy, 29(5), 260–271. Retrieved from https://pubmed.ncbi.nlm.nih.gov/34472424/
- Jimenez, A. (n.d.). LinkedIn profile. Retrieved from https://www.linkedin.com/in/dralexjimenez/
Is Motion The Key To Healing- Video
Calisthenics: Your Body’s Gym, No Membership Required
Calisthenics, from the Greek words for “beauty” and “strength,” is like the workout version of a Swiss Army knife—versatile, effective, and equipment-free. As detailed by El Paso Back Clinic, this ancient Greek training method builds strength, flexibility, and endurance using just your bodyweight, making it perfect for anyone looking to get fit and pain-free (El Paso Back Clinic, n.d.).
Why Calisthenics Rocks
You don’t need a fancy gym or weights that cost more than your rent. Calisthenics uses your body as resistance, so you can work out in your living room, backyard, or even while waiting for your coffee to brew. It targets multiple muscle groups, improves coordination, and boosts functional movement, all of which help reduce musculoskeletal pain. Studies show that bodyweight exercises like calisthenics are effective for chronic low back pain, improving core stability and reducing fatigue (Gordon & Bloxham, 2021; Owen et al., 2020).
Here’s why calisthenics is the perfect partner for chiropractic care:
- Core Strength: A strong core supports your spine, reducing the risk of back pain.
- Posture Perfection: Exercises like planks help you stand tall instead of slouching like a tired scarecrow.
- Flexibility Gains: Movements like lunges stretch tight muscles, complementing chiropractic adjustments.
- Sedentary Slayer: Short bursts of calisthenics break up desk time, improving muscle function and reducing pain (Mace et al., 2022).
References
- El Paso Back Clinic. (n.d.). Calisthenics: The ancient Greek workout to get a shredded body. Retrieved from https://elpasobackclinic.com/calisthenics-the-ancient-greek-workout-to-get-a-shredded-body/
- Gordon, R., & Bloxham, S. (2021). Some types of exercise are more effective than others in people with chronic low back pain: A network meta-analysis. Journal of Physiotherapy, 67(4), 252–261. Retrieved from https://pubmed.ncbi.nlm.nih.gov/34580091/
- Mace, C., Kerse, N., Maddison, R., Olds, T., Jatrana, S., Wham, C., … & Rolleston, A. (2022). The effect of breaking up sedentary time with calisthenics on neuromuscular function: A preliminary study. International Journal of Environmental Research and Public Health, 19(3), 1452. Retrieved from https://pubmed.ncbi.nlm.nih.gov/35162460/
- Owen, P. J., Miller, C. T., Mundell, N. L., Verswijveren, S. J., Tagliaferri, S. D., Brisby, H., … & Belavy, D. L. (2020). Exercise therapy for chronic low back pain. Cochrane Database of Systematic Reviews, (9). Retrieved from https://pubmed.ncbi.nlm.nih.gov/32997745/
Five Calisthenic Exercises to Kick Pain to the Curb
Ready to get moving and tell pain to take a hike? Here are five beginner-friendly calisthenic exercises you can do at home or in a gym. They’re simple, effective, and require no gear—just your body and a bit of grit. (Note: Check with a pro like Dr. Jimenez before starting, especially if you have injuries or health conditions.)
1. Push-Ups (Chest, Shoulders, Core)
- How to Do It: Get into a plank position with hands shoulder-width apart. Lower your chest toward the floor, keeping your body straight, then push back up. No face-planting, please!
- Benefits: Builds upper body strength and core stability, reducing shoulder and neck pain.
- Beginner Hack: Try knee push-ups if the full version feels like armageddon. You’ll still feel like a champ.
2. Bodyweight Squats (Legs, Glutes, Core)
- How to Do It: Stand with feet hip-width apart. Lower your hips like you’re sitting in an invisible chair, keeping your chest up and knees over toes. Stand back up.
- Benefits: Strengthens legs and glutes, supporting your lower back and improving posture.
- Humor Alert: Pretend you’re dodging a swarm of bees—squat low and fast!
3. Plank (Core, Back, Shoulders)
- How to Do It: Lie face down, then prop up on your forearms and toes, keeping your body straight like a board. Hold for 20–30 seconds or until you start dreaming of quitting.
- Benefits: Boosts core strength, stabilizes the spine, and helps prevent lower back pain.
- Beginner Tip: Start with 10-second holds. You’re not trying to break a world record… yet.
4. Lunges (Legs, Glutes, Core)
- How to Do It: Step forward with one leg, lowering your back knee toward the ground. Keep your front knee over your ankle, then push back to start. Switch legs.
- Benefits: Improves leg strength, balance, and hip flexibility, easing lower back strain.
- Humor Alert: Imagine you’re lunging to grab the last slice of pizza—motivation matters!
5. Superman Hold (Back, Glutes, Core)
- How to Do It: Lie face-down, arms extended overhead. Lift your arms, chest, and legs off the ground like you’re flying. Hold for 5–10 seconds, then lower.
- Benefits: Strengthens your back and glutes, counteracting slouching and reducing back pain.
- Beginner Tip: Lift just your arms or legs if the full move feels like you’re auditioning for a Marvel movie.
Sample 15-Minute Routine
Do this circuit 3–4 times a week:
- Push-Ups: 10–15 reps
- Bodyweight Squats: 15–20 reps
- Plank: 20–30 seconds
- Lunges: 10 reps per leg
- Superman Hold: 5 reps (10 seconds each)
Pair this with chiropractic visits to ChiroMed for maximum results. Dr. Jimenez can check your form and tweak exercises to fit your needs, ensuring you’re not accidentally turning your workout into a comedy of errors.
Why Chiropractic Care and Calisthenics Are a Match Made in Heaven
Think of chiropractic care and calisthenics as peanut butter and jelly—they’re great on their own, but together, they’re unstoppable. Here’s how they team up to fight musculoskeletal pain and its pesky risk factors:
- Fixing the Foundation: Chiropractic adjustments correct spinal and joint misalignments, setting the stage for effective exercise by reducing nerve irritation.
- Building Strength: Calisthenics strengthens muscles, reinforcing the benefits of adjustments by stabilizing your spine and joints.
- Pain Relief Powerhouse: Studies show that combining manual therapy with exercise is more effective than either alone for reducing pain and disability (Hidalgo et al., 2021).
- Better Movement Control: Calisthenics improves neuromuscular stability, helping you move better and avoid re-injury (McCaskey et al., 2022).
- Mental Health Bonus: Calisthenics can reduce stress and fatigue, which often worsen pain, making you feel as zen as a sunny El Paso afternoon (Niedermeier et al., 2021).
At ChiroMed, Dr. Jimenez crafts plans that blend these approaches. For instance, a patient with chronic back pain might get spinal adjustments to fix misalignments, followed by a calisthenics routine to strengthen their core, ensuring long-term relief and resilience.
References
- Hidalgo, B., Hall, T., Bossert, J., Dugeny, A., Cagnie, B., & Pitance, L. (2021). The combined effects of manual therapy and exercise on pain and related disability for individuals with nonspecific neck pain: A systematic review with meta-analysis. Journal of Manual & Manipulative Therapy, 29(5), 260–271. Retrieved from https://pubmed.ncbi.nlm.nih.gov/34472424/
- McCaskey, M. A., Wirth, B., & Balagué, F. (2022). The role of neuromuscular control of postural and core stability in functional movement and athlete performance. Frontiers in Physiology, 13, 796097. Retrieved from https://pubmed.ncbi.nlm.nih.gov/35250609/
- Niedermeier, M., Fröhlich, K., Frühauf, A., & Kopp, M. (2021). Psychological effects of calisthenic exercises on neuroinflammatory and rheumatic diseases. Frontiers in Psychology, 12, 678075. Retrieved from https://pubmed.ncbi.nlm.nih.gov/34177728/
Personal Injury Care: Dr. Jimenez’s Expertise in El Paso
El Paso’s active vibe and busy streets mean personal injuries—like car crashes, workplace accidents, or sports mishaps—are part of life. Dr. Alex Jimenez at ChiroMed is a standout for these cases, thanks to his unique blend of chiropractic and medical expertise. His approach includes:
- High-Tech Diagnostics: Using MRI, X-ray, or CT scans to pinpoint injuries like herniated discs or soft tissue damage.
- Customized Treatment: Combining adjustments, rehabilitation, and calisthenics to restore function and ease pain.
- Legal Support: Providing detailed medical reports for insurance or legal claims, ensuring patients get fair treatment.
- Holistic Healing: Adding nutrition counseling, acupuncture, or naturopathy for complete recovery.
Imagine a patient with whiplash from a rear-end collision. Dr. Jimenez might use imaging to confirm a cervical issue, perform adjustments to restore alignment, and prescribe planks to strengthen neck muscles. His reports then help the patient’s lawyer build a strong case. This all-in-one approach makes Dr. Jimenez a vital resource for El Paso’s injury victims.
How to Add Chiropractic Care and Calisthenics to Your Life
Ready to ditch the pain and feel awesome? Here’s how to integrate chiropractic care and calisthenics into your routine, with a nod to Dr. Jimenez’s expertise:
- Get Checked Out: Visit ChiroMed for a full assessment. Dr. Jimenez will spot any issues and create a custom plan.
- Start with Adjustments: Regular chiropractic visits will fix misalignments and prep your body for exercise.
- Add Calisthenics: Try the exercises above, aiming for 2–3 sessions a week. Focus on form to avoid looking like a wobbly Jenga tower.
- Track Your Progress: Note changes in pain and mobility, and share them with Dr. Jimenez to fine-tune your plan.
- Tweak Your Lifestyle: Sit less, stand taller, and chill out to keep those risk factors at bay.
A Pinch of Humor
Think of calisthenics as your body’s way of saying, “I’m ready to be awesome!” and chiropractic care as the coach that gets you there. So, put down the remote, crank up some music, and move like nobody’s watching—your spine will thank you!
Conclusion
Musculoskeletal pain doesn’t have to run your life. By combining chiropractic care and calisthenics, you can tackle pain, improve function, and reduce overlapping risk factors like weak muscles, poor posture, and stress. At ChiroMed – Integrated Medicine in El Paso, Dr. Alex Jimenez, DC, APRN, FNP-C, offers personalized care that blends spinal adjustments with exercises like push-ups and planks, helping patients achieve lasting relief. His expertise in personal injury cases, backed by advanced imaging and legal support, makes him a trusted partner for El Pasoans seeking recovery and justice.
Disclaimer: This blog post is for informational purposes only and is not a substitute for professional medical advice. Always consult a qualified healthcare provider, such as Dr. Alex Jimenez at ChiroMed – Integrated Medicine, before starting any exercise or treatment program. For personalized care, contact ChiroMed at +1 (915) 412-6680 or [email protected].
References
- ChiroMed – Integrated Medicine. (n.d.). About us. Retrieved from https://chiromed.com/
- El Paso Back Clinic. (n.d.). Calisthenics: The ancient Greek workout to get a shredded body. Retrieved from https://elpasobackclinic.com/calisthenics-the-ancient-greek-workout-to-get-a-shredded-body/
- Gatchel, R. J., Reuben, D. B., Dagenais, S., Turk, D. C., Chou, R., Hershey, A. D., … & Horn, S. D. (2020). Chronic musculoskeletal pain: Nonpharmacologic, noninvasive treatments. American Family Physician, 102(8), 465–472. Retrieved from https://pubmed.ncbi.nlm.nih.gov/33064420/
- Hidalgo, B., Hall, T., Bossert, J., Dugeny, A., Cagnie, B., & Pitance, L. (2021). The combined effects of manual therapy and exercise on pain and related disability for individuals with nonspecific neck pain: A systematic review with meta-analysis. Journal of Manual & Manipulative Therapy, 29(5), 260–271. Retrieved from https://pubmed.ncbi.nlm.nih.gov/34472424/
- Jimenez, A. (n.d.). LinkedIn profile. Retrieved from https://www.linkedin.com/in/dralexjimenez/
- Gordon, R., & Bloxham, S. (2021). Some types of exercise are more effective than others in people with chronic low back pain: A network meta-analysis. Journal of Physiotherapy, 67(4), 252–261. Retrieved from https://pubmed.ncbi.nlm.nih.gov/34580091/
- Mace, C., Kerse, N., Maddison, R., Olds, T., Jatrana, S., Wham, C., … & Rolleston, A. (2022). The effect of breaking up sedentary time with calisthenics on neuromuscular function: A preliminary study. International Journal of Environmental Research and Public Health, 19(3), 1452. Retrieved from https://pubmed.ncbi.nlm.nih.gov/35162460/
- McCaskey, M. A., Wirth, B., & Balagué, F. (2022). The role of neuromuscular control of postural and core stability in functional movement and athlete performance. Frontiers in Physiology, 13, 796097. Retrieved from https://pubmed.ncbi.nlm.nih.gov/35250609/
- Niedermeier, M., Fröhlich, K., Frühauf, A., & Kopp, M. (2021). Psychological effects of calisthenic exercises on neuroinflammatory and rheumatic diseases. Frontiers in Psychology, 12, 678075. Retrieved from https://pubmed.ncbi.nlm.nih.gov/34177728/
- Owen, P. J., Miller, C. T., Mundell, N. L., Verswijveren, S. J., Tagliaferri, S. D., Brisby, H., … & Belavy, D. L. (2020). Exercise therapy for chronic low back pain. Cochrane Database of Systematic Reviews, (9). Retrieved from https://pubmed.ncbi.nlm.nih.gov/32997745/