Chiropractic Shockwave Therapy for Pain and Healing
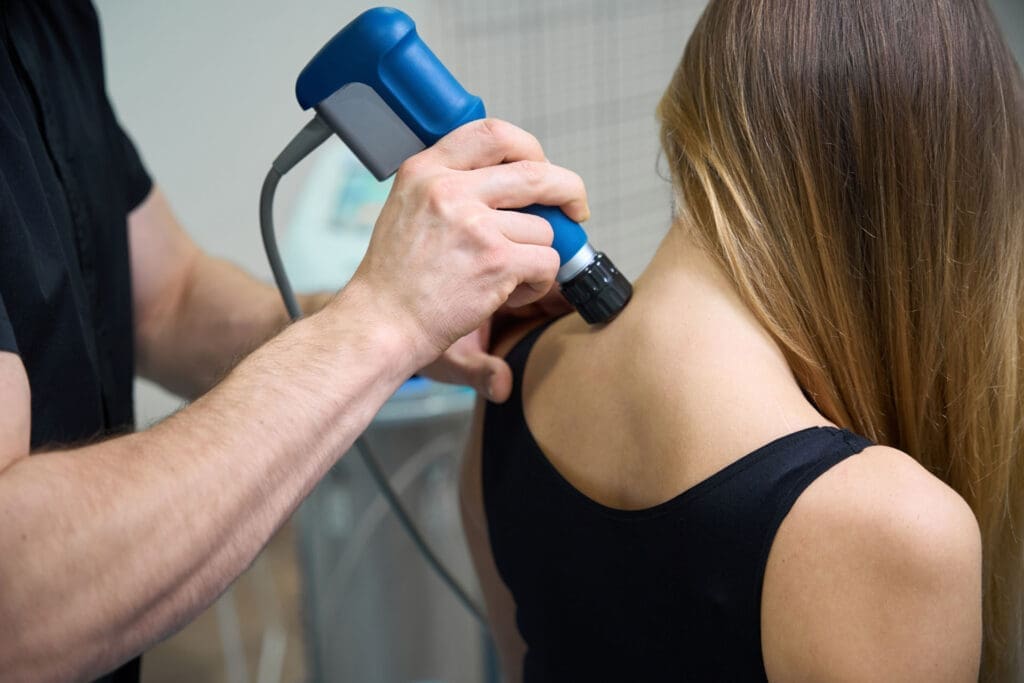
Radial vs. Focused Approaches, Physiological Mechanisms, Clinical Protocols, and Practical Considerations
Abstract
In this educational post, I share a clear, first-person overview of how shockwave therapy integrates into evidence-based chiropractic and advanced practice nursing care, explaining the differences between radial and focused shockwave systems, the underlying regenerative physiology, and how these modalities can be combined to optimize patient outcomes. I discuss FDA status, indications, dosing paradigms, and treatment sequencing for conditions such as tennis elbow, plantar fasciitis, whiplash-associated neck pain, and broader myofascial pain syndromes. I also outline practical details on device maintenance, session duration, patient experience, and cash-pay considerations, all framed within modern clinical research methods. Finally, I demonstrate how integrative chiropractic care, functional medicine, and rehabilitative protocols complement shockwave therapy to accelerate healing and restore function, supported by current literature and clinical observations from my practice.
Introduction: My Integrative Lens on Shockwave Care
As Dr. Alexander Jimenez, DC, APRN, FNP-BC, CFMP, IFMCP, ATN, CCST, I approach musculoskeletal care through an integrative model that blends chiropractic medicine, advanced practice nursing, functional medicine, and rehabilitative sciences. In recent years, I have incorporated acoustic shockwave technologies to complement manual therapy, neuromuscular re-education, and metabolic optimization. The clinical question patients and colleagues often ask is simple: how do these devices work, which type is appropriate, and how do we combine them within a patient-centered care plan?
In this post, I take you through a straightforward journey:
- What shockwave therapy is and how it differs between radial and focused systems
- The physiological basis of tissue regeneration triggered by acoustic waves
- Why combining radial and focused treatments can produce synergistic results
- FDA status, indications, session parameters, and maintenance
- Evidence-based protocols and how we titrate energy levels using real-time patient feedback
- How integrative chiropractic care and functional medicine enhance outcomes
- Practical notes on reimbursement, patient materials, and clinical communication
Throughout, I reference contemporary literature and share clinical observations from my practice, highlighting the care pathways we use at ChiroMed and those we use in collaboration with broader interdisciplinary networks.
Shockwave Therapy Basics: What It Is and Why It Matters
Shockwave therapy delivers high-pressure acoustic waves into target tissues to stimulate the body’s innate regenerative and anti-inflammatory mechanisms. The field evolved from lithotripsy, originally used to break kidney stones. Clinicians then noticed surrounding soft tissues exhibited improved quality post-treatment, spurring research into orthopedic and sports applications.
Key distinctions:
- Radial shockwave disperses energy from the skin surface and fans out through the tissue to a depth of roughly 6 cm, favoring superficial tendons and large muscle groups.
- Focused shockwave converges energy at a precise focal point up to ~12.5 cm deep, ideal for tendons, bone, ligaments, and deep joint pain.
These mechanical stimuli produce controlled microtrauma, which is central to the therapeutic cascade. Rather than damaging tissues, the microtrauma acts as a signal—prompting targeted neovascularization, growth factor upregulation, and cellular recruitment necessary for remodeling and repair.
Radial vs. Focused Shockwave: Energy Distribution and Clinical Targeting
The difference between radial and focused shockwave lies in energy distribution:
- Radial: Highest energy at the skin; wavefront dissipates as it travels inward; broad field engagement of fascia and muscle.
- Focused: Energy converges at depth; highly pinpoint targeting of the primary pain generator or structural lesion.
In practice, I often layer these modalities in a single session:
- Use radial shockwave across affected myofascial chains (e.g., forearm flexors/extensors and biceps in lateral epicondylopathy) to reduce global tone, address trigger points, and improve tissue pliability.
- Follow with focused shockwave directly over the primary lesion (e.g., degenerative extensor tendon insertion at the lateral epicondyle) to catalyze tissue-specific healing responses.
This dual approach respects both the regional interdependence of musculoskeletal pain and the necessity of site-specific regenerative signaling.
Physiological Underpinnings: From Microtrauma to Regeneration
Why does controlled acoustic microtrauma work? The physiology unfolds across several interconnected domains:
- Mechanotransduction: Acoustic waves deform cellular membranes and extracellular matrix (ECM). Integrins, stretch-activated ion channels, and cytoskeletal elements transduce mechanical inputs into biochemical signals that regulate gene expression and protein synthesis (Wang, 2012).
- Neovascularization and angiogenesis: Shockwave stimulates vascular endothelial growth factor (VEGF), eNOS, and related pathways, increasing capillary density and improving perfusion to ischemic or chronically degenerated tissues (Hausdorf et al., 2011).
- Inflammatory modulation: Microtrauma induces a controlled acute-phase response, converting a chronic, low-grade inflammatory milieu into a time-limited acute state with organized repair—resetting stalled healing cycles typical of tendinopathies (Rompe et al., 2009).
- Fibroblast activation and collagen remodeling: Enhanced fibroblast activity and collagen turnover shift tissue architecture from disordered Type III collagen toward more aligned, load-bearing Type I collagen, improving tensile strength (Wang et al., 2003).
- Nociceptive effects: Shockwave may modulate pain via hyperstimulation analgesia, substance P depletion at sensory nerve endings, and activation of descending inhibitory pathways. Clinically, patients often report immediate analgesia and improved range of motion after a session—effects that partially recede within ~72 hours before consolidating with serial treatments (Notarnicola & Moretti, 2012).
- Stem/progenitor cell recruitment: Acoustic cues can enhance mesenchymal stromal cell migration and differentiation in preclinical models, supporting tendon-bone interface healing and cartilage support under specific dosing conditions (Chen et al., 2014). While human data are still evolving, these mechanisms inform dosing strategies.
In short, shockwave interrupts chronic pain physiology, converts it into an acute reparative state, and guides structural remodeling through repeat, appropriately titrated dosing.
Immediate Relief vs. Long-Term Remodeling: Setting Expectations
One hallmark of clinical shockwave is the rapid analgesic effect many patients feel upon standing after the session. Patients often say that the arm, heel, or neck “feels amazing” with improved range of motion. However, I emphasize that this is step one. Over the next ~72 hours, some symptoms transiently return. With each subsequent session, the recurrence is diminished, reflecting cumulative tissue regeneration and functional adaptation.
We schedule shockwave in series—common patterns include 4–6 sessions spaced 5–10 days apart, depending on indication, tissue response, and comorbidities. The objective isn’t merely pain reduction; it’s structural and functional restoration.
FDA Status and Clinical Indications
Understanding regulatory status helps us communicate clearly and ethically:
- Focused shockwave has FDA approval for chronic plantar fasciitis (e.g., ESWT/Focused ESWT devices).
- Radial shockwave systems have FDA clearance for the treatment of chronic and acute musculoskeletal pain.
In practice, I consider shockwave for:
- Plantar fasciitis/heel pain (focused primary; radial adjunct for calf/plantar fascia chain)
- Lateral epicondylopathy (focused at tendon insertion; radial over forearm muscle groups)
- Patellar tendinopathy and Achilles tendinopathy
- Gluteal and proximal hamstring tendinopathies
- Myofascial pain syndromes and trigger points
- Hip abductor complex, rotator cuff tendinopathy, and selected bony stress responses under proper guidance
- Neck pain and whiplash-associated disorders below the skull base—radial for global muscular tone; focused cautiously for deep facet/tendon interfaces when indicated
Note: Cranial applications remain contraindicated in the US at present, though ongoing investigational work in Europe is underway.
Session Design, Dosing, and Patient Experience
We aim for treatment sessions around 10 minutes when combining modalities:
- Radial shockwave: ~5 minutes, commonly 2,500–3,000 pulses per session
- Focused shockwave: ~5 minutes, with pulse counts adapted to the device and indication
The handpiece interfaces allow real-time pulse tracking, energy adjustments, and preset stops. I titrate energy using patient feedback to maintain a therapeutic sensation of roughly 5–6 out of 10—intense enough to engage the physiology, but not so strong as to provoke guarding or undue distress. Because shockwave is diagnostic in practice, I use palpable landmarks, ultrasound when appropriate, and patient-reported tenderness to find and follow the pain generators.
- Sound levels: Radial devices are louder (mini jackhammer sound), whereas focused devices are quieter. Modern systems have improved acoustic dampening relative to older platforms.
Safety and Contraindications
- Avoid treatment over active infection, malignancy, or open growth plates (pediatric considerations).
- Exercise caution over vascular or neural bundles, and in patients with coagulopathies or on anticoagulants.
- Cranial applications are not cleared in the US; limit upper cervical work to below the skull base.
- Dose conservatively in severe neuropathy or altered pain processing syndromes, titrating by feedback.
Device Maintenance and Practical Operations
For reliable performance, maintenance is straightforward:
- Radial shockwave: Replace the guide tube and bullet approximately every 1,000 treatments (~2 million pulses for the pair). Revision kits include two bullets and two guide tubes. Handpiece notifications prompt replacement; providers can perform an easy swap via video guidance or live support.
- Focused shockwave: Replace the coil after around 2 million pulses (~1,000 treatments). The handpiece is typically overnighted to service for same-day repair and return, with scheduling tips to minimize clinic downtime.
Applying Shockwave in Personal Injury and Neck Care
For whiplash-associated cases, I use an integrative protocol:
- Radial shockwave across hypertonic upper trapezius, levator scapulae, scalenes, and paraspinals below the skull base to normalize tone and reduce myofascial trigger points.
- Focused shockwave when indicated over facet capsule areas or tendinous insertions with precise dosing, guided by palpation and, when appropriate, ultrasound. This combination reduces guarding and prepares tissues for manual therapy and motor control retraining.
Integrative Chiropractic Care: Layering Modalities for Superior Outcomes
Shockwave is not a standalone cure—it is most powerful when integrated:
- Chiropractic adjustments: Once radial shockwave reduces guarding and focused shockwave modulates deep nociception, spinal and extremity adjustments can be delivered with less resistance and greater carryover.
- Neuromuscular re-education: I pair shockwave with targeted isometrics in early phases, then eccentric loading (e.g., Alfredson protocol variants) to align collagen fibers and reinforce tensile strength in tendons.
- Fascia-focused care: Post-shockwave, instrument-assisted soft-tissue mobilization or myofascial release can remodel ECM cross-links while perfusion is elevated.
- Functional medicine support: Optimize micronutrients (Vitamin C, collagen peptides, magnesium), sleep, glycemic control, and inflammation (addressing omega-3/6 balance) to support collagen synthesis and tissue repair. I monitor metabolic markers when needed for stubborn cases.
Clinical Observations from My Practice
In my clinics (see ChiroMed and my professional LinkedIn profile), I observe consistent patterns:
- Plantar fasciitis: Focused shockwave over the medial calcaneal attachment, with radial shockwave across the posterior chain (gastrocnemius/soleus and plantar fascia). Patients often report first-step pain reduced after session two, with functional gains consolidated by week 4–6.
- Lateral epicondylopathy: Radial shockwave to forearm compartments reduces tone; focused shockwave to the common extensor tendon origin accelerates pain resolution. I incorporate eccentric wrist-extensor exercises and ergonomic coaching to achieve sustained outcomes.
- Cervical myofascial pain: Radial shockwave to the upper quarter reduces headaches and neck stiffness, especially when combined with scapular stabilization and cervical motor control drills.
- Achilles tendinopathy: Dose-focused sessions at the midportion or insertion; radial shockwave reverberates across calf muscle fascia. Eccentrics and load management remain essential.
Patients report immediate relief, with a transient return of symptoms, followed by decreasing recurrence and improved tissue quality across a series. These patterns align with the known biology of shockwave-induced remodeling and the literature’s outcome curves.
Evidence-Based and Research Methods
Modern shockwave research spans randomized controlled trials, meta-analyses, and biomechanical studies. Core findings:
- Plantar fasciitis: Multiple RCTs support the superiority of focused ESWT over sham or conservative care for chronic cases, improving pain and function (Gerdesmeyer et al., 2008).
- Lateral epicondylopathy: ESWT demonstrates clinically meaningful pain reduction and improvements in grip strength, with particular benefit in chronic cases (Rompe et al., 2004).
- Tendinopathy biology: Mechanotransduction and angiogenic responses underlie the observed improvements (Wang, 2012), while studies show reductions in substance P and CGRP in tendon nociceptors, which explain rapid analgesia (Maier et al., 2003).
- Myofascial pain: Radial shockwave can reduce trigger point tenderness and improve functional measures compared to baseline (Cagnie et al., 2013).
Device technologies measure energy differently:
- Electromagnetic focused systems commonly report energy in millijoules per square millimeter (mJ/mm²), reflecting the energy density at the tissue interface.
- Electrohydraulic systems may report joules, which represent total burst energy, without the same normalized-area metric.
When interpreting literature, I align dosing models with energy density, frequency, and pulse counts, then correlate them with the clinical target and tolerance. This ensures translational fidelity from studies to practice.
Shockwave Protocol Design: Practical Steps
I standardize protocols while leaving room for individualized titration:
- Intake: Assess pain generators, regional interdependence, activity demands, comorbidities, and prior response to care.
- Planning:
- Radial shockwave: 2,500–3,000 pulses across related muscle and fascial chains; start lower energy and titrate to a 5–6/10 therapeutic sensation.
- Focused shockwave: Target lesion with energy density consistent with literature for the indication; adjust based on tenderness and tissue depth.
- Sequencing: Radial first to reduce tone; focused second to pinpoint the lesion.
- Integration: Post-session gentle ROM, hydration guidance, and, within 24–48 hours, begin isometric or eccentric loading routines.
- Series: Typically 4–6 sessions, each spaced by 5–10 days, with reevaluation after session 3 to confirm trajectory.
- Outcomes: Pain VAS, functional scales (e.g., VISA-A for Achilles), and objective ROM/strength assessments.
Reimbursement, Cash-Pay, and Patient Communication
Shockwave is often positioned as a cash-pay modality in the United States. While some providers explore coding pathways, my stance focuses on transparency and value:
- Present a clear series package (e.g., 4–6 sessions), with per-session rates typically between $250–$300, depending on the modality combination.
- Use patient education materials—brochures, website pages, and scripts—to explain mechanisms, timelines, and expected post-treatment sensations.
- Emphasize the functional ROI: fewer flare-ups, improved performance, reduced reliance on adjunct analgesics, and potential avoidance of more invasive interventions.
Patient Materials and Training
Comprehensive patient-facing content includes:
- What shockwave is
- Why we combine radial and focused treatments
- What they will feel during and after a session
- The importance of completing the series and participating in home exercise
- Safety points and post-care instructions
Team training ensures consistent dose titration, proper handpiece handling, maintenance, and confident communication with patients.
Clinical Pearl: The 72-Hour Window
I counsel patients that immediate relief is common, but some symptoms may re-emerge within ~72 hours as acute signaling fades and tissue repair continues. This is normal. Over subsequent sessions, they notice a stepwise reduction in recurrence. Setting this expectation enhances adherence and satisfaction.
Integrative Outcomes: Faster Rehabilitation, Better Function
Within my integrative framework, shockwave accelerates:
- Tissue readiness for manual therapy
- Engagement with therapeutic exercise
- Re-alignment of movement patterns
- Return to work and sport
Functional medicine supports the biologic terrain for collagen synthesis, capillary formation, and sleep-dependent repair. Over time, patients experience not just symptom relief, but durable biomechanical improvements.
Closing Thoughts
Shockwave therapy—when properly dosed, sequenced, and integrated—bridges the gap between immediate analgesia and long-term tissue regeneration. By combining radial and focused approaches, aligning with current research, and embedding care within chiropractic, rehabilitative, and functional frameworks, we achieve meaningful, measurable outcomes. In my practice, these technologies have become a reliable part of restoring movement and reducing chronic pain, provided we honor the physiology and respect the patient’s lived experience.
References
- Extracorporeal Shock Wave Therapy for Chronic Plantar Fasciitis: RCT Evidence (Gerdesmeyer, L., et al., 2008). The Lancet.
- Evidence-Based Use of ESWT in Tendinopathies (Rompe, J. D., et al., 2004). Knee Surgery, Sports Traumatology, Arthroscopy.
- Mechanotransduction and ESWT: Biological Mechanisms (Wang, C. J., 2012). International Orthopaedics.
- Angiogenic Effects of Shockwave in Soft Tissue (Hausdorf, J., et al., 2011). European Surgery.
- Shockwave Analgesia and Neuropeptide Modulation (Maier, M., et al., 2003). The American Journal of Sports Medicine.
- Radial ESWT for Myofascial Pain: Clinical Outcomes (Cagnie, B., et al., 2013). Manual Therapy.
- Tendon Collagen Remodeling Under ESWT (Wang, C. J., et al., 2003). The American Journal of Sports Medicine.
- ESWT in Chronic Tendinopathy: Clinical Pathways (Rompe, J. D., et al., 2009). Postgraduate Medical Journal.
Post Disclaimer
General Disclaimer, Licenses and Board Certifications *
Professional Scope of Practice *
The information herein on "Chiropractic Shockwave Therapy for Pain and Healing" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those on this site and on our family practice-based chiromed.com site, focusing on naturally restoring health for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and facilitate clinical collaboration with specialists across disciplines. Each specialist is governed by their professional scope of practice and licensure jurisdiction. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that are directly or indirectly related to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card
Licenses and Board Certifications:
DC: Doctor of Chiropractic
APRN: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card

