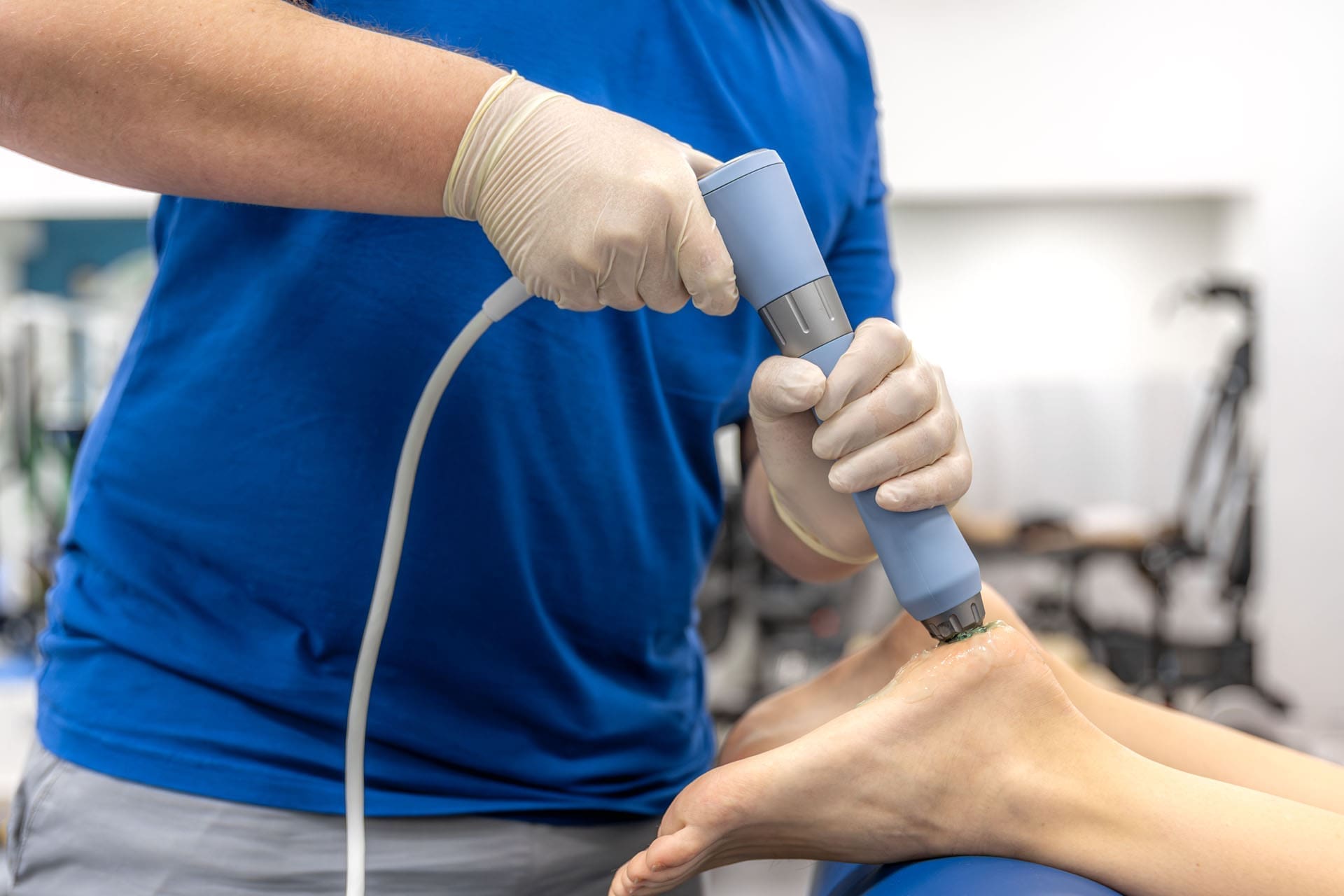
Integrative Care for Plantar Fasciitis With SoftWave
Abstract
In this educational post, I share my personal journey with severe plantar fasciitis and how SoftWave shockwave therapy transformed my recovery without injections or surgery. From there, we look at modern, evidence-based research on shockwave physics and mechanisms, compare true shockwave and radial pressure-wave devices, and explore patient outcome data from independent registries. I then outline how integrative chiropractic care fits into this model, including spinal and regional joint mechanics, fascial and neuromuscular coordination, anti-inflammatory nutrition, and return-to-sport protocols. You will learn why electrohydraulic shockwave is considered a gold standard, how it triggers angiogenesis and modulates inflammation, and how to implement it alongside biologics such as PRP in a clinically rational way. Throughout, I incorporate clinical observations from my practice to demonstrate real-world application and patient-centered workflows.
Why This Matters
I am Dr. Alexander Jimenez, DC, APRN, FNP-BC, CFMP, IFMCP, ATN, CCST. My clinical focus integrates chiropractic medicine, advanced practice nursing, functional medicine, sports science, and tissue rehabilitation. My mission is simple: deliver safe, effective, and science-driven care that helps patients return to life and sport with better long-term outcomes.
For many of my patients, chronic musculoskeletal pain feels like a maze of temporary relief and recurrent setbacks. New technologies can promise a lot but deliver unevenly. My goal in this post is to clarify the science, present real data, and show how integrative chiropractic care and SoftWave shockwave therapy can be combined to create a precise, reproducible plan of action.
From Pain To Practical Solutions: A Patient’s Plantar Fasciitis Story
Seven years ago, while working long hours on their feet as a wedding planner, a patient developed bilateral plantar fasciitis—a stubborn, burning heel pain worsened by standing, walking, and push-off mechanics. The standard recommendation the patient received was cortisone injections, which can blunt pain but may impair soft tissue healing and carry a risk of plantar fascia rupture with repeated use. The patient declined and assumed they would have to live with the pain.
A colleague introduced the patient to SoftWave shockwave therapy. Their first session was intense—older protocols often sought to “treat into pain”—but they felt relief the same day. The pain recurred within a few days, and the patient moved on. Then, two months later, the patient woke up and realized they hadn’t felt heel pain for days. They hadn’t stretched, changed footwear, or altered workload. The pain was just… gone. They stayed pain-free for nearly four years before needing another series. That experience ignited a commitment to evidence-based regenerative technologies that work with the body’s repair systems rather than against them.
What Is A Shockwave? The Physics That Matter
When you hear “shockwave,” think of a high-speed acoustic energy wave traveling faster than the speed of sound through tissue. In medicine, the waveform and speed are crucial:
- True shockwave: A high-velocity acoustic wave that reaches supersonic speeds and produces a sharp pressure gradient at the leading edge. Electrohydraulic systems generate this wave inside the applicator and deliver it as a coherent, high-energy impulse.
- Radial pressure wave: A lower-velocity pressure wave that disperses energy superficially and primarily creates mechanical perturbations near the skin surface.
Key physiological effects of true shockwave:
- Cell membrane mechanotransduction: The rapid pressure shift causes a transient change in cell membrane permeability, initiating signaling cascades.
- Angiogenesis: Upregulation of pro-angiogenic factors (e.g., VEGF) stimulates the formation of both small and large vessels, improving perfusion to hypoxic or degenerated tissues.
- Inflammation modulation: Downregulation of NF-κB pathways and altered cytokine profiles can help shift chronic inflammatory states toward resolution.
- Tissue remodeling: Stimulation of tenocytes, fibroblasts, and osteoblasts enhances matrix turnover, collagen alignment, and bone healing.
- Analgesic neuromodulation: Changes in peripheral nociceptor sensitivity and local neuropeptide signaling can reduce pain over time without neurodestructive effects.
Why speed and waveform matter:
- The steep pressure gradient of a true shockwave produces a shearing force at the cell membrane, which initiates the biological cascade (mechanotransduction).
- Devices that produce sound waves that converge into a shockwave only outside the applicator may have a shorter effective burst and require precise targeting to avoid under- or overdosing tissue.
- Electrohydraulic devices generate a shockwave within the applicator, providing a consistent, therapeutic energy profile that can reach deeper targets (often cited as up to approximately 12 cm, depending on tissue, coupling, and parameters).
Electrohydraulic Versus Electromagnetic/Piezoelectric: Practical Differences
There are several ways to generate shockwaves:
- Electrohydraulic: Two electrodes create a spark in water, producing a cavitation bubble; the leading edge of the bubble is the shockwave. This is often considered a gold standard by clinical shockwave societies due to stable energy delivery and deeper penetration.
- Electromagnetic: A magnetic coil accelerates a membrane or projectile; a shockwave forms as sound waves converge.
- Piezoelectric: Arrays of crystals emit waves that focus and converge to create a shockwave in a focal zone.
Clinical implications:
- Electrohydraulic systems typically deliver a full-energy shockwave at the applicator exit, reducing the “gap” between the device and the therapeutic zone.
- Convergent systems (electromagnetic, piezoelectric) can be effective but may have narrow focal zones, shorter burst durations, and require meticulous targeting and tip selection.
- The patient experience can differ: a broader energy distribution tends to be more comfortable, enabling higher-dose delivery without anesthesia.
True Shockwave Versus Radial Pressure Waves: Mechanisms And Outcomes
It is common to see radial devices marketed under “shockwave” branding. Mechanistically, radial devices:
- Produce pressure waves at sub-shock speeds.
- Disperse energy superficially, relying on microtrauma to induce reactive hyperemia and local neurogenic effects.
- Can be uncomfortable, and their therapeutic depth is generally limited.
Where radial can be useful:
- Short-term pain relief in superficial soft tissue conditions.
- Adjunct to manual therapy for myofascial trigger points.
- Situations requiring cost-effective, quick, superficial treatment.
Limitations:
- The durability of results may degrade over months in chronic degenerative conditions, as suggested by independent patient-reported outcome data comparing radial and true shockwave approaches.
The Two-Wave Advantage: Focused And Broad Focus Delivery
With electrohydraulic systems, particularly those using parabolic reflectors, two effects can be achieved:
- Primary focused wave: Laser-pointer-like focal energy reaching deeper tissue targets.
- Broad focus column: Recovered energy from the expanding cavitation bubble is redistributed, creating a larger therapeutic zone.
Why this matters:
- A larger treatment volume can address complex pain generators that are regionally interdependent (e.g., plantar fascia, intrinsic foot muscles, tibialis posterior, and soleus).
- Faster treatment times due to broader coverage.
- Reduced technician dependency because biofeedback cues and broader zones make precision less brittle.
- Improved comfort, allowing higher energy without anesthesia.
Biofeedback: The Patient Guides The Map
One practical advantage of shockwave therapy is patient biofeedback during treatment:
- Healthy tissue feels like gentle tapping.
- Inflamed or damaged tissue feels sharply distinct, allowing clinicians to map hotspots and functional pain generators.
- This reduces guesswork and allows real-time tailoring of energy density, pulse number, and coverage.
Sports Medicine Use Case: Rapid Return-To-Play
Consider an athlete with an adductor strain. Typical recovery for moderate strains is often 6–10 weeks, depending on grade and reinjury risk. Athletes treated with true shockwave combined with integrative rehab can sometimes return in 3–4 weeks when:
- Deep perfusion is improved via angiogenesis and vasodilation.
- Pain is modulated without masking protective reflexes.
- Tissue remodeling is supported with eccentric loading, neuromuscular re-education, and fascia mobility during the subacute window.
Orthopedic Insights From Elite Sports
Orthopedic specialists serving NBA and NFL athletes frequently use shockwave for:
- Bone edema
- Slow-healing fractures
- Post-operative nonunion risk
- Soft tissue tendinopathies
These clinicians report greater patient tolerance with true shockwave devices that deliver comfortably, thereby allowing higher-energy dosing without anesthesia and consistent day-to-day clinic throughput. This aligns with the published literature demonstrating the utility of shockwaves in bone and tendon biology through angiogenesis and mechanotransductive signaling.
How Integrative Chiropractic Care Fits The Model
Shockwave therapy works best in an integrative framework that addresses mechanical, neurophysiological, metabolic, and behavioral dimensions. In my clinic, we approach musculoskeletal problems through the following pillars:
- Biomechanics and joint mechanics:
- Correct regional alignment: In plantar fasciitis, foot pronation, tibial internal rotation, and hip mechanics create downstream overload on the plantar fascia. Chiropractic adjustments to the subtalar joint, midfoot, and pelvis can redistribute load and normalize gait.
- Improve segmental mobility: Thoracolumbar stiffness can degrade shock absorption; lumbar-pelvic adjustments support kinetic chain efficiency.
- Fascial continuity and neuromuscular coordination:
- Fascia connects the foot to the calf, hamstrings, and the lower back via myofascial chains. SoftWave improves perfusion and tissue pliability, while chiropractic soft-tissue work promotes gliding and hydration of the fascial planes.
- Focused motor control drills retrain the intrinsic foot muscles, the tibialis posterior, and the hip abductors to prevent recurrence.
- Load management and graded exposure:
- Implement eccentric loading and isometric pain-modulating holds to enhance collagen remodeling in tendons under safe strain.
- Use return-to-sport progressions based on pain response, strength benchmarks, and functional testing (e.g., single-leg hop, Y-balance).
- Anti-inflammatory nutrition and recovery biology:
- Encourage omega-3 fatty acids, polyphenols (curcumin, quercetin), vitamin D, magnesium, and targeted collagen peptides to support connective tissue health.
- Address sleep architecture and stress modulation, which influence cytokine profiles and healing velocity.
- Footwear, orthotics, and surface management:
- Consider temporary orthotic support to unload the plantar fascia during high-volume training weeks.
- Optimize shoe geometry (heel-to-toe drop, midfoot stiffness) to improve force distribution.
Clinical Observations From My Practice
Across multiple musculoskeletal conditions, I observe:
- Immediate reductions in pain scores following shockwave, especially when combined with regional adjustments and fascial mobilization.
- Durability improves when patients receive structured motor retraining and metabolic support.
- In tendinopathies (patellar, Achilles, gluteal), pairing shockwave therapy with progressive eccentric loading and coaching on stride or jump mechanics yields superior outcomes compared with passive care alone.
- For bone edema and stress reactions, true shockwave paired with relative rest, calcium/vitamin D, and careful return-to-impact criteria often accelerates readiness while reducing reinjury risk.
True Shockwave And Biologics: Rational Combinations
Shockwave interacts with biologic therapies thoughtfully:
- Same-day approach:
- Use shockwave to reduce pain and increase perfusion; perform PRP or cellular biologic injection afterward. Patients often tolerate injections better due to the immediate analgesic effects.
- Pre-injection priming:
- Deliver shockwave 2–3 days prior to biologic injection to enhance vascularity and cellular signaling, potentially improving biologic distribution and response.
- Diagnostic reinforcement:
- Use shockwave biofeedback to identify pain generators with a witness present; document patient responses to localize pathology and justify targeted biologic therapy.
Why each protocol makes sense:
- Shockwave-induced vasodilation and angiogenic signaling can facilitate biologic dispersion and nutrient delivery.
- Modulation of inflammation reduces hostile cytokine environments that can degrade biologic efficacy.
- Analgesia without anesthesia preserves protective neuromuscular control, reducing the risk of overloading post-injection immediately.
Device Selection And Practical Considerations
If you are evaluating devices:
- Prioritize true shockwave generation with consistent energy delivery and sufficient depth.
- Evaluate energy distribution patterns: A broad focus column plus focus offers versatility for both diffuse and focal pathologies.
- Consider patient comfort: Devices that deliver higher energy comfortably improve compliance and throughput.
- Assess training and workflow: Systems that are biofeedback-guided and easy to delegate to trained staff can streamline care without compromising safety.
Clinic Workflow And Patient Experience
Shockwave sessions in my clinic typically last 10–15 minutes. We:
- Conduct a focused functional exam and pain provocation tests.
- Use biofeedback mapping to guide energy dosing.
- Immediately follow with manual therapy, chiropractic adjustments, and targeted exercises to lock in gains.
- Provide home care protocols: gentle mobility, isometric holds, footwear guidance, and nutrition.
- Track outcomes using PROMs (pain scales, LEFS, VISA-A for Achilles, etc.) to quantify progress and justify care plans.
Cost And Access
Shockwave therapy is often a cash-based service, though some regions and payers may offer limited reimbursement for specific indications. In my experience, patients value:
- Rapid relief
- Non-invasive approach
- Fewer injections
- Evidence-backed tools
Transparent pricing, clear expectations, and outcome tracking build trust and encourage adherence.
Use Cases: Plantar Fasciitis, Tendinopathy, And Bone Edema
- Plantar fasciitis:
- Address degenerative microtears and fibrosis with shockwave-induced angiogenesis and matrix remodeling.
- Integrate foot mechanics correction, calf flexibility, and eccentric loading.
- Typical plan: 3–6 sessions over 4–8 weeks, tailored by pain and function.
- Achilles and patellar tendinopathy:
- Target mid-substance degeneration and enthesis changes using focused energy.
- Pair with tempo-controlled eccentrics and isometric protocols (45–60 second holds for pain modulation).
- Bone edema and slow-healing fractures:
- Use shockwave to stimulate osteogenesis and microcirculation, while managing load and nutrition.
- Coordinate with imaging and orthopedic oversight for safe progression.
Physiological Underpinnings: Why These Techniques Work
- Mechanotransduction: Shockwave applies mechanical stress that cells convert into biochemical signals—a core regenerative cue in tendon and bone.
- Angiogenesis and perfusion: Chronic pain is often a story of oxygen debt. Improving microvascular flow restores the redox balance, supports ATP production, and accelerates matrix repair.
- Inflammation resolution: Many chronic conditions are stuck in an immune loop of low-grade inflammation. Shockwave can shift cytokine profiles toward resolution, enabling fibroblasts and tenocytes to remodel effectively.
- Neuromodulation: Pain reduction without nerve ablation allows normal motor learning and movement quality to return during rehab—a safer, smarter approach.
Implementation Roadmap For Clinicians
- Assess:
- Identify pain generators via functional testing and biofeedback mapping.
- Consider imaging for bone edema or complex tendinopathy.
- Plan:
- Select energy levels and pulse counts based on tissue depth and patient tolerance.
- Integrate chiropractic adjustments, manual therapy, and exercise on the day of.
- Deliver:
- Keep sessions short, progressive, and guided by patient feedback.
- Use a broad focus for regional complaints and focused energy for pinpoint lesions.
- Reinforce:
- Provide home protocols, nutrition plans, and sleep hygiene.
- Schedule follow-ups and measure outcomes with standardized scales.
- Combine when indicated:
- Coordinate with PRP or other biologics using same-day or pre-injection priming.
- Document responses to build a data-informed case, improving patient consent and expectations.
What Patients Feel And How We Adjust
- Early sessions may include transient soreness at hot spots; this is expected and short-lived.
- Most patients feel immediate lightness or reduced pain, making subsequent rehab easier.
- If discomfort increases, we adjust energy or coverage while maintaining therapeutic intent.
Safety And Contraindications
- Avoid direct application over malignancy, active infection, or open wounds.
- Caution with pregnancy over the abdomen/low back.
- Coordinate with cardiology for anticoagulated patients near deep vascular structures.
- For acute complete tendon ruptures, shockwave is not a substitute for surgical repair; we use it post-operatively when cleared.
A Real-World Example: Return-To-Sport Strategy
For a competitive court-sport athlete with adductor strain:
- Week 0–1:
- Shockwave to the adductor complex and pelvic attachments.
- Chiropractic adjustments for pubic symphysis and sacroiliac joints.
- Isometric adductor holds, gentle mobility, and anti-inflammatory nutrition.
- Week 2–3:
- Progressive eccentric adductor loading and lateral movement drills.
- Continue shockwave as symptoms guide; expand coverage to hip flexors and gluteal stabilizers.
- Gait and stride mechanics corrections.
- Week 3–4:
- Introduce change-of-direction, acceleration/deceleration, and reactive drills.
- Clearance based on pain-free function, strength symmetry, and field tests.
In practice, this integrative plan frequently compresses recovery timelines while preserving tissue integrity.
Where To Learn More
For clinicians and patients interested in exploring shockwave research, professional societies and independent registries offer robust resources. You will find clinical guidelines, mechanisms, and outcome data across tendon, bone, and soft tissue conditions.
Training, Support, And Workflow Integration
Clinics that implement shockwave successfully typically:
- Receive hands-on training from experienced providers.
- Adopt biofeedback mapping in daily workflow.
- Leverage marketing assets to educate their community and referrers.
- Track PROMs and share outcomes in peer forums to refine protocols.
Closing Thoughts: Bringing Science, Skill, And Compassion Together
Patients with chronic pain taught me a simple truth: the body is eager to heal when given the right signals. SoftWave shockwave therapy delivers those signals powerfully and safely. When combined with integrative chiropractic care, targeted exercise, and smart biologics, the results are often transformative. Patients do not need to rely solely on injections or tolerate long downtimes. They need a coherent, evidence-informed plan that respects physiology, mechanics, and lived experience.
If you are struggling with chronic pain or you are a clinician looking for a better way, consider a thoughtful shockwave-based approach integrated with chiropractic biomechanics, fascia care, and functional medicine. It is not just about feeling better today—it is about building durable health for tomorrow.
References
- International Society for Medical Shockwave Treatment (ISMST): Clinical guidelines and resources (n.d.). Clinical guidance on shockwave mechanisms, indications, and safety.
- SoftWave Therapy: Research library and compendium (n.d.). Device-specific studies, international compendium, and clinical applications.
- ChiroMed: Clinical observations and integrative care insights by Dr. Alexander Jimenez (n.d.). Practice-based evidence and case-informed protocols.
- Dr. Alexander Jimenez, LinkedIn professional profile: Sports medicine and functional chiropractic integration (n.d.). Professional background and clinical updates.
Post Disclaimer
General Disclaimer, Licenses and Board Certifications *
Professional Scope of Practice *
The information herein on "Integrative Care for Plantar Fasciitis With SoftWave" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those on this site and on our family practice-based chiromed.com site, focusing on naturally restoring health for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and facilitate clinical collaboration with specialists across disciplines. Each specialist is governed by their professional scope of practice and licensure jurisdiction. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that are directly or indirectly related to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card
Licenses and Board Certifications:
DC: Doctor of Chiropractic
APRN: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card