Integrative MLS Laser for Back Pain and PRP Support
Abstract
This educational post explores how modern, evidence-based laser therapy protocols—specifically multi-wave locked system (MLS) laser therapy—are applied to common musculoskeletal problems like low back pain, facet joint-related stiffness, knee osteoarthritis, trigger points, and post-injection recovery. Presented in a first-person narrative by Dr. Alexander Jimenez, DC, APRN, FNP-BC, CFMP, IFMCP, ATN, CCST, it explains why prioritizing patient comfort, precise dosing via energy density, and multimodal targeting of connective tissues produce superior outcomes.
I detail how to set up robotic and handheld MLS laser delivery, calibrate dose using the X–Y field, and integrate laser therapy with integrative chiropractic care, orthobiologics (e.g., PRP), and metabolic optimization for mitochondrial health. I also clarify the distinction between acute and chronic protocols, the concept of energy density (4–10 J/cm²), pulse technology that protects tissues from thermal overload, and the clinical logic behind timing and sequence with PRP. Finally, I share clinical observations from my practice and insights from leading researchers using contemporary study designs, including randomized and controlled trials and consensus guidance, to ground recommendations in the current science.
Patient Comfort, Precision, and Workflow: Why Setup Matters
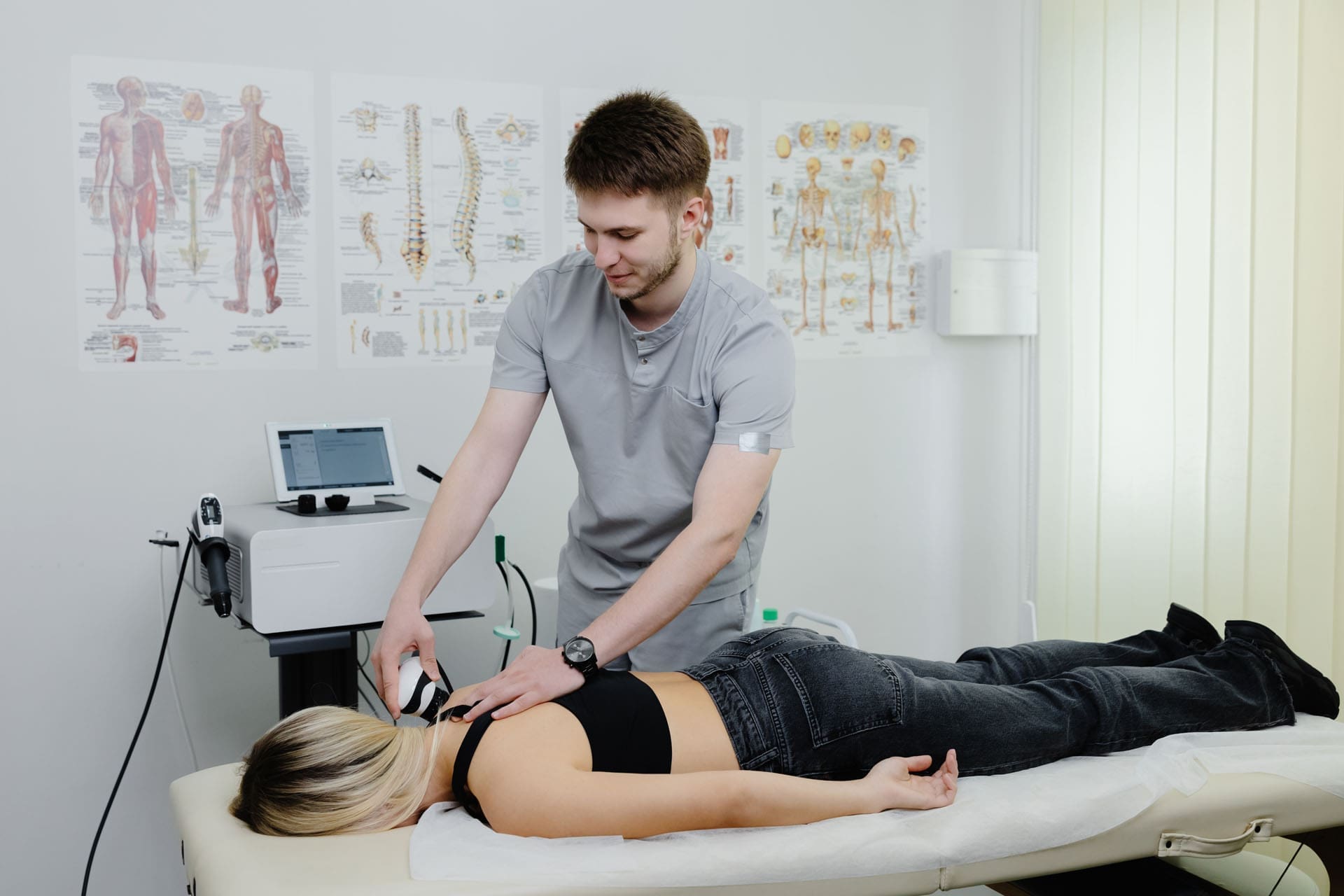
As a clinician, I have learned that successful laser therapy begins with one simple principle: patient comfort first. When I set up a robotic MLS laser for low back pain—especially in suspected facet joint dysfunction at L4–L5—I position the patient face down. The treatment window must be stable; if the patient shifts, I risk misalignment and uneven dosing. Maintaining a direct line of skin contact ensures accurate energy delivery and reproducible results.
- Key setup principles:
- Prioritize patient comfort to prevent movement and preserve targeting accuracy.
- Ensure direct-to-skin application for the handheld diode; the robotic headcan remains 5–7 inches off the skin due to its collimated beam and focal geometry.
- Calibrate the robot’s X and Y axes to center on the symptomatic site, then expand coverage to include both the primary lesion and surrounding connective tissues. This is what I call a clinical multimodal approach.
Why do I expand beyond the pain site? Because musculoskeletal pain rarely lives in isolation. Fascia, ligaments, and periarticular tissues function as a tensegrity network. When inflammation, nociceptive signaling, and muscular guarding spread through that network, addressing only the painful focal point misses upstream and downstream contributors. A global field—centered on the primary complaint and widened to nearby connective tissue—helps restore biomechanical harmony and promotes fluid exchange, mitochondrial efficiency, and neuromuscular balance. This approach aligns with modern integrative chiropractic care, in which spinal and soft-tissue adjustments, neuromuscular re-education, and laser therapy combine to reduce nociceptive signaling and optimize function.
Robotic vs. Handheld MLS Laser: Complementary Channels, Distinct Goals
In practice, I often employ both the robotic MLS laser and a handpiece simultaneously. Both are MLS devices, but they differ:
- Robotic head:
- Three diodes, a collimated beam with a focal distance of ~6 inches.
- Non-contact application is ideal for larger fields or when skin contact is contraindicated (post-surgical regions, fragile skin, or neuropathic sensitivity).
- Software-driven auto-recalibration: if I enlarge or shrink the X–Y treatment area, the device automatically adjusts treatment time to maintain the prescribed energy density.
- Handpiece:
- A single diode requires direct skin contact.
- Ideal for trigger points, narrow joint spaces, and dynamic application during guided movement.
- Short, focused exposures (e.g., 25 seconds per point) deliver precision dosing to the densest nociceptive clusters.
Using two separate channels allows me to run broader regional coverage with the robot while simultaneously desensitizing specific trigger points with the handpiece. This dual strategy is powerful in acute low back pain with facet involvement and for myofascial knots—what one analogy calls the “cooked meat” zones—firm, hypertonic bands within otherwise pliable “raw meat” muscle tissue. While the analogy is imperfect, patients recognize the feel instantly, and the focused pulse helps soften the local hypercontractile segment by modulating calcium handling, ATP availability, and nociceptive signaling in the immediate region.
Energy Density: The Dose That Drives Outcomes
Laser therapy is often misunderstood as a race to increase total energy (joules). In reality, the most clinically relevant parameter is energy density (J/cm²)—how much energy we deliver per unit area. For most musculoskeletal indications, the literature supports a target window of 4–10 J/cm². In my low back protocol, I typically choose ~6 J/cm² for facet-mediated stiffness.
- Why energy density matters:
- Achieves sufficient photobiomodulation to stimulate mitochondrial cytochrome c oxidase and downstream ATP production.
- Avoids the bioinhibition paradox (excess dose that suppresses cellular signaling) consistent with the Arndt–Schulz law, where too little dose yields no biological response, and too much can inhibit repair.
- Maintains consistent thermal equilibrium, so tissue temperature remains constant over time, which is a hallmark of properly dosed pulsed wavelengths.
Modern MLS systems use a combination of 808 nm (near-infrared, continuous or modulated) and 905 nm (super-pulsed) light. The 905 nm super-pulsed bursts allow very high peak power (e.g., 50 W) in extremely short pulses, minimizing surface heating while driving photons deeper. This “punch and rest” cycle provides tissues with time to absorb and distribute energy, preventing superficial thermal saturation and enabling deep-tissue photobiomodulation. If a patient feels excessive surface warmth, I re-evaluate the wavelength, dose, or settings to preserve the tissue’s thermal kinetics.
Visualizing the Treatment Field: Triangles, Wavelengths, and Practical Insight
Patients often enjoy seeing what’s happening in real time. Using a smartphone camera, the 808 nm wavelength is often visible as a triangle-shaped field on the skin. The 905 nm super-pulsed emission is generally invisible to smartphone cameras due to its pulse characteristics. Showing this helps the patient understand where energy is being delivered and why field geometry matters.
I calibrate the robot’s focal distance with a 6-inch ruler and adjust the X–Y coordinates until the triangle covers the target region and peripheral connective tissues. This geometry is more than aesthetics; it influences photon flux density and therefore the uniformity of cellular stimulation across the field. Small changes in field size cause the device to automatically recalculate the time required to maintain constant energy density, eliminating manual errors and ensuring dosing accuracy.
Acute and Chronic Protocols: Sequencing and Cumulative Effects
One of the most frequent clinical questions I receive is how many treatments are needed and how quickly results appear. Based on clinical experience and published guidance:
- Acute conditions:
- Aim for six treatments.
- Allow ~24 hours between sessions to allow tissue kinetics and cumulative photobiomodulation pathways to take effect.
- Common schedule: Monday/Wednesday/Friday for two consecutive weeks.
- Chronic conditions:
- Aim for 12 treatments, again with 24 hours between sessions.
- Patients often feel significant improvement after 3–5 sessions, but it is important to complete the series to realize the cumulative benefits of mitochondrial and inflammatory modulation. I recommend packaged care plans to encourage adherence and completion.
- Post-treatment time course:
- I counsel patients that 4–6 hours after an MLS session is often when the first significant changes are felt. If we treat at 11:00 AM, I ask them to reassess the function at around 5:00 PM that same day, performing their usual movement test to gauge the difference.
Knee Osteoarthritis: Field Geometry and Patellofemoral Considerations
For knee osteoarthritis (KOA), field geometry matters. Treating the anterior knee directly with the leg extended can reflect significant energy off the patella and anterior bony surfaces. I flex the knee to open the joint spaces and ensure that energy reaches the intra-articular and periarticular tissues. I also include posterior coverage to target the popliteal fossa, posterior capsule, and surrounding fascia.
- Clinical pearls:
- Use flexed positioning to reduce reflection and enhance penetration.
- Treat multiple compartments—medial, lateral, anterior (in flexion), and posterior—to ensure whole-joint coverage.
- Dose by energy density per compartment (e.g., ~6 J/cm²), rather than summing arbitrary total joules. The device will automatically calculate the total joules based on area and density.
Integrative chiropractic care is invaluable here—mobilizing the tibiofemoral and patellofemoral joints, freeing the IT band and lateral retinaculum, and reinforcing hip–knee kinetic chain alignment. Laser-induced reductions in synovial inflammation and nociception, combined with adjustments and neuromuscular re-education, reduce loading asymmetry and improve gait.
Bone Healing: Off-Label Insights and Early-Phase Targeting
While most of our discussion focuses on soft-tissue pathology, clinicians frequently ask about fractures. In my experience, there can be a meaningful benefit to bone healing when MLS therapy is applied early—within 7–10 days of injury—though such use is often considered off-label. Mechanistically, early-phase laser input supports angiogenesis, osteoblastic activity, and hematoma organization by stimulating mitochondrial signaling within the periosteal and soft-tissue envelopes surrounding the fracture. It is less effective for established nonunion, where the biological environment has already become chronically dysregulated.
- Practical considerations:
- Focus energy on the peri-fracture envelope where vascular and cellular activity is highest.
- Consider daily sessions in the acute inflammatory phase for the best impact.
- Integrate with orthopedic guidance and imaging to confirm progress.
Orthobiologics and PRP: Priming, Day-of, and Post-Injection Sequencing
Pairing MLS laser therapy with platelet-rich plasma (PRP) has become a promising strategy. The sequence matters.
- Pre-injection priming:
- 2–3 treatments in the two weeks preceding PRP prepare the microenvironment by enhancing local perfusion, lymphatic clearance, and mitochondrial readiness.
- This reduces local oxidative stress burden and improves cellular responsiveness to growth factors.
- Day of injection:
- A tailored MLS protocol is used to minimize trauma-induced nociception and to stabilize vascular responses without suppressing the beneficial pro-inflammatory phase of PRP. MLS is not an anti-inflammatory hammer; properly dosed pulsed emissions tend to modulate rather than abolish the necessary early signals.
- Post-injection build:
- Six treatments post-PRP help synchronize mitochondrial ATP supply, growth factor signaling, and matrix remodeling, thereby boosting clinical outcomes compared with PRP alone.
This sequencing mirrors the “prep the soil” concept—optimizing tissue to respond to biological seed inputs. Early data and clinical observations suggest that MLS + PRP can yield greater pain relief and functional improvements than PRP alone, by 15–20% in some series, though results vary based on tissue type, dosing fidelity, and patient-specific metabolic status (see References).
Mitochondrial Modulation: From Small Fiber Relief to Chronic Recovery
Patients and clinicians often ask: what changes first—pain relief, inflammatory control, or mitochondrial efficiency? In practice, these pathways overlap, but the temporal arc often looks like this:
- Immediate to early:
- Modulation of small myelinated fibers can quickly reduce pain and temperature sensitivity, aided by central pattern changes and gate-control influences.
- Rapid shifts in vasomotor tone improve local perfusion and wash out inflammatory mediators.
- Intermediate:
- Inflammatory and immune modulation refines cytokine balance (e.g., downregulation of TNF-α and IL-1β, upregulation of IL-10) and microglial reactivity at neuropathic interfaces.
- Redox balance improves as reactive oxygen species are buffered and mitochondrial enzymes are upregulated.
- Later/chronic:
- Mitochondrial biogenesis and enhanced ATP production elevate tissue repair capacity.
- Improvements in ECM remodeling, collagen crosslinking quality, and tendon/ligament fiber organization become clinically evident as strength and function return.
This is why finishing the treatment series matters. Early symptom relief can tempt patients to stop early. However, the deeper mitochondrial and matrix changes typically require completion of the protocol to lock in long-term functional gains.
Metabolic Optimization: CoQ10, Creatine, NAD, and Medication Considerations
MLS laser therapy does not occur in a metabolic vacuum. Many patients are on statins, metformin, and other medications that can influence mitochondrial function. In integrative practice, I frequently layer nutraceutical support when clinically appropriate and evidence-supported:
- CoQ10: replenishes electron transport chain cofactor depleted by statins, supports ATP production.
- Creatine: provides phosphate donation to regenerate ATP during high-demand phases.
- NAD+ precursors (e.g., NR, NMN): support sirtuin signaling, mitochondrial maintenance, and DNA repair processes.
- Methylene blue (low dose, select cases): can act as an electron cycler to support mitochondrial throughput.
- Anti-inflammatory diet and glycemic control: reduce oxidative burden and improve tissue recovery dynamics.
I emphasize shared decision-making and medical oversight for supplements—especially when interacting with existing medications. The goal is to align lifestyle, metabolic support, and MLS protocol so the patient’s tissues are primed for repair. This integrative framework reflects how I practice and teach at my clinics and platforms, where chiropractic adjustments, soft-tissue work, neuromuscular re-education, laser therapy, and metabolic optimization are woven into cohesive care pathways (see Chiromed and LinkedIn links in References).
Trigger Points and Fascial Networks: Precision Meets Systems Thinking
When addressing trigger points, I use the handpiece in short pulses with direct skin contact to deliver localized energy density that downregulates nociceptive fiber firing, relieves actin–myosin contracture, and improves local microcirculation. Simultaneously, the robotic head treats the broader fascial network, because trigger points rarely resolve in isolation. This combined strategy eases the “cooked meat” knot while restoring gliding in adjacent muscle and fascial planes. Integrative chiropractic care—active release techniques, instrument-assisted soft-tissue mobilization, and spinal mechanics correction—complements laser-induced biochemical changes, facilitating durable outcomes.
Safety, Durability, and Practical Use
MLS devices are built with durability; issues are rare once installed. Service networks can perform on-site maintenance as needed, thereby avoiding the risks associated with shipping heavy equipment. Patient sensations during MLS therapy are typically minimal:
- Most patients feel no pain, perhaps mild warmth or tingling.
- The pulsed nature of MLS minimizes surface heating, allowing higher peak power without thermal injury.
- If sensitivity occurs, I reassure patients that they may be “overachievers” in responsiveness—a lighthearted way to normalize their sensation—and I adjust parameters as needed.
Evidence Base and Methods: Modern, Multi-Wave, Dose-Controlled Research
The rationale for energy density targeting (4–10 J/cm²) stems from a combination of controlled trials, consensus guidelines, and mechanistic research in photobiomodulation. The World Association for Laser Therapy (WALT) and subsequent photobiomodulation consensus literature emphasize dosing by J/cm² to standardize clinical outcomes across devices and tissues. MLS’s dual-wavelength, pulsed-peak approach addresses known limitations of continuous-wave systems by minimizing superficial heat while increasing depth of effect. Studies in tendinopathies, osteoarthritis, neuropathic pain, and post-surgical recovery increasingly support structured protocols, with outcome measures including pain scales, functional scores, range of motion, and return-to-activity metrics. While device specifics differ, the consistent theme is that dose discipline, pulsed emission, and field geometry drive reproducibility.
Clinical Observations from Dr. Jimenez: Integrative Pathways That Work
At my clinics, I have seen:
- Low back facet pain responds rapidly when I combine robotic field coverage (centered on L4–L5, with slight medial/lateral expansion) with handheld trigger-point relief in the paraspinal bands. Chiropractic adjustments immediately after laser often hold better because the muscle tone and pain signaling are reduced.
- Knee osteoarthritis improvements in stair negotiation and walking distances when I treat the posterior knee, the medial and lateral compartments, and the anterior knee in flexion, paired with hip–core stabilization and gait retraining.
- Enhanced results with PRP when I follow the pre-injection priming, day-of modulation, and post-injection series approach described above.
- Faster return to activity in athletes when laser therapy is integrated with shockwave, chiropractic mobilization, and neuromuscular drills—each tool serving distinct biological and mechanical roles.
These observations align with the literature and underscore the importance of multimodal, sequence-aware care.
Practical Protocol Summary
- Low back facet pain:
- Robotic MLS: center X–Y over L4–L5 symptoms, expand to connect fascia; ~6 J/cm².
- Handpiece: 25-second bursts to paraspinal trigger points; direct skin contact.
- Schedule: 6 sessions acute; 12 for chronic; 24-hour spacing.
- Knee osteoarthritis:
- Treat the posterior and anterior compartments in flexion; add the medial/lateral compartments.
- Dose per compartment: around 6 J/cm²; let the device recalculate the time based on the area.
- Integrate chiropractic joint mobilization and soft-tissue work.
- PRP integration:
- 2–3 pre-injection MLS sessions.
- Day-of-injection MLS with tailored parameters.
- 6 post-injection MLS sessions.
- Reinforce with metabolic support as clinically appropriate (CoQ10, creatine, NAD+ precursors), while respecting medications.
- Trigger points:
- Handpiece, direct contact, short focused exposures; pair with robotic field treatment.
- Follow with manual therapy and corrective exercises.
Why Integrative Chiropractic Care Fits Perfectly
Laser therapy initiates biochemical cascades that reduce pain, inflammation, and tissue stiffness. Integrative chiropractic care then capitalizes on that improved tissue state. Adjustments and mobilizations realign joints; soft-tissue techniques free fascial restrictions; neuromuscular training restores movement efficiency. Together, they transform photobiomodulation’s cellular gains into functional victories—better posture, smoother gait, stronger lifts, and less recurrence. This integrated model is central to modern precision musculoskeletal care and is the foundation of how I approach complex cases in my practice.
Closing Thoughts
Laser therapy—especially MLS with dose-centered energy density and pulsed dual-wavelength design—has matured into a robust tool for musculoskeletal and integrative care. When layered thoughtfully with chiropractic methods, orthobiologics, and metabolic optimization, it helps patients move from short-term relief to durable function. The secret is not just the light; it is the protocol, the sequence, and the system we build around the patient’s biology and biomechanics. That is the essence of integrative care, and it is how we transform evidence into outcomes.
References
- World Association for Laser Therapy (WALT) recommendations for dosing in laser phototherapy. (n.d.). WALT.
- Photobiomodulation: Mechanisms and clinical applications. (2017). Photomedicine and Laser Surgery.
- Near-infrared and super-pulsed laser therapy: Dosimetry and biological effects. (2016). Lasers in Medical Science.
- Platelet-rich plasma combined with photobiomodulation: Outcomes and considerations. (2020). Lasers in Surgery and Medicine.
- Energy density over total joules: Dose-response in musculoskeletal photobiomodulation. (2016). Journal of Photochemistry and Photobiology B.
- Clinical observations and integrative protocols by Dr. Alexander Jimenez, DC, APRN, FNP-BC: ChiroMed-El Paso Integrative Practice and Dr. Jimenez on LinkedIn.
Post Disclaimer
General Disclaimer, Licenses and Board Certifications *
Professional Scope of Practice *
The information herein on "Integrative MLS Laser for Back Pain and PRP Support" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those on this site and on our family practice-based chiromed.com site, focusing on naturally restoring health for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine; wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics; subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and facilitate clinical collaboration with specialists across disciplines. Each specialist is governed by their professional scope of practice and licensure jurisdiction. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that directly or indirectly relate to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
(Board Certified: Family Practice Nurse Practitioner—Multistate)*
(Licensed Nurse Practitioner & Chiropractor - Multistate)*
Clinical Director
Digital Business Card
Dr. Maria Cardenas, MD
(Board Certified: Internal Medicine)
(Licensed Medical Doctor)
Medical Director, Clinical Director & Collaborative Physician
NPI # 1164426749
MD License #: J2933
Licenses and Board Certifications:
MD: Medical Doctor
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
(Board Certified: Family Practice Nurse Practitioner—Multistate)*
(Licensed Nurse Practitioner & Chiropractor - Multistate)*
Clinical Director
Digital Business Card
Dr. Maria Cardenas, MD
(Board Certified: Internal Medicine)*
(Licensed Medical Doctor)*
Medical Director, Clinical Director & Collaborative Physician
NPI # 1164426749
MD License #: J2933
📆 Schedule Appointment: Schedule 24/7 (Click Here)