Nutritional Yeast for Healthy Cooking and Nutrition
Can incorporating nutritional yeast be an option for individuals seeking a healthy vegan and vegetarian cheese substitute?

Nutritional Yeast
Nutritional yeast is a deactivated form of Saccharomyces cerevisiae yeast, commonly known as baker’s or brewer’s yeast. It’s popular in vegan and vegetarian cooking for its savory, cheesy flavor and nutritional benefits. Nutritional yeast is harvested, rinsed, and heat-dried to deactivate it, removing its leavening properties. This means it doesn’t cause food to rise but adds flavor and vital nutrients.
Nutrition
Nutritional yeast nutrition information is for 16 grams or around 1.5 tablespoons. (U.S. Department of Agriculture, 2019)
- Calories – 60
- Fat – 0.5 grams
- Sodium – 30 milligrams
- Carbohydrates – 5 grams
- Fiber – 3 grams
- Sugars – 0 grams
- Protein – 8 grams
- Thiamin – vitamin B1 – 10 milligrams
- Riboflavin – vitamin B2 – 10 milligrams
- Vitamin B6 – 12 milligrams
- Vitamin B12 – 24 micrograms
Carbohydrates
- Around 1.5 tablespoons contains 5 grams of carbohydrates, including 3 grams of fiber.
- Yeast provides an especially beneficial form of soluble fiber known as beta-glucan, with unique health benefits. (Bashir K. M. I., & Choi J. S. 2017)
Fats
- Most brands are naturally fat-free.
Protein
- It provides all essential amino acids with 8 grams per 1.5 tablespoons.
Vitamins and Minerals
Most nutritional yeast products are fortified with added B vitamins. Most provide 600% or more B vitamins per 16 grams and 1,000% of the daily value for vitamin B12, depending on the brand. It also has:
- Calcium
- Thiamin
- Iron
- Potassium
Nutritional Yeast Health Benefits
Health benefits include:
Reduces Risk of Anemia
Iron is typically the first nutrient to come to mind. However, inadequate folate or vitamin B12 also causes anemia. A common treatment for a vitamin B12 deficiency is injections, but large doses consumed can also be effective. (National Institutes of Health, Office of Dietary Supplements, 2024) Individuals who follow a plant-based or vegan diet often have limited sources of vitamin B12. Most brands of nutritional yeast are fortified with B12, providing more than 500% of the daily value per serving. Because B12 is water-soluble, it won’t cause toxicity when consumed in high doses and can serve as a key source of this essential nutrient.
Supports Heart Health
Nutritional yeast contains beta-glucan, a carbohydrate found in the cell walls of plants, bacteria, and fungi. Higher intakes lead to favorable cardiovascular outcomes, including lowering bad cholesterol and increasing good cholesterol. (Bashir K. M. I., & Choi J. S. 2017) In addition, most brands contain potassium, which reduces blood pressure.
Promote Healthy Immune System Function
More research is needed, but several studies have shown how yeast-derived beta-glucan can strengthen the immune system. (Stier H., Ebbeskotte V., & Gruenwald J. 2014) These benefits are attributed to beta glucan’s bacterial fermentation in the intestines. Beta-glucan may also stimulate the activity of crucial immune system cells, like macrophages.
Prevents Constipation
Fiber is essential. The recommended fiber intake is at least 25 to 35 grams daily. Unfortunately, many do not get enough. Nutritional yeast contributes 3 grams of fiber per 16 grams. Fiber regulates bowel movements by pulling water into the colon and adding bulk and softness to stool. (University of Michigan, 2008)
Using nutritional yeast can help reach an adequate fiber intake.
Diabetes Management
Getting enough fiber helps prevent blood sugar fluctuations. Low-fiber diets have been shown to increase the risk of diabetes in various populations. (Harvard T.H. Chan, School of Public Health, 2022) Fiber slows digestion and increases satiety, controlling hunger and the glycemic response. Fiber is beneficial for preventing diabetes and helping those with diabetes maintain good numbers.
Allergies
- Individuals who suspect a yeast or mold allergy see an allergist for a full evaluation.
- Yeast overgrowth is another possible condition that is unrelated to yeast allergies.
- Yeast overgrowth can occur in compromised immune systems or following antibiotic treatment.
- Because yeast is present in many foods, anyone with a true yeast allergy may have to avoid several food items, including baked goods, fermented alcoholic beverages, marmite/vegemite, sourdough bread, and certain multivitamins. (Cunningham E. 2013)
Adverse Effects
Nutritional yeast is inactive and unlikely to cause negative effects. However, for individuals who suffer from irritable bowel syndrome (IBS) or migraines, yeast may be a trigger. (UMass Medical School Center for Applied Nutrition, 2020)
Varieties
- Nutritional yeast may be sold as granules, powder, or flakes. (UMass Medical School Center for Applied Nutrition, 2020)
- Check the label to see if the product is fortified with added vitamins and minerals or has added sodium.
- Nutritional yeast is a dry food product available year-round in supermarkets or sold in a bulk food bin.
Storage, Safety, and Use
Although nutritional yeast is a dry product, it will stay in the refrigerator longer after it has been opened. Store it in an airtight container, and be mindful of the expiration date on the label.
It can be added to savory dishes such as pasta, roasted meats, vegetables, and salads. Ways to use include:
- On scrambled eggs.
- On top of garlic bread.
- Popcorn seasoning.
- Add to soups.
- In pasta dishes, as a substitute for parmesan cheese.
- An alternative to cheese sauce.
Injury Medical Chiropractic and Functional Medicine Clinic
Injury Medical Chiropractic and Functional Medicine Clinic works with primary healthcare providers and specialists to develop highly effective treatment plans through an integrated approach for each patient and restore health and function to the body through nutrition and wellness, functional medicine, acupuncture, Electroacupuncture, and integrated medicine protocols. We focus on what works for you to relieve pain, restore function, prevent injury, and mitigate issues through adjustments that help the body realign itself. The clinic can also work with other medical professionals to integrate a treatment plan to resolve musculoskeletal problems.
Learning About Food Substitutions
References
U.S. Department of Agriculture. FoodData Central. (2019). Nutritional yeast. Retrieved from https://fdc.nal.usda.gov/food-details/1744022/nutrients
Bashir, K. M. I., & Choi, J. S. (2017). Clinical and Physiological Perspectives of β-Glucans: The Past, Present, and Future. International journal of molecular sciences, 18(9), 1906. https://doi.org/10.3390/ijms18091906
National Institutes of Health, Office of Dietary Supplements. (2024). Vitamin B12: Fact sheet for health professionals. Retrieved from https://ods.od.nih.gov/factsheets/VitaminB12-HealthProfessional/
Stier, H., Ebbeskotte, V., & Gruenwald, J. (2014). Immune-modulatory effects of dietary Yeast Beta-1,3/1,6-D-glucan. Nutrition journal, 13, 38. https://doi.org/10.1186/1475-2891-13-38
University of Michigan. (2008). Bowel function anatomy. https://medicine.umich.edu/sites/default/files/content/downloads/bowel-function.pdf
Harvard T.H. Chan, School of Public Health. (2022). Fiber. https://nutritionsource.hsph.harvard.edu/carbohydrates/fiber/
Cunningham E. (2013). Is there a diet for “yeast allergy”? Journal of the Academy of Nutrition and Dietetics, 113(3), 484. https://doi.org/10.1016/j.jand.2013.01.013
UMass Medical School Center for Applied Nutrition. Chan, U., School, M., & Nutrition, C. F. A. (2020). Nutritional yeast: Nourishing or no-go? UM. https://www.umassmed.edu/nutrition/blog/blog-posts/2020/2/nutritional-yeast–nourishing-or-no-go/




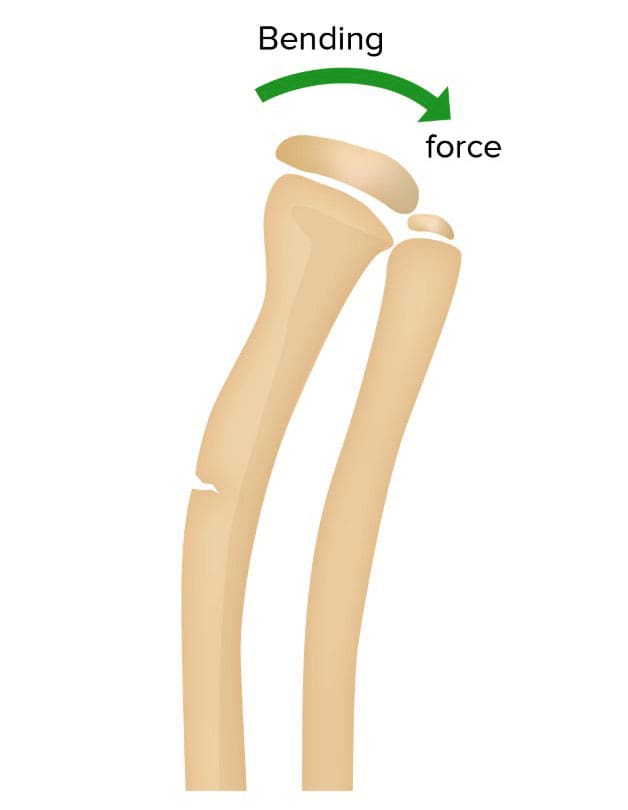 Causes
Causes