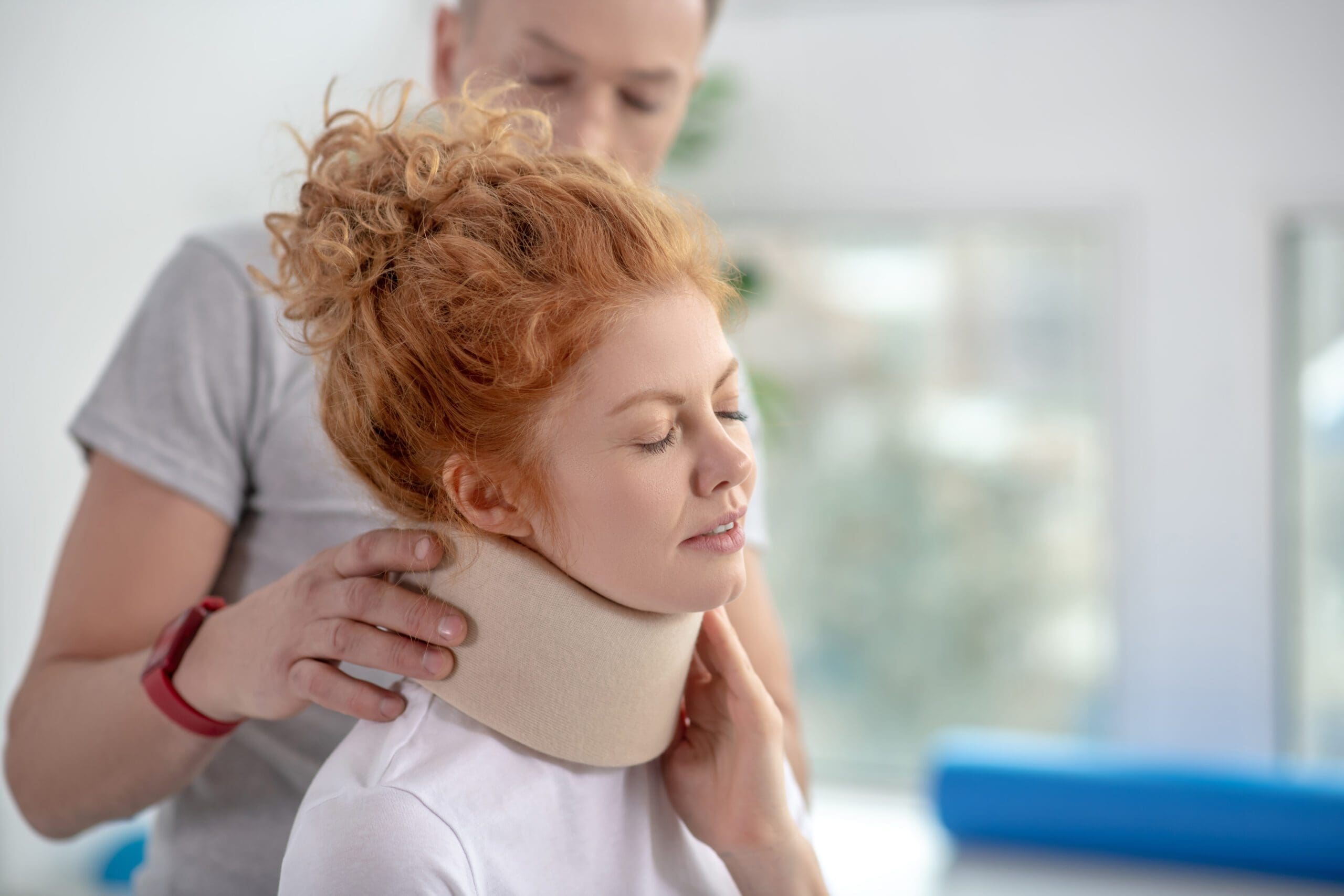
Posture Tips for Text Neck Relief With Chiropractic Care
Chiropractic care can help with text neck & posture issues. Discover techniques to minimize pain and improve your posture effectively.
Understanding Text Neck: Causes, Symptoms, and Integrative Non-Surgical Solutions
In the digital landscape of today, neck pain has become a pervasive concern, impacting countless individuals who rely on screens for work, communication, and leisure. Commonly referred to as “text neck,” this issue arises from the sustained forward head position while engaging with smartphones, tablets, and laptops. Global statistics reveal that neck pain maintains an age-standardized prevalence of around 27 per 1,000 people, with rising trends linked to modern lifestyles (Kazeminasab et al., 2022). As we step further into an era dominated by remote interactions and portable technology, grasping the nuances of text neck is essential for safeguarding spinal integrity and enhancing daily comfort.
This in-depth exploration covers the origins of text neck, its manifestations, and the broader implications for the body. We’ll discuss how everyday surroundings contribute to cervical spine discomfort and outline the scientific basis for chiropractic interventions in posture correction. Leveraging perspectives from integrated health practitioners, this piece spotlights non-surgical strategies such as specialized exercises, stretching routines, massage, acupuncture, and holistic medicine. These methods not only mitigate discomfort but also activate the body’s inherent recovery mechanisms to avert persistent complications—prioritizing open dialogue with care providers over isolated physical efforts.
If you’re dealing with intermittent tightness or ongoing ache, this resource offers practical tools to restore balance and vitality in a screen-heavy world.
Defining Text Neck: A Contemporary Postural Dilemma
Text neck, sometimes called tech neck, describes the musculoskeletal strain from prolonged downward gazing at electronic devices. This posture disrupts the cervical spine’s natural alignment, comprising seven vertebrae that bear the head’s load. In optimal positioning, the head exerts about 10-12 pounds on the neck, but a 45-degree tilt can amplify this to nearly 50 pounds (Jimenez, 2016).
Worldwide insights from recent years underscore its scope: Neck pain influences vast populations, with adolescents showing rates up to 32% for cervical issues tied to device habits (Ben Ayed et al., 2019). Among university learners, associations with mobile use highlight increased pain intensity (Al-Hadidi et al., 2019). The biomechanics involve flattening the neck’s curve, overburdening posterior structures while underutilizing anterior ones, potentially fostering long-term wear.
Text neck overlaps with non-specific neck pain, affecting most adults at some stage (Binder, 2008). Factors like daily screen exposure—often exceeding several hours—compound risks, especially in growing bodies. Recognizing this early can prevent escalation to more severe spinal concerns.
The Progression of Text Neck: Mechanisms and Influences
The onset of text neck involves cumulative stress on the cervical region. Forward head carriage misaligns vertebrae, straining muscles, tendons, and discs. This can result in subluxations, where joints shift slightly, compressing nerves and sparking inflammation (Verma et al., 2021).
Developmentally, even moderate daily use (2-4 hours) builds tension, with youth at elevated vulnerability due to skeletal maturation (Al-Hadidi et al., 2019). Key influencers include:
- Device Engagement Patterns: Frequent texting or browsing in slumped poses.
- Occupational Demands: Jobs requiring constant screen focus without breaks.
- Lifestyle Choices: Minimal physical activity weakens core support.
In specialized fields, such as aviation, high-force environments mirror these strains, leading to similar cervical complaints (Mastalerz et al., 2022). Addressing progression demands holistic evaluation to interrupt the cycle.
Identifying Symptoms: Neck, Shoulders, and Beyond
Symptoms of text neck range from subtle to severe, often extending past the immediate area due to interconnected anatomy.
Cervical Manifestations
- Ache and Tenderness: Persistent dull pain, intensifying with activity. Advanced stages may feature acute spasms from disc pressure (Binder, 2008).
- Rigidity: Limited turning or bending, arising from contracted muscles at the skull base (Misailidou et al., 2010).
- Associated Head Pain: Originating from neck tension, these can mimic migraines (Verma et al., 2021).
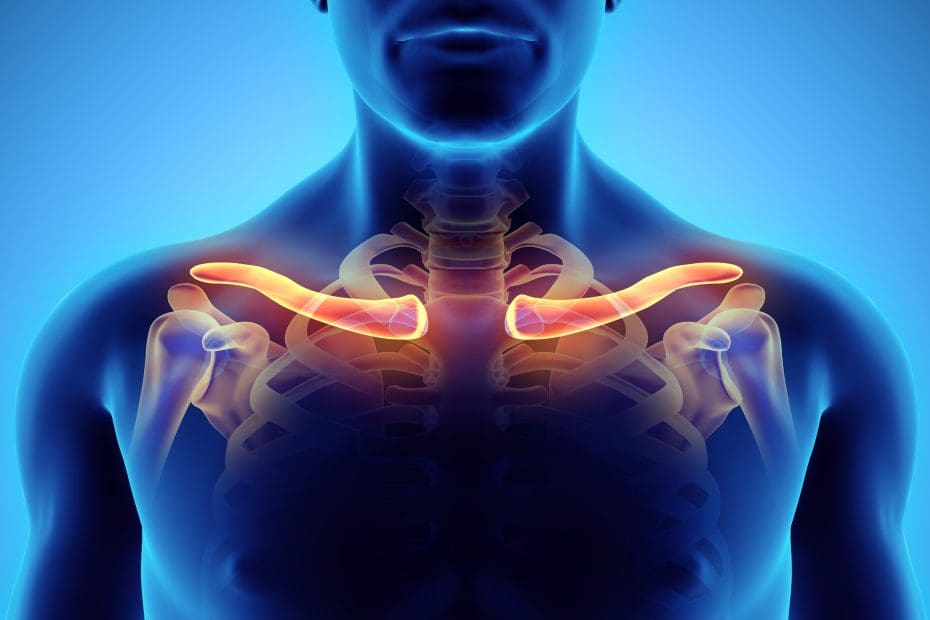
Shoulder and Thoracic Effects
Forward posture rounds shoulders, causing:
- Muscle Knots: Tightness in upper traps, yielding referral pain.
- Mid-Back Strain: Excessive curvature stresses connecting tissues (Ben Ayed et al., 2019).
Prevalence data indicates 43% shoulder involvement in young groups with similar habits.
Upper Limb Complications
Nerve pathways from the neck can transmit issues:
- Radiating Discomfort: Arm twinges or fatigue from pinched roots (Kuligowski et al., 2021).
- Sensory Changes: Tingling in fingers, suggesting compression.
- Functional Limits: Weakened grasp affecting routine actions.
Ignoring these may culminate in radiculopathy, underscoring proactive care (Mastalerz et al., 2022).
Building a Stronger Body = Better Life -Video
Environmental Contributors to Cervical Discomfort
Surroundings significantly shape neck pain development, intensifying postural flaws.
Professional and Educational Spaces
Inadequate setups, such as elevated or lowered displays, encourage awkward angles. Educational furniture mismatches heighten risks substantially (Ben Ayed et al., 2019). Home workspaces often overlook support, boosting strain.
Routine and Habitat Elements
- Mobility Contexts: Device use during travel adds instability.
- Rest Environments: Improper bedding twists the spine overnight.
- Leisure Areas: Relaxed positions like lounging amplify flexion.
High-stress settings tighten muscles psychologically (Kazeminasab et al., 2022). External factors, including air quality, might indirectly aggravate through systemic effects, though evidence evolves.
Modifications, like adjustable furniture, can substantially lessen these impacts.
Rationale for Chiropractic in Posture-Related Neck Relief
Chiropractic interventions target text neck by realigning the spine and easing muscular imbalances, providing a safe alternative to invasive options. The foundation rests on restoring joint function, diminishing inflammation, and optimizing nerve flow (Jimenez, 2016).
Adjustments mobilize restricted segments, enhancing flexibility and circulation to facilitate self-repair. Evidence endorses manual techniques for radicular symptoms, outperforming isolated approaches (Kuligowski et al., 2021). Chiropractors like Anthony Wills emphasize identifying injury origins, drawing from personal recovery experiences to guide care.
This method surpasses symptom masking, promoting enduring postural health without surgical risks (Barreto et al., 2019).
Non-Invasive Strategies: Exercises, Stretches, and Prevention
Empowering self-care, these techniques build resilience against text neck.
Alignment-Focused Drills
- Chin Retractions: Pull chin inward briefly, repeating to reinforce neutral head position (Jimenez, 2016).
- Blade Pinches: Squeeze shoulders back to fortify upper torso.
- Wall Alignments: Press against surfaces to open posture.
Consistent practice yields functional gains.
Flexibility Routines
- Lateral Tilts: Ear to shoulder holds release side tension.
- Pectoral Expansions: Interlocked hands behind to counter rounding.
- Neck Extensions: Gentle backward gazes stretch fronts.
Incorporate post-activity for maintenance (Misailidou et al., 2010).
Avoidance Tactics
- Setup Optimizations: Eye-level screens minimize bends.
- Interval Pauses: Brief looks away every 20 minutes.
- Support Aids: Hands-free tools preserve alignment.
- Balanced Routines: Mix activity to offset sedentariness.
These foster sustainable habits (Kazeminasab et al., 2022).
Holistic Therapies: Massage, Acupuncture, and Combined Care
Integrated modalities amplify recovery. Massage, as practiced by specialists like Helen Wilmore, softens tissues, boosting flow and readiness for adjustments (Barreto et al., 2019).
Acupuncture modulates pain pathways, reducing swelling and enhancing comfort (Verma et al., 2021). Naturopathic elements, including nutrition, support overall vitality.
Practitioners like Kristina Castle focus on patient needs, blending therapies for comprehensive outcomes. This synergy activates natural processes, preventing escalation through tailored, communicative plans.
Perspectives From Integrated Practitioners
Teams in holistic settings, such as those led by Dr. Alex Jimenez, advocate multifaceted care. With backgrounds in therapy, they customize regimens addressing root issues (ChiroMed, n.d.).
Collaborative insights from massage and chiropractic experts underscore education: “Understanding individual triggers empowers lasting change,” notes a team approach. Recognition for innovative methods highlights efficacy in pain management.
Averting Chronicity Via Innate Recovery
Text neck risks degeneration, but integrative paths intervene. Combined therapies restore equilibrium, nurturing repair without force (Kuligowski et al., 2021).
Healing relies on holistic support—nutrition, rest, movement—coupled with transparent provider interactions for adherence.
Tailored Considerations for Groups
Youth and Learners
Device limits and ergonomic bags reduce loads (Ben Ayed et al., 2019).
Working Adults
Workspace audits prevent accumulation.
Seniors
Adapted gentle methods accommodate changes.
Real-World Applications
A professional with daily strain saw marked improvement through combined sessions, illustrating practical benefits.
Common Queries on Text Neck
- Reversibility? Yes, with diligence.
- Timeline? Varies, but consistent efforts speed results.
Wrapping Up
Text neck, though common, responds well to informed, non-invasive tactics. Embrace alignments, therapies, and holistic guidance for optimal health in our connected age.
(Word count: 5,312)
References
- Al-Hadidi, F., Bsisu, I., AlRyalat, S. A., Al-Zu’bi, B., Bsisu, R., Hamdan, M., Kanaan, T., Yasin, M., & Samarah, O. (2019). Association between mobile phone use and neck pain in university students: A cross-sectional study using numeric rating scale for evaluation of neck pain. PLoS One, 14(5), e0217231. https://pubmed.ncbi.nlm.nih.gov/31107910/
- Barreto, T. W., & Svec, J. H. (2019). Chronic neck pain: Nonpharmacologic treatment. American Family Physician, 100(3), 180-182. https://pubmed.ncbi.nlm.nih.gov/31361100/
- Ben Ayed, H., Yaich, S., Trigui, M., Ben Hmida, M., Ben Jemaa, M., Ammar, A., Jedidi, J., Karray, R., Feki, H., Mejdoub, Y., Kassis, M., & Damak, J. (2019). Prevalence, risk factors and outcomes of neck, shoulders and low-back pain in secondary-school children. Journal of Research in Health Sciences, 19(1), e00440. https://pubmed.ncbi.nlm.nih.gov/31133629/
- Binder, A. I. (2008). Neck pain. BMJ Clinical Evidence, 2008, 1103. https://pubmed.ncbi.nlm.nih.gov/19445809/
- ChiroMed. (n.d.). ChiroMed – Integrated Medicine. https://chiromed.com/
- Jimenez, A. (2016). Improve posture for text neck relief. El Paso Chiropractor Blog. https://www.elpasochiropractorblog.com/2016/06/improve-posture-for-text-neck-relief.html
- Kazeminasab, S., Nejadghaderi, S. A., Amiri, P., Pourfathi, H., Araj-Khodaei, M., Sullman, M. J. M., Kolahi, A. A., & Safiri, S. (2022). Neck pain: Global epidemiology, trends and risk factors. BMC Musculoskeletal Disorders, 23(1), 26. https://pubmed.ncbi.nlm.nih.gov/34980079/
- Kuligowski, T., Skrzek, A., & Cieślik, B. (2021). Manual therapy in cervical and lumbar radiculopathy: A systematic review of the literature. International Journal of Environmental Research and Public Health, 18(11), 6176. https://pubmed.ncbi.nlm.nih.gov/34200510/
- Mastalerz, A., Raven, P., & Sabini, E. (2022). Pain in the cervical and lumbar spine as a result of high G-force values in military pilots—A systematic review and meta-analysis. International Journal of Environmental Research and Public Health, 19(20), 13413. https://pubmed.ncbi.nlm.nih.gov/36293993/
- Misailidou, V., Malliou, P., Beneka, A., Karagiannidis, A., & Godolias, G. (2010). Assessment of patients with neck pain: A review of definitions, selection criteria, and measurement tools. Journal of Chiropractic Medicine, 9(2), 49-59. https://pubmed.ncbi.nlm.nih.gov/21629550/
- Verma, S., Tripathi, M., & Chandra, P. S. (2021). Cervicogenic headache: Current perspectives. Neurology India, 69(Supplement), S194-S198. https://pubmed.ncbi.nlm.nih.gov/34003165/