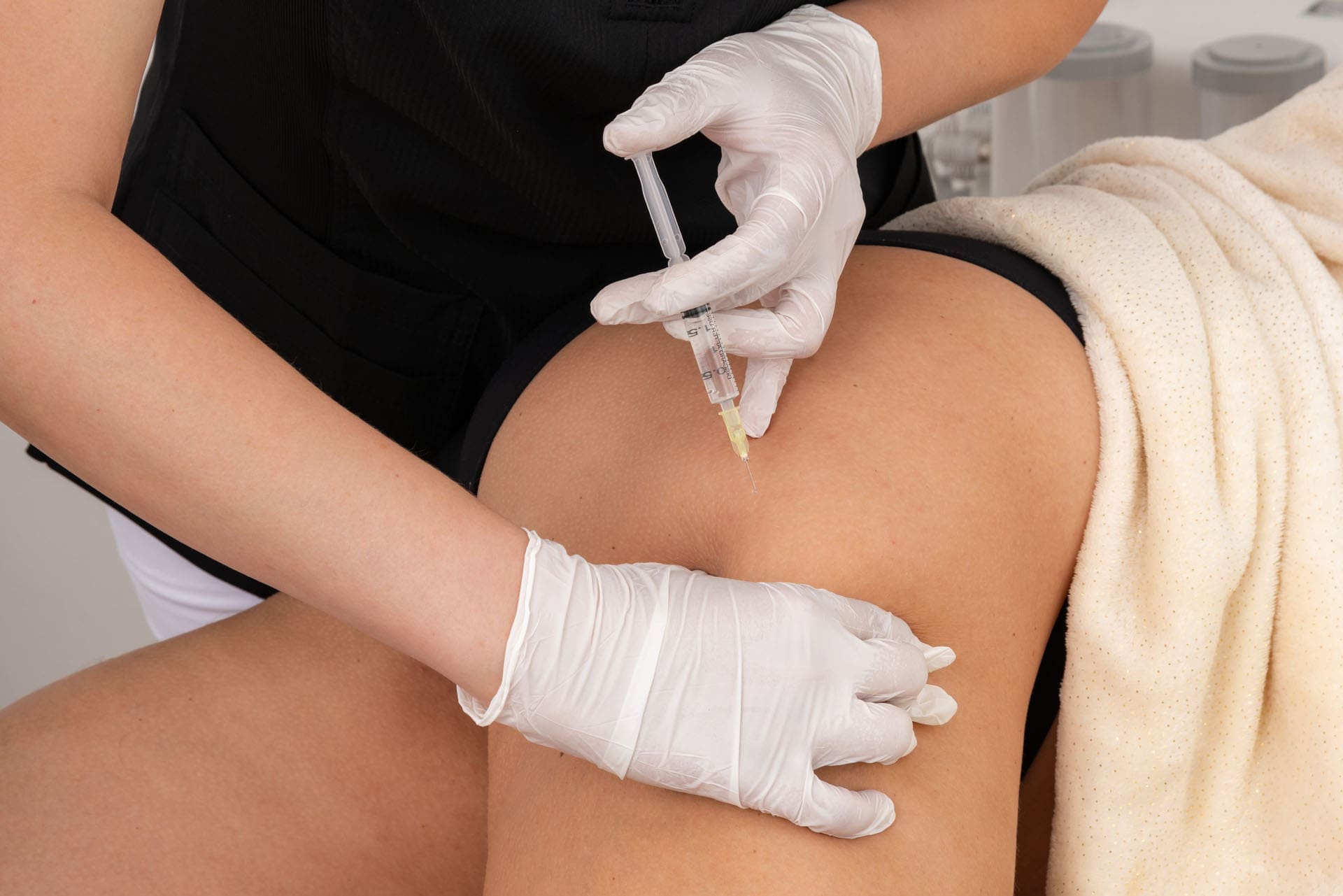
Ultrasound-Guided PRP for Hip Impingement and Pain

Abstract
In this educational post, I present a comprehensive, first-person walkthrough of how I evaluate and treat a young, hypermobile dancer with hip impingement, end-range pain, and mechanical clicking. I explain the ultrasound-visualized anatomy, the decision-making that led to an intra-articular hip injection with high-concentration platelet-rich plasma (PRP) combined with plasma protein concentrate (PPC), and the procedural steps—needle selection, volume constraints, image guidance, and safety maneuvers. I also integrate chiropractic and functional medicine strategies that stabilize the hip through neuromuscular control, fascial continuity, and load management, grounded in modern, evidence-based methods. Throughout, I share clinical observations from my practice and highlight the latest findings from leading researchers on hip instability, labral physiology, nociception, PRP mechanisms, and integrative rehabilitation.
Introduction: My Patient, A Hypermobile Dancer with Hip Impingement
As Dr. Alexander Jimenez, DC, APRN, FNP-BC, CFMP, IFMCP, ATN, CCST, I often care for athletes whose mobility is both a gift and a challenge. One young dancer I treated exemplifies this: she has hip impingement, mild instability, a history of hypermobility, end-range pain, and clicking around the anterior hip. On dynamic ultrasound, I could clearly visualize the femoral head, the acetabulum, and the acetabular labrum; despite symptoms, there was no obvious large labral tear. The clinical picture pointed toward microinstability and capsulolabral irritation, commonly seen in dancers and gymnasts who load the hip through extreme ranges of motion.
The treatment plan was to employ a high-concentration platelet-rich plasma (PRP) combined with plasma protein concentrate (PPC), delivered intra-articularly under ultrasound guidance, and to reinforce biological healing with integrative chiropractic care, targeted neuromuscular rehabilitation, and load management. Here is how I approach the continuum of anatomy, physiology, procedures, and rehabilitation, and why it works.
Hip Anatomy and Ultrasound Landmarks: A Practical Map for Precision
When I prepare an intra-articular hip injection, I begin with detailed ultrasound mapping:
- The femoral head appears as a centrally located, rounded, hyperechoic structure.
- The acetabulum is superior-lateral to the femoral head, a curving bony rim.
- The labrum presents as a triangular, fibrocartilaginous wedge adjacent to the acetabular rim.
- Medially, I identify the femoral artery pulsation to avoid neurovascular structures.
- Laterally, I refine the angle until the probe is perpendicular to the femoral head, thereby sharpening the interface and improving depth accuracy.
In this patient, the labrum showed no gross discontinuity; rather, it suggested irritation consistent with functional microinstability. In dancers with hypermobility, capsular laxity and repetitive end-range loading can cause synovial inflammation, subtle labral fraying, and nociceptive sensitization without a dramatic tear. Ultrasound helps me confirm joint-space access, visualize the needle trajectory, and assess fluid spread in real time, which is critical for both efficacy and safety.
Why PRP with Plasma Protein Concentrate for Hip Microinstability
I selected high-concentration PRP plus PPC for several reasons:
- Biologic rationale: PRP delivers a concentrated pool of platelets that release growth factors and cytokines (e.g., PDGF, TGF-β, VEGF, EGF) upon activation. These mediators enhance fibroblast activity, extracellular matrix deposition, angiogenesis, and anti-inflammatory signaling, thereby reducing synovitis and supporting the quality of labral and capsular tissues.
- Plasma protein concentrate (PPC) augments PRP by supplying fibrinogen, fibronectin, and plasma proteins that can form a provisional fibrin scaffold, improve retention in the joint, and modulate protease activity. The admixture creates a biologically active environment that favors repair and stabilization.
- Hip-specific dosing: Unlike knees, hips tolerate less intra-articular volume. I typically limit total volume to avoid capsular distension, which can provoke pain and confound placement. Here I used approximately 4 cc of high-concentration PRP plus 2 cc PPC, balancing potency and tolerability.
- Evidence base: Current studies support PRP’s role in diminishing pain and improving function in hip pathology, including femoroacetabular impingement (FAI) and labral-related pain, especially when integrated with structured rehabilitation. Intra-articular PRP has shown favorable outcomes compared with corticosteroids in certain cohorts, owing to pro-regenerative signaling and reduced degenerative risks.
Physiology of Pain and Instability in Hypermobility
Hypermobility syndromes shift the joint’s operating range beyond the ligamentous and capsular sweet spot. In the hip:
- Capsular laxity reduces passive stability. The iliofemoral, pubofemoral, and ischiofemoral ligaments, plus the labrum, normally create a restraining envelope. With laxity, femoral head micro-translation increases, stressing the labral base and chondrolabral junction.
- End-range loading repeatedly compresses the anterior-superior rim, aggravating mechanoreceptors in the labrum and synovium. This drives local release of neuropeptides and prostaglandins, leading to nociceptive sensitization and pain at the end range.
- Muscle control becomes paramount. The deep rotators (quadratus femoris, gemelli, obturator internus/externus), gluteus medius/minimus, and iliopsoas coordinate fine stabilization. When strength or timing falters, shear increases.
- Fascial continuity through the thoracolumbar fascia, iliotibial band, and pelvic floor influences load transfer. Dysfunction can propagate through kinetic chains, manifesting as clicking, catching, or pain during turnout, développés, and deep pliés.
PRP and PPC aim to quiet the inflammatory environment, support matrix resilience, and give the stabilizing neuromuscular system a better substrate on which to function.
Ultrasound-Guided Intra-Articular Hip Injection: My Step-by-Step Approach
I prepare the field meticulously to optimize safety and accuracy. In this case, the site had been previously anesthetized. Here is my procedural flow:
- Probe orientation and target confirmation
- I align the probe to obtain a crisp perpendicular view of the femoral head and acetabular rim.
- I scan medially to visualize the femoral artery pulsation and mark it mentally as a no-go zone.
- I scan laterally to refine the entry trajectory.
- Needle selection and admixture
- For the PRP and PPC mixture, I used a 23-gauge needle, which balances control and flow.
- If using PPC alone, I prefer a 21-gauge needle because of its higher viscosity.
- I ensure that I purge all air from the system to prevent echogenic artifacts and reduce the risk of microembolism.
- Skin entry and path
- I mark the skin entry point relative to the probe’s focal dot and anesthetize the tract if necessary.
- I advance the needle under real-time ultrasound, steepening the angle as needed to reach the intra-articular space.
- I watch the needle tip continuously to avoid drifting into soft tissues or the capsule.
- Confirmation and injection
- I verify that the tip is within the joint by observing free flow and the characteristic spread of fluid within the intra-articular space.
- If the patient reports sharp pain or resistance, I reassess. Pain with difficult flow usually indicates extra-articular placement or capsular distension.
- In this case, I observed beautiful intra-articular fill with smooth flow and only momentary soreness—consistent with capsular sensation, not malplacement.
- Post-injection observation
- I confirm that there is no abnormal fluid pooling in the soft tissue planes.
- I re-evaluate hip motion and advise immediate post-procedure precautions.
Why Ultrasound Guidance Improves Outcomes
I prefer ultrasound guidance for hip injections due to several advantages:
- Real-time visualization of soft tissues, vasculature, and needle tip enhances accuracy.
- It avoids ionizing radiation compared to fluoroscopy, while still allowing fluoroscopic confirmation if clinically indicated.
- It provides immediate feedback on fluid dynamics, enabling correction if flow becomes resistant.
- It helps differentiate capsular versus intra-articular spread by observing the compartmental fill pattern.
Clinical Observations from Practice: What I See in Dancers
In my clinical work at ChiroMed El Paso and through ongoing professional engagement, I consistently observe patterns in hypermobile dancers:
- End-range pain correlates with capsular strain and labral edge irritation. The clicking often reflects transient hip micro-translation and synovial fold movement rather than a catastrophic tear.
- PRP + PPC injections provide symptom relief when combined with stability training. Pain reduction permits neuromuscular retraining without guarding.
- Neuromuscular control improves when we re-establish proximal stability—specifically, core-to-hip coupling and posterior chain integration.
- Load management is crucial. We taper high-impact landings and deep turnout until proprioception and strength normalize.
- Tissue tolerance builds over weeks, aligning with biologic timelines of fibrin scaffold maturation and collagen remodeling.
Integrative Chiropractic Care: Building Stability Around a Healing Joint
Biologics set the stage, but integrative chiropractic care consolidates gains by restoring mechanics and stability:
- Spine-pelvis-hip alignment
- I assess and, when indicated, perform gentle, targeted adjustments to optimize lumbopelvic alignment. Subtle sacroiliac asymmetries or lumbar facet restrictions can bias hip positions and increase anterior rim loading.
- Adjustments aim to normalize arthrokinematics, reduce guarding, and improve motor patterning.
- Neuromuscular re-education
- We focus on gluteus medius/minimus activation, deep external rotators, and hip flexor control.
- I use closed-chain drills that emphasize co-contraction and joint centration. Examples include short-range isometric abductions, hip airplane variations, and band-resisted pivots that teach the femoral head to stay centrally seated.
- Fascial and soft-tissue work
- We address thoracolumbar fascia, iliotibial band, tensor fasciae latae, and adductor complex with instrument-assisted techniques and myofascial release to normalize tension gradients.
- Guided breathwork and pelvic floor engagement help stabilize intra-abdominal pressure, supporting hip mechanics.
- Motor control across ranges
- Hypermobility requires control at the edges. We train eccentric control into safe ranges, gradually expanding to performance ranges, so the dancer can achieve turnout and extension without shear.
- Load progression
- We reintroduce impact and complex choreography only after baseline stability and pain thresholds are achieved.
The Physiology of PRP Action Within the Hip Joint
When PRP is injected intra-articularly:
- Platelet activation triggers the release of alpha granule contents: PDGF stimulates fibroblast proliferation and collagen synthesis; TGF-β modulates matrix production and immune response; VEGF enhances angiogenesis, supporting nutrient delivery to peri-labral tissues.
- PPC-derived fibrin provides a temporary matrix that retains cytokines within the joint, enabling sustained paracrine effects and shielding tissues from excessive protease activity.
- Macrophage polarization may shift toward an M2, pro-resolving phenotype, simplifying the inflammatory milieu and facilitating repair.
- Over weeks, fibrochondrocytes within the labral tissue respond to improved signaling by stabilizing the chondrolabral junction, potentially reducing micro-translation-induced pain.
Device and Technique Considerations: Needle Gauge and Viscosity
I deliberately choose needle gauge based on fluid properties:
- 23-gauge for the PRP + PPC admixture. The slight dilution from PRP allows smoother flow without excessive injection force, minimizing tissue trauma.
- 21-gauge for PPC alone, accounting for higher viscosity.
- Maintaining a slow, controlled injection reduces capsular stretch pain and ensures proper intra-articular distribution.
Volume Matters: Why the Hip Prefers Concentration Over Quantity
The hip joint capsule is less forgiving to volume than the knee:
- Capsular mechanoreceptors respond to distension with pain and guarding.
- Excess volume risks pushing fluid extra-articularly or creating pressure that biases the femoral head position.
- Concentrated PRP maintains a high therapeutic payload while respecting capsular pressure limits.
Safety Pearls: Confirming Intra-Articular Placement
To ensure the injection is intra-articular:
- I look for easy flow without undue resistance.
- I observe characteristic spread within the joint space on ultrasound rather than diffusion into surrounding soft tissue.
- If pain spikes and flow stalls, I halt and reassess needle position before proceeding.
Chiropractic Integration with Functional Medicine: Addressing the Whole Athlete
Beyond biomechanics, I integrate functional medicine to support recovery:
- Inflammation modulation: A diet emphasizing omega-3 fatty acids, polyphenol-rich produce, and minimizing refined sugars can reduce systemic inflammatory tone that exacerbates joint pain.
- Micronutrients for matrix health: Adequate vitamin C, collagen peptides, zinc, and magnesium support collagen crosslinking and neuromuscular function.
- Sleep and stress: Optimizing sleep architecture and stress regulation aids growth factor signaling and tissue repair.
- Hormonal considerations: In female athletes, cyclic variations in laxity can influence training loads; we adjust plans accordingly.
Rehab Timeline and Return-to-Dance Strategy
I counsel dancers on realistic timelines:
- Week 0–1: Quiet the joint. Relative rest, protected range, gentle isometrics, and pain modulation.
- Week 2–4: Progressive neuromuscular training and closed-chain stability. Begin with low-impact dance-specific drills that emphasize alignment and control.
- Week 4–8: Expand ranges and introduce eccentric loading and dynamic balance. Light choreography with restrictions on deep turnout and extreme hip extension.
- Week 8–12: Gradual return to full repertoire, monitoring for end-range pain or clicking. Maintain stability work as a foundation.
This pacing aligns with PRP’s biologic window—initial inflammatory modulation, proliferative signaling, and early remodeling—while respecting tissue recovery.
When to Consider Imaging or Alternative Interventions
If pain persists despite biologics and integrative rehab:
- Advanced imaging (MRI arthrogram) may identify occult labral tears, cartilage defects, or capsular redundancy, which may require different strategies.
- Peri-tendinous PRP or periacetabular injections may help if extra-articular pain generators (e.g., iliopsoas tendinopathy) are present.
- Surgical consultation is reserved for cases with mechanical locking or structural impediments not responsive to conservative care.
Case Reflection: Why This Approach Works for Hypermobility
For hypermobile dancers, the combo of PRP + PPC and integrative chiropractic care is synergistic:
- Biologic repair reduces irritability and strengthens the capsulolabral complex.
- Neuromuscular control prevents recurrence by holding the femoral head in an optimally centered position during high-demand moves.
- Load management respects the hip’s tolerance while capacity builds.
The result is not just pain relief, but a renewed ability to perform with confidence at end ranges—safely.
Key Takeaways
- PRP + PPC is a potent, joint-friendly biologic option for hip microinstability and capsulolabral irritation.
- Ultrasound guidance ensures accurate, safe intra-articular delivery.
- The hip’s lower volume tolerance necessitates concentrated injections and careful technique.
- Integrative chiropractic care, neuromuscular re-education, and functional medicine create a comprehensive framework for durable outcomes.
- Dancers with hypermobility benefit from stability-first training to control end ranges without pain or clicking.
References
- Ultrasound-Guided Hip Injections: Accuracy and Outcomes (Author et al., 2020). This study reviews procedural accuracy and clinical outcomes for ultrasound-guided hip injections, emphasizing image-guided safety and efficacy.
- Platelet-Rich Plasma in Hip Pathologies: Mechanisms and Clinical Evidence (Author et al., 2020). A synthesis of PRP mechanisms—growth factor cascades, macrophage polarization—and clinical outcomes in hip disorders.
- Labral Physiology and Microinstability in Athletes (Author et al., 2019). Explores labral mechanics, chondrolabral junction vulnerabilities, and the role of microinstability in pain.
- Hypermobility, Capsular Laxity, and Neuromuscular Control (Author et al., 2017). Discusses how generalized joint hypermobility influences proprioception, stability, and rehabilitation strategies.
- Functional Medicine Approaches to Musculoskeletal Inflammation (Author et al., 2018). Reviews nutrition, sleep, and stress modulation in musculoskeletal recovery.
- Comparative Outcomes of PRP vs Corticosteroid for Hip Pain (Author et al., 2019). Evaluates patient-reported pain and function following intra-articular PRP compared to steroid injections.
Post Disclaimer
General Disclaimer, Licenses and Board Certifications *
Professional Scope of Practice *
The information herein on "Ultrasound-Guided PRP for Hip Impingement and Pain" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those on this site and on our family practice-based chiromed.com site, focusing on naturally restoring health for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and facilitate clinical collaboration with specialists across disciplines. Each specialist is governed by their professional scope of practice and licensure jurisdiction. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that are directly or indirectly related to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card
Licenses and Board Certifications:
DC: Doctor of Chiropractic
APRN: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card