Understanding Therapeutic Approaches for Tissue Regeneration with Photobiomodulation
Discover the impact of photobiomodulation in tissue regeneration and its therapeutic approaches for better health.
Abstract
In this educational post, I walk you through how I evaluate and apply modern, multiwavelength laser therapy using MLS technology for low back pain, facet-mediated joint pain, knee osteoarthritis, soft-tissue injuries, and orthobiologic integrations such as PRP. From patient positioning and dosing to understanding the physiological cascade of photobiomodulation, I present the latest research and clinical protocols, explain why we calibrate to energy density in joules per square centimeter, and outline how integrative chiropractic care improves outcomes through precise mechanical assessment, neuromuscular re-education, and connective-tissue engagement. You will learn how dosing windows, pulse structure, and wavelength selection support analgesia, resolution of inflammation, mitochondrial function, and microcirculatory improvements—plus how to safely combine laser therapy with rehabilitation, shockwave, and PRP in a stepwise, patient-centered plan.
Introduction: My Clinical Framework for MLS Laser Therapy
As Dr. Alexander Jimenez, DC, APRN, FNP-BC, CFMP, IFMCP, ATN, CCST, I blend integrative chiropractic care with advanced rehabilitative technologies to optimize musculoskeletal outcomes. Over decades in clinics and interdisciplinary settings, I’ve seen that the most important variable in laser success is not just the device—it’s the workflow, patient comfort, anatomical precision, and dosing discipline. Modern MLS laser systems deliver synchronized dual wavelengths—typically an 808-nm continuous component and a 905-nm pulsed component—engineered to maximize therapeutic photobiomodulation while minimizing thermal load at the surface. The result is consistent dosing to the targeted tissue with reduced risk of superficial overheating.
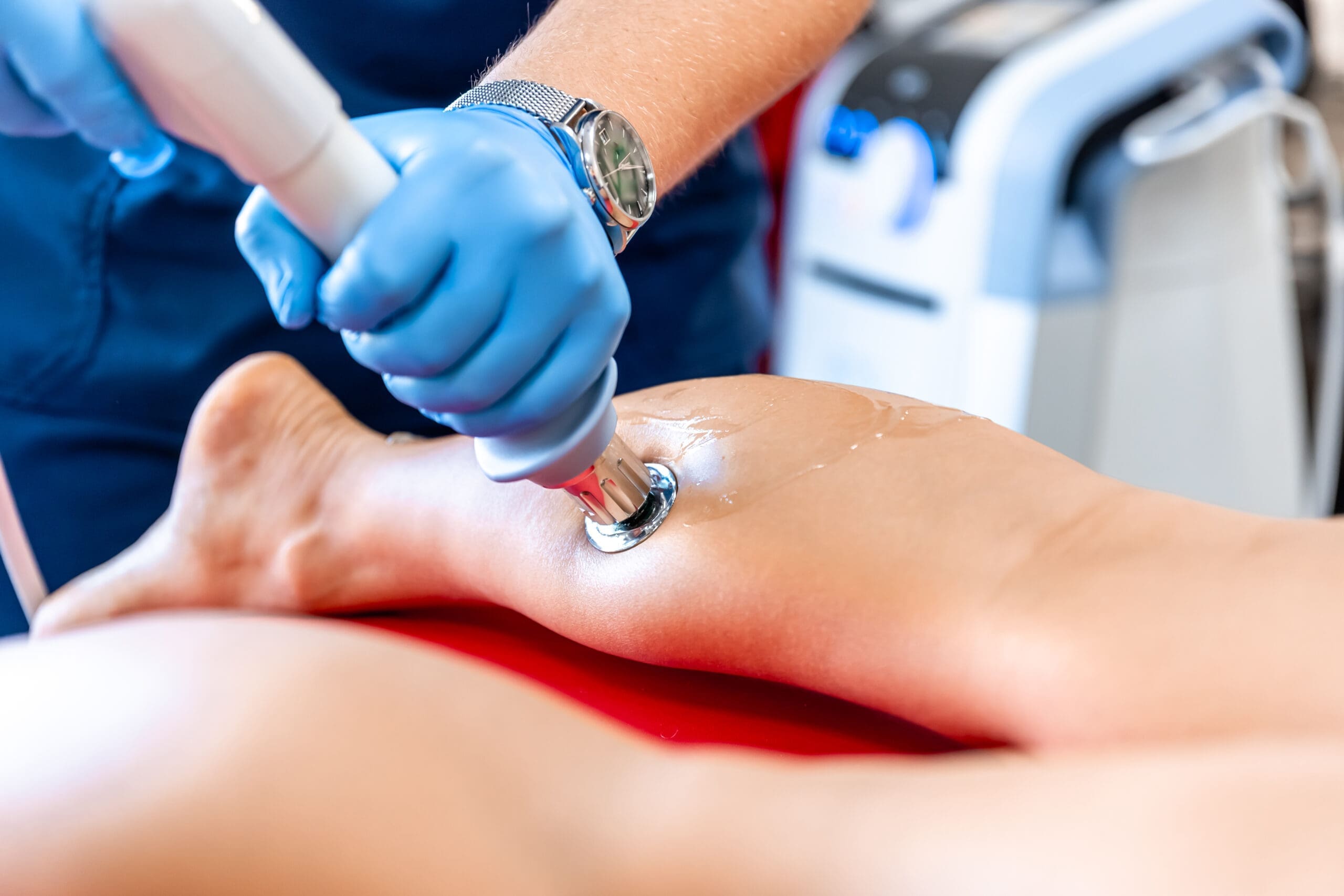
Below, I reframe a hands-on demonstration into a patient-centered journey, explain the science, and share how I incorporate these methods with chiropractic assessment, trigger point discovery, fascial continuity, and orthobiologic protocols. I aim to ensure you not only know what to do but also why to do it—and how to apply it safely and effectively using the latest evidence.
Patient Comfort and Positioning: The Starting Point for Precision
Key clinical lesson: Patient comfort is critical. When a robotic laser array is programmed to a precise region, movement ruins alignment and compromises dose delivery. For lumbar facet and paraspinal treatments:
- Positioning:
- Low back cases are set up face down (prone) for spine-neutral exposure.
- The laser head must be at the correct focal distance—often around 6 inches for a robotic MLS head—with a manufacturer-provided ruler to ensure the sweet spot for beam collimation.
- Handheld diodes are applied directly to the skin for punctual targets, such as trigger points or joint spaces, where tactile feedback guides accuracy.
- Why positioning matters physiologically:
- Collimated beams preserve fluence across depth; misalignment reduces energy density at target tissues.
- Stable respiratory movement and muscle tone affect microtargeting of facets, interspinous ligaments, and paraspinal myofascia. Comfortable patients move less, ensuring reliable dosing.
- Direct skin contact improves photon coupling for the handheld diode, reducing interface losses and aiding precise delivery to nociceptive and myofascial triggers.
Integrative Chiropractic Care: Mapping Pain Generators and Connective Tissue
Laser therapy is powerful, but it works best when guided by a skilled structural evaluation, which I refine within integrative chiropractic care:
- I begin with:
- Facet loading tests and segmental palpation to identify painful motion segments (e.g., L4–L5 facets producing unilateral right-sided pain).
- Trigger point mapping using the tactile distinction between supple muscle and firm nodules—the so-called “cooked meat vs. raw meat” analogy, which helps describe hypertonic bands amidst pliable tissue.
- Regional fascial continuity assessment, because pain seldom lives in isolation. Engaging paraspinal fascia, thoracolumbar fascia, and gluteal connective tissue can reduce compensatory strain.
- Why this matters:
- Trigger points harbor sensitized nociceptors and metabolically stressed fibers; laser’s photobiomodulation supports local ATP recovery and neurochemical modulation.
- Facet irritation is inflammatory and mechanical; improving microcirculation and reducing inflammatory mediators supports the tissue, while chiropractic care restores segmental mechanics.
- Global connective-tissue engagement changes load distribution; laser helps soften densified fascia, and adjustments re-coordinate how forces travel through the spine and pelvis.
Robotic and Handheld: A Clinical Multimodal Approach
- Modern MLS platforms often include:
- A robotic head delivering synchronized dual wavelengths over a defined X–Y treatment field.
- A handheld diode for highly focused points.
- Workflow:
- I zero the X–Y axes on the robotic interface to center the primary pain site. Then I expand the field to include adjacent connective tissue, adopting a global, multisite approach.
- The robot treats the broader region for 6–12 minutes, while I concurrently apply the handheld to discrete trigger points for 20–30 seconds each.
- Why this dual approach:
- Robotic fields ensure uniform density over larger areas, improving consistency in paraspinal tissues.
- Handheld punctual dosing adds specificity for trigger points, tender facets, or periarticular zones—ideal when patient movement (guided breathing or gentle mobilization) enhances the therapeutic effect.
- Treating both the source and the surrounding network supports load-sharing and reduces recurrences.
Dosimetry: Energy Density vs. Total Joules
Laser dosing must be clinical and quantitative. The most robust standard in the literature is energy density, measured in joules per square centimeter (J/cm²), rather than total joules. A typical effective window for musculoskeletal tissues is 4–10 J/cm², depending on the condition, acuity, and depth (World Association for Laser Therapy guidance and subsequent studies emphasize dose per area as the key benchmark).
- Practical dosing:
- For low back pain with facet irritation, I often target 6 J/cm² to start, adjusting based on response and tissue characteristics.
- Total joules will scale with the treatment field size, but the software should auto-recalculate time when you enlarge or shrink the X–Y field to deliver the desired J/cm² without manual math.
- Why density matters:
- Cellular photobiomodulation follows a biostimulatory window; too little energy fails to trigger meaningful cascades, too much can provoke bioinhibition (Arndt-Schulz law).
- Dose per area ensures consistent tissue response independent of field size, improving reproducibility.
Pulse Structure, Power, and Heat Management
Modern MLS devices often use high peak power (e.g., up to 50 W) but short pulse durations, synchronized with continuous 808-nm light. This design delivers high photon flux to deeper tissues without excessive surface heating.
- Physiology of pulsing:
- Short pulses drive photons deeper before heat builds at the surface; inter-pulse rest periods allow thermal relaxation and energy absorption without temperature creep.
- 808-nm continuous-wave light supports steady photobiomodulation at the muscle and connective tissue levels.
- 905-nm pulsed complements penetration and neuromodulatory effects at nociceptive fibers and microvasculature.
- Clinical takeaway:
- If a patient reports heat at the surface, reassess wavelengths, pulse parameters, and dose. Correctly calibrated systems should maintain tissue temperature over time, indicating safe energy delivery.
Treatment Timing and Response Expectations
A single session may produce a delayed-onset analgesia window—often noticeable 4–6 hours post-treatment. In my clinic, I ask patients to check functional tests later that day (for example, bending or walking at 17:00 if the session was at 11:00). Early improvements after one session are common. Still, cumulative effects emerge over a short course.
- Typical course:
- Acute conditions: ~6 sessions over 2 weeks.
- Chronic conditions: ~12 sessions over 3–4 weeks.
- Spacing: Minimum 24 hours between sessions; realistic schedules often have a Monday–Wednesday–Friday cadence.
- Why cumulative dosing matters:
- Photobiomodulation signals alter gene expression, cytokine profiles, and mitochondrial function over time. Repetition consolidates tissue-level changes and neural recalibration.
Knee Osteoarthritis: Targeting Compartments and Patellar Reflection
For knee OA, positioning is crucial:
- With the knee flexed, avoid direct anterior-only beams that reflect off the patella. Include posterior and medial/lateral compartments.
- Dose by compartmental area, maintaining the target J/cm² per treated field. If multiple compartments are indicated, treat each field to the appropriate density rather than arbitrarily summing total joules.
- Physiological reasoning:
- OA involves synovial inflammation, cartilage stress, capsular fibrosis, and periarticular trigger points. Laser supports microcirculation, inflammatory modulation, and analgesia while integrative chiropractic care addresses hip-knee-ankle mechanics and gait re-education.
- You will not reverse bone-on-bone structurally with laser alone; however, you can delay symptom progression, reduce flares, and restore daily function.
Bone Healing and Fractures: Off-Label Considerations
While laser therapy for bone healing may be considered off-label in certain jurisdictions, clinicians have reported benefits when it is initiated within 7–10 days post-fracture, during the inflammatory phase. The rationale:
- Early photobiomodulation may support angiogenesis, osteoblastic signaling, and the orchestration of inflammation that favors callus formation.
- Nonunion fractures are far more complex, often requiring surgical or biologic intervention; lasers may not reliably correct nonunion but can be adjunctive in multimodal plans.
Always align with local regulations and informed consent, and document the intended therapeutic goals. My personal practice emphasizes the inflammatory-window strategy in conjunction with orthopedic guidance and imaging follow-up.
Combining MLS Laser with Orthobiologics: PRP Protocols
Laser therapy can complement PRP via tissue priming, peri-injection modulation, and post-injection support:
- A progressive protocol I employ:
- Pre-injection: 2–3 laser sessions to prime local microcirculation, reduce baseline inflammatory noise, and enhance cellular redox readiness.
- Day of injection: Adjust parameters to limit immediate pain and support controlled inflammatory signaling essential for PRP efficacy (do not blunt the pro-inflammatory phase; aim to augment coordinated inflammation, not suppress it).
- Post-injection: ~6 sessions over 2–3 weeks to optimize ATP availability, fibroblast activity, and matrix remodeling while managing pain.
- Evidence trends:
- Emerging clinical observations suggest additive efficacy when a laser is layered over PRP compared with PRP alone, with improved pain and functional scores in musculoskeletal cohorts (see references).
- Why integrative chiropractic care helps here:
- I use segmental stabilization, mobility drills, and neuromuscular retraining to direct the newly remodeled tissue toward efficient movement patterns. This reduces aberrant load and helps preserve PRP gains.
Acute vs. Chronic Effects: Mapping the Physiological Cascade
Laser therapy acts on multiple levels, often concurrently. For clarity, think in phases:
- Immediate to short-term (minutes to hours):
- Analgesia via modulation of small myelinated fibers and C-fiber signaling.
- Changes in ion channel activity and neurogenic inflammation.
- Early microcirculatory shifts with vasomotor influences.
- Subacute (days):
- Inflammatory modulation: Downregulation of pro-inflammatory cytokines (e.g., TNF-α, IL-1β), upregulation of anti-inflammatory mediators (e.g., IL-10) in line with photobiomodulation literature.
- Edema reduction through improved lymphatic flow and endothelial function.
- Mitochondrial activation: Cytochrome c oxidase absorbs photons, increasing ATP production, ROS signaling at hormetic levels, and transcriptional responses that promote recovery.
- Remodeling (weeks):
- Enhanced fibroblast proliferation, collagen deposition, and matrix organization in ligaments and fascia.
- Neural plasticity shifts that reduce central sensitization, reinforced by targeted rehab and chiropractic neuromechanical inputs.
Optimizing Mitochondrial Support: Clinical Considerations
Many patients take medications (e.g., certain statins) that can influence mitochondrial function. In my practice, I support mitochondrial resilience ethically and collaboratively:
- Nutritional and lifestyle adjuncts:
- Consider coenzyme Q10, creatine (phosphate donor), nicotinamide riboside/NMN for NAD+ support, and dietary polyphenols that moderate oxidative stress.
- Encourage sleep optimization, glycemic control, and anti-inflammatory nutrition to support mitochondrial biogenesis and redox balance.
- What laser adds:
- Photobiomodulation directly enhances electron transport chain efficiency, increasing ATP while moderating ROS within a hormetic range that drives adaptive signaling.
- These effects dovetail with targeted supplementation and therapeutic exercise, potentially offsetting medication-related mitochondrial stress.
- Practical caution:
- Always individualize adjuncts based on medical history and coordinate with the patient’s primary physician or pharmacist. Laser is nonpharmacologic, but co-therapies require medical oversight.
Integrative Chiropractic Care During Laser Courses
Laser therapy is not a standalone panacea. A mechanically intelligent plan reduces recurrence:
- Segmental and regional adjustments:
- Gentle high-velocity, low-amplitude or low-force mobilizations restore facet glide, disc-friendly mechanics, and neural mobility.
- Pelvic and hip alignment improve load transfer to the knee and spine.
- Soft-tissue integration:
- Myofascial release aligns collagen fibers, enabling laser-softened tissues to remodel along the correct lines of tension.
- Neuromuscular re-education—gluteal activation, core endurance, posterior chain drills—transforms pain relief into durable movement patterns.
- Reasoning:
- Laser modulates biology; chiropractic care organizes biomechanics. Together, they create a bio-mech synergy that outperforms isolated treatments.
Safety, Durability, and Service
Modern MLS systems are designed for on-site reliability with field-service support, avoiding shipping risks. Typical issues are rare after installation, and comprehensive training sets teams up for success.
- Patient sensations:
- Most patients feel no pain during treatment; some report mild warmth or tingling. If sensitive, reassure and re-check parameters; small sensations are within normal expectations when dosing within the therapeutic window.
- Maintenance:
- Keep optics clean, verify focal distance with the ruler, and routinely check software calibration. Follow manufacturer service intervals.
Explaining Energy Dosing to Patients: Clear Communication
Patients often ask about total joules. I explain that we focus on energy density (J/cm²) because tissues respond to dose per area, not raw totals. The software automatically adjusts the time when we change the treatment area, so they receive a consistent, science-based dose tailored to their condition.
Trigger Point Strategy: Why Punctual Application Works
When I palpate a trigger point, I often apply the handheld diode for 20–30 seconds per spot, moving across a map of nodules discovered on exam:
- Mechanisms:
- Local ATP restoration aids sarcomere relaxation in taut bands.
- Substance P and calcitonin gene-related peptide (CGRP) signaling can be moderated, reducing local neurogenic inflammation.
- Microvascular perfusion improves in the endplate zone of dysfunctional motor units.
- Practice tip:
- Combine with breathing cues, gentle contract-relax techniques, or post-irradiation eccentrics to lock in improved tone.
Shockwave, Laser, and PRP: Coordinating Modalities
In clinics that rely on shockwave therapy, we coordinate timing to leverage mechanotransduction and photobiomodulation:
- Typical sequence:
- Use shockwave to provoke controlled micro-disruption and stimulate regenerative signaling.
- Apply laser to augment mitochondrial activity, reduce excessive inflammatory noise, and improve perfusion.
- Integrate PRP with pre- and post-laser treatments, as described, to layer biologic potential atop mechanically and metabolically optimized tissue.
- Rationale:
- Mechanotransduction + photobiomodulation + biologics equals a triad of healing: mechanical cueing, bioenergetic support, and cellular supply.
Exploring Integrative Medicine- Video
Clinical Observations from My Practice
In my clinics and collaborations, I consistently see:
- Low back facet pain responds within the first week, with functional gains evidenced by improved tolerances to extension and rotation.
- Knee OA patients reporting better stair negotiation and reduced morning stiffness after 6–12 sessions, especially when hip stability and foot mechanics are concurrently addressed.
- Post-PRP recovery with faster pain control and an earlier return to graded activity when the laser is layered per protocol.
- Patient adherence improves when the plan is explained as a stepwise journey with cumulative benefits, rather than a single miracle session.
For further details on my approach and outcomes, you can explore my clinical observations and frameworks on my professional pages:
Putting It All Together: A Practical Treatment Blueprint
- Intake and exam:
- Identify pain generators (facet, ligamentous strain, trigger points), movement faults, and red flags.
- Dosing plan:
- Choose 4–10 J/cm², start around 6 J/cm² for common spine and joint cases, adjust per response and acuity.
- Position and align:
- Prone setup for low back; flexed knee for OA with posterior and compartmental coverage; verify 6-inch focal distance for robotic heads.
- Deliver multimodal therapy:
- Robotic field for broad tissue coverage; handheld diode for punctual trigger points and joint spaces.
- Chiropractic integration:
- Segmental adjustments, myofascial release, and neuromuscular drills during the laser course for lasting change.
- Orthobiologic layering:
- PRP with 2–3 pre-injection sessions, day-of session modulated for supportive effects, and ~6 post-injection sessions.
- Scheduling:
- Acute: ~6 sessions; Chronic: ~12 sessions, spaced by ≥24 hours, often three per week.
- Reassessment:
- Functional tests at 4–6 hours post-treatment on the first day; weekly progress checks; adjust parameters or fields as needed.
Final Thoughts: Precision, Patience, and Integration
The best outcomes come from precision dosing, patient comfort, and integrated care. MLS laser therapy is a potent tool when used with a systems mindset—connective tissue mapping, segmental mechanics, mitochondrial support, and thoughtful protocols. Patients appreciate that the plan is clear, the science is sound, and the results are cumulative. With a compassionate, evidence-based approach, you can reliably reduce pain, restore movement, and improve quality of life.
References
- World Association for Laser Therapy (WALT) treatment recommendations: Photobiomodulation dose guidelines (WALT, n.d.)
- Therapeutic photobiomodulation: mechanisms and applications (Hamblin, M. R., 2017)
- The role of cytochrome c oxidase in photobiomodulation (Karu, T. I., 2008)
- Photobiomodulation for musculoskeletal pain: systematic review and meta-analytic perspectives (Chow, R., 2020)
- Optimizing PRP outcomes with adjunct therapies: emerging evidence (Filardo, G., 2018)
- Arndt-Schulz law and bioinhibition in dose-response to photobiomodulation (Huang, Y-Y., 2016)
In-text citation examples:
- WALT dosing windows emphasize targeting 4–10 J/cm² for musculoskeletal tissues (WALT, n.d.).
- Photobiomodulation acts via cytochrome c oxidase, improving ATP and signaling cascades (Karu, 2008; Hamblin, 2017).
- Systematic reviews support analgesic and anti-inflammatory effects across musculoskeletal pain conditions (Chow, 2020).
- Adjunctive strategies with PRP may enhance outcomes compared to PRP alone in select cohorts (Filardo, 2018).
- Dose discipline avoids bioinhibition, consistent with Arndt-Schulz principles (Huang, 2016).
SEO tags
MLS laser therapy, photobiomodulation, integrative chiropractic care, low back pain, facet joint pain, knee osteoarthritis, PRP integration, orthobiologics, trigger points, energy density J/cm2, 808 nm, 905 nm pulsed laser, mitochondrial function, microcirculation, chiropractic adjustments, shockwave therapy, pain management, rehabilitation, Arndt-Schulz law, WALT guidelines
Post Disclaimer
General Disclaimer, Licenses and Board Certifications *
Professional Scope of Practice *
The information herein on "Understanding Therapeutic Approaches for Tissue Regeneration with Photobiomodulation" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those on this site and on our family practice-based chiromed.com site, focusing on naturally restoring health for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine; wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics; subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and facilitate clinical collaboration with specialists across disciplines. Each specialist is governed by their professional scope of practice and licensure jurisdiction. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that directly or indirectly relate to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
(Board Certified: Family Practice Nurse Practitioner—Multistate)*
(Licensed Nurse Practitioner & Chiropractor - Multistate)*
Clinical Director
Digital Business Card
Dr. Maria Cardenas, MD
(Board Certified: Internal Medicine)
(Licensed Medical Doctor)
Medical Director, Clinical Director & Collaborative Physician
NPI # 1164426749
MD License #: J2933
Licenses and Board Certifications:
MD: Medical Doctor
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
(Board Certified: Family Practice Nurse Practitioner—Multistate)*
(Licensed Nurse Practitioner & Chiropractor - Multistate)*
Clinical Director
Digital Business Card
Dr. Maria Cardenas, MD
(Board Certified: Internal Medicine)*
(Licensed Medical Doctor)*
Medical Director, Clinical Director & Collaborative Physician
NPI # 1164426749
MD License #: J2933
📆 Schedule Appointment: Schedule 24/7 (Click Here)