Personal Injury and Work Injury Recovery in El Paso

Abstract
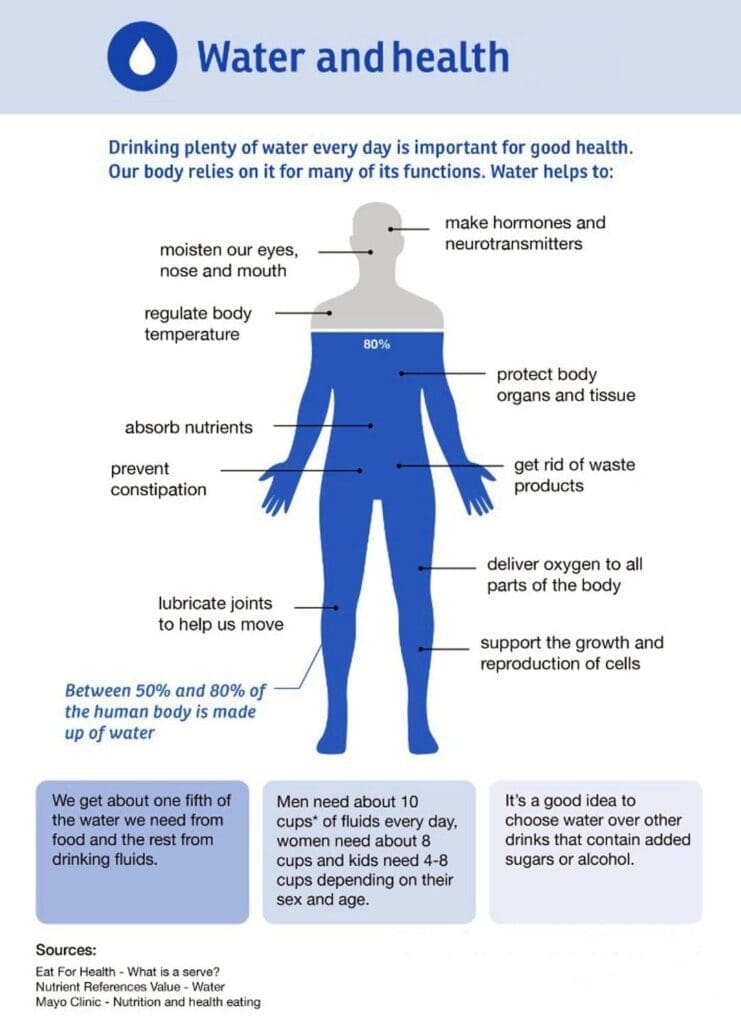
Personal and work injuries such as whiplash, muscle strains, and slips and falls often leave people in pain, stiff, and unable to move freely. In this article, Dr. Alex Jimenez, DC, APRN, FNP-BC, CFMP, IFMCP, ATN, CCST, shares how integrative chiropractic care at ChiroMed Integrated Medicine in El Paso helps patients achieve full recovery. The clinic combines gentle chiropractic adjustments, functional medicine, rehabilitation exercises, nutritional counseling, and even acupuncture and naturopathy to treat the whole person. Instead of just covering up symptoms, this approach identifies and addresses the root causes of pain so patients regain mobility, improve their daily movement, and heal faster. Readers will discover the latest science-backed methods, why personal injury attorneys trust evidence-based clinics like ChiroMed, and how tools such as therapeutic ultrasound support both healing and strong legal records. Follow this clear journey from injury to lasting wellness.
The Hidden Toll of Personal and Work Injuries
Every day in El Paso, people get hurt in car crashes, on the job, or from simple slips and falls. Whiplash occurs when the head jerks forward and backward suddenly, stretching neck muscles and ligaments and irritating spinal nerves. Strains happen when muscles or tendons tear slightly, causing swelling, weakness, and sharp pain. Slips and falls can jolt the lower back or hips, knocking joints out of alignment and pinching nerves that control movement and feeling.
Inside the body, these injuries trigger inflammation—a natural defense system that rushes blood, fluids, and immune cells to the damaged area to begin repair. At first, this helps, but if inflammation lingers, it builds scar tissue that feels tight and weak. Nerves running along the spine get compressed, sending constant pain signals to the brain and slowing normal healing. Without the right care, people lose their ability to move easily, struggle to sleep, and feel tired all the time. At ChiroMed Integrated Medicine, integrative chiropractic care changes this pattern by treating the entire body system, not just one sore spot. This whole-person method restores balance and speeds true recovery.
Why Integrative Chiropractic Care Stands Out in El Paso
Many clinics focus only on quick pain relief with pills or surgery. ChiroMed Integrated Medicine takes a smarter, more complete route. Located at 11860 Vista Del Sol Dr, Suite 128 in El Paso, the clinic blends four (and more) proven tools:
- Gentle chiropractic adjustments
- Functional medicine lab testing
- Targeted rehabilitation
- Nutritional counseling plus naturopathy and acupuncture
This integrative chiropractic care approach looks at the root cause—misaligned spine, ongoing inflammation, poor nutrition, hidden stress, or even hormone imbalances—rather than treating symptoms alone. Dr. Alex Jimenez and his multidisciplinary team create plans tailored to each patient because no two injuries or bodies are exactly alike. The goal is clear: restore natural movement, ease pain without drugs when possible, and help patients return to work and everyday life with strength and confidence. Since 1996, ChiroMed has built a reputation for honest, patient-centered care that combines conventional and natural methods for the best results.
How Chiropractic Adjustments Restore Spinal Alignment and Mobility
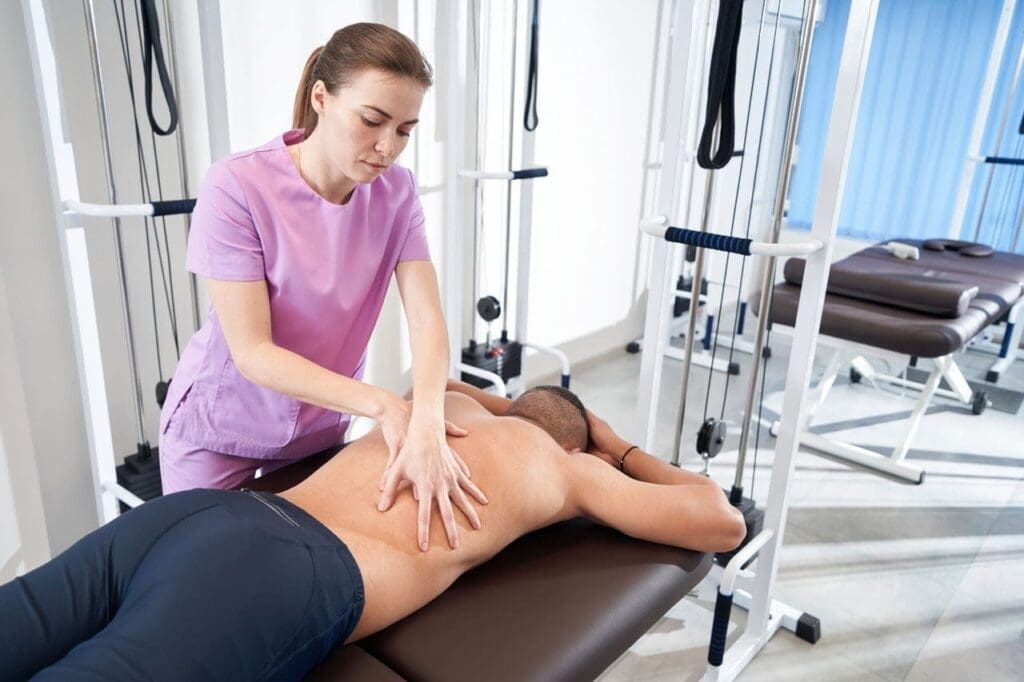
A chiropractic adjustment is a safe, controlled movement that gently guides a joint back into its correct position. After whiplash, neck bones often shift and press on nearby nerves. The adjustment releases that pressure, which quickly lowers the pain signals racing to the brain.
On a deeper level, proper alignment boosts blood flow to injured tissues, relaxes over-tight muscles that have been guarding the area, and lets spinal discs cushion shocks again. Tiny sensors called mechanoreceptors in the joints wake up and send “everything is safe” messages to the nervous system, calming the body’s pain pathways. Patients at ChiroMed often notice they can turn their heads more easily, wake up with less morning stiffness, and stand taller within just a few weeks. Adjustments are always paired with soft-tissue techniques, so muscles stay relaxed around the newly balanced spine. This step is key because a misaligned spine keeps sending wrong signals that slow healing.
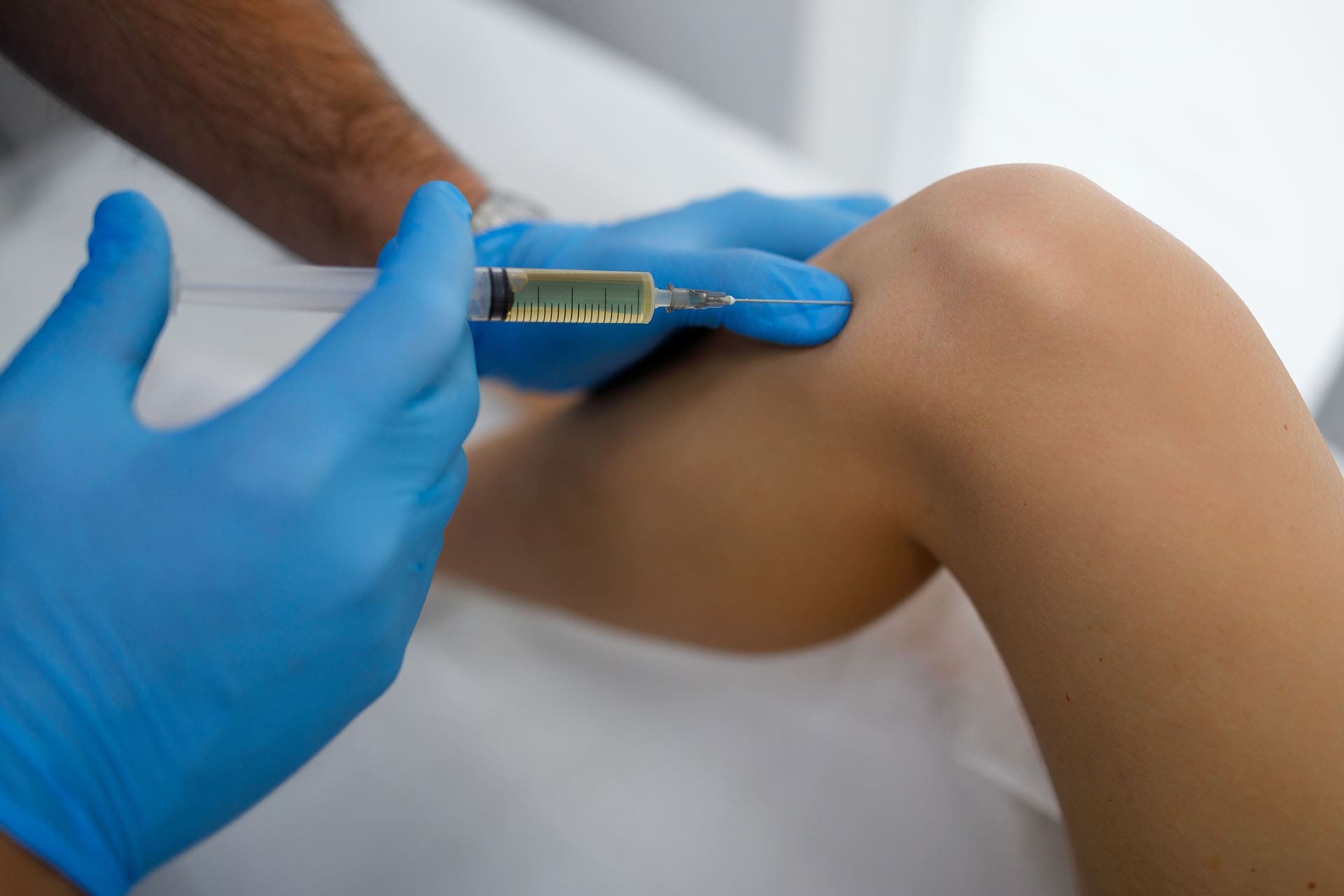
The Power of Functional Medicine: Finding and Fixing Root Causes
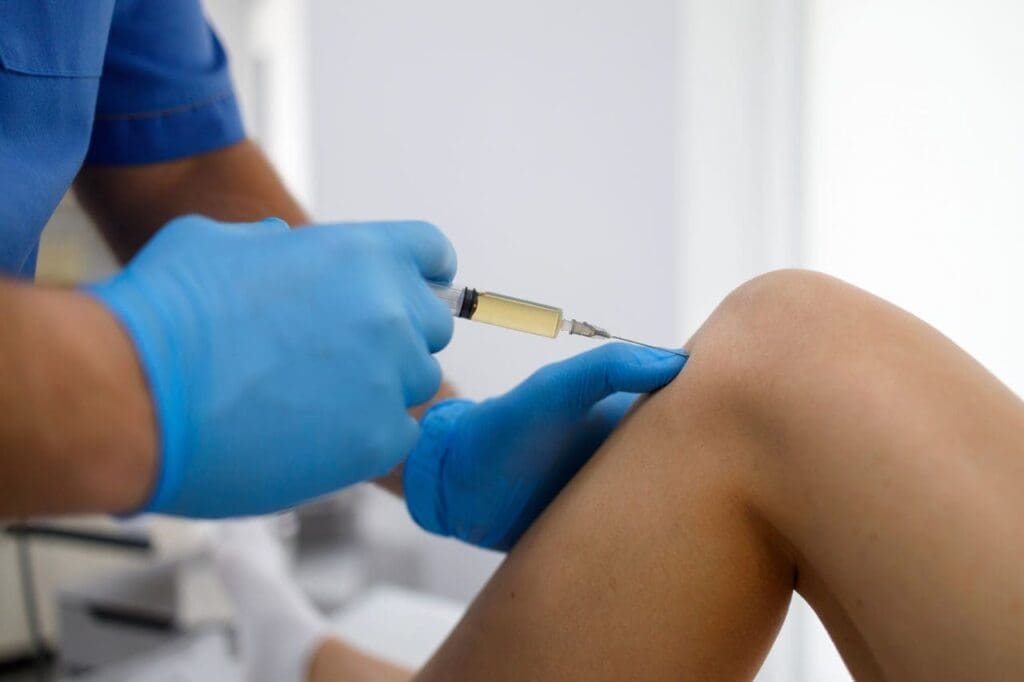
Functional medicine at ChiroMed goes beyond the visible injury. Dr. Jimenez uses advanced blood tests and assessments to uncover hidden problems such as low vitamin levels, elevated inflammatory markers, blood sugar ups and downs, or even stress hormones that keep the body stuck in repair mode. Poor nutrition or ongoing worry can trap tissues in a “fight-or-flight” state, blocking full recovery.
By correcting these root issues, healing speeds up dramatically. Balanced nutrients reduce swelling, targeted supplements rebuild damaged cartilage and nerves, and naturopathic support calms the whole system. This explains why some patients bounce back quickly while others struggle—ChiroMed finds the “why” behind slow healing and offers lasting solutions rather than temporary fixes.
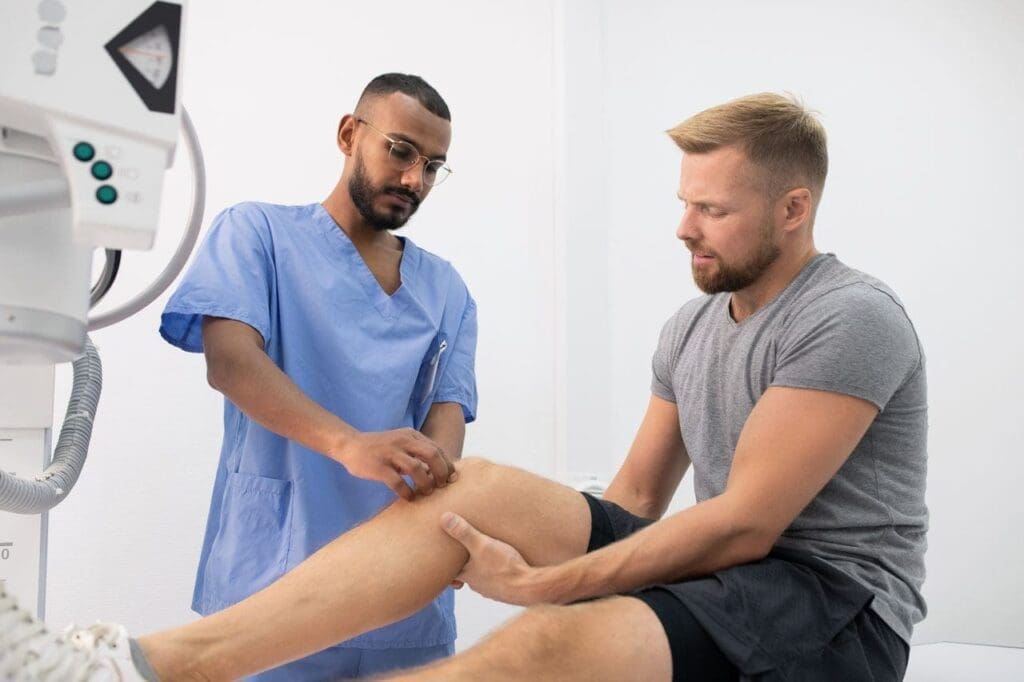
Rehabilitation Exercises That Rebuild Strength and Functional Movement
Rehabilitation at ChiroMed is never guesswork. The team uses precise assessments, including motion analysis and nerve tests, to identify exactly which muscles are weak or overly tight after injury. Patients then follow safe, guided exercises that build balance, core power, and smooth flexibility.
Why is this so important? Injured areas often heal with stiff, weak scar tissue that limits motion. Targeted movements gently break down poor scar tissue patterns and retrain muscles to support the spine as they were meant to. Over time, patients regain the ability to bend, lift, twist, and walk without worry of re-injury. The real win is functional movement—everyday motions that let people safely and confidently return to work, hobbies, and family life.
Nutritional Counseling and Naturopathy: Fueling the Body’s Natural Repair System
Food truly acts as medicine after an injury. The body suddenly needs more protein to rebuild tissues, anti-inflammatory foods to quiet swelling, and key nutrients like omega-3 fats to protect nerves and joints. At ChiroMed, Dr. Jimenez’s team creates personalized meal plans and high-quality supplements based on each patient’s lab results.
Patients learn simple, doable changes—such as adding leafy greens to fight inflammation, choosing lean proteins to repair muscle, or using naturopathic herbs to support natural detoxification and healing. These steps reduce pain without extra medication and provide the body with the exact building blocks needed for faster tissue repair. Many people at the clinic report higher energy, fewer flare-ups, and better sleep once nutrition and naturopathy are dialed in.
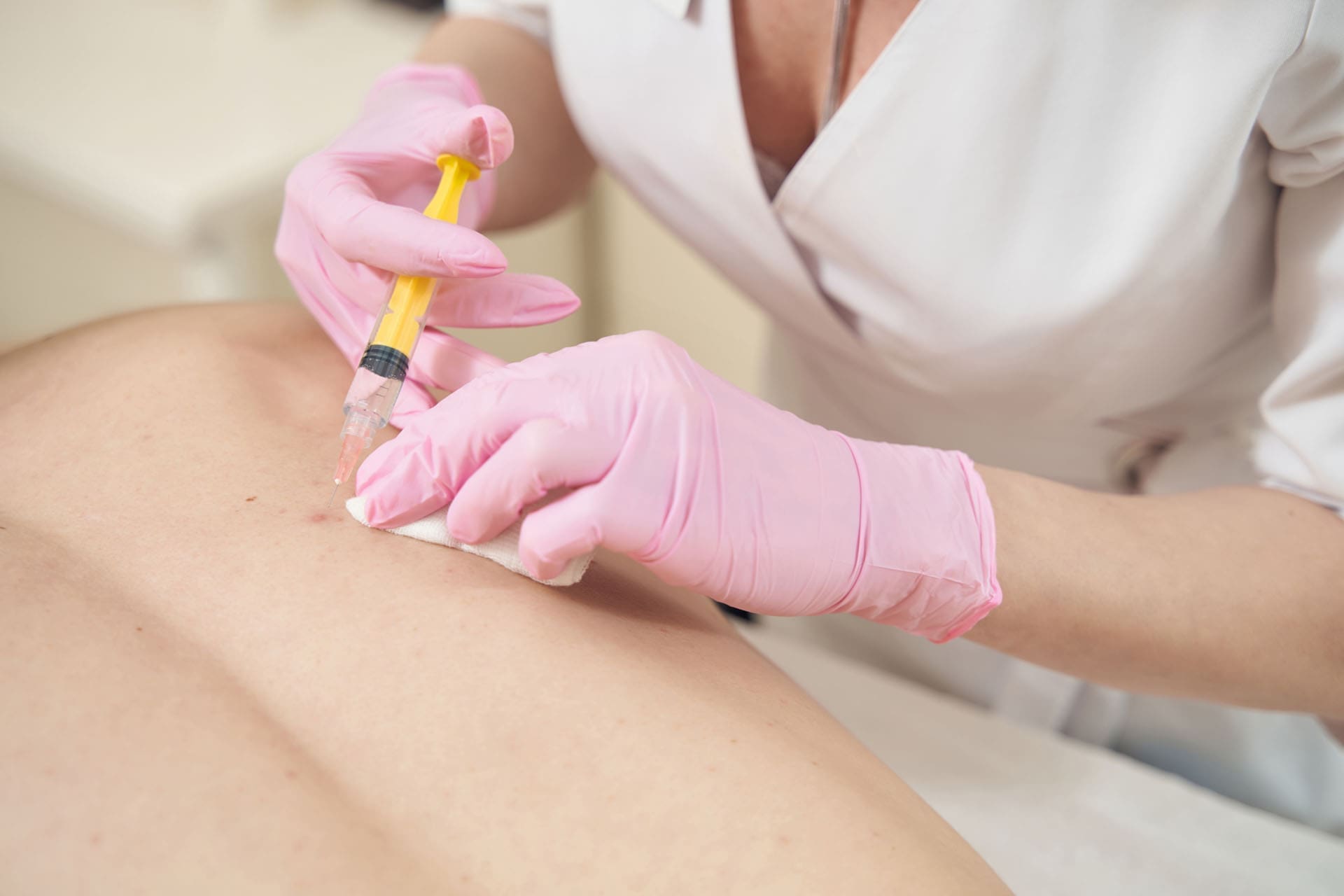
Therapeutic Ultrasound: Deep Healing for Soft Tissues and Strong Legal Documentation
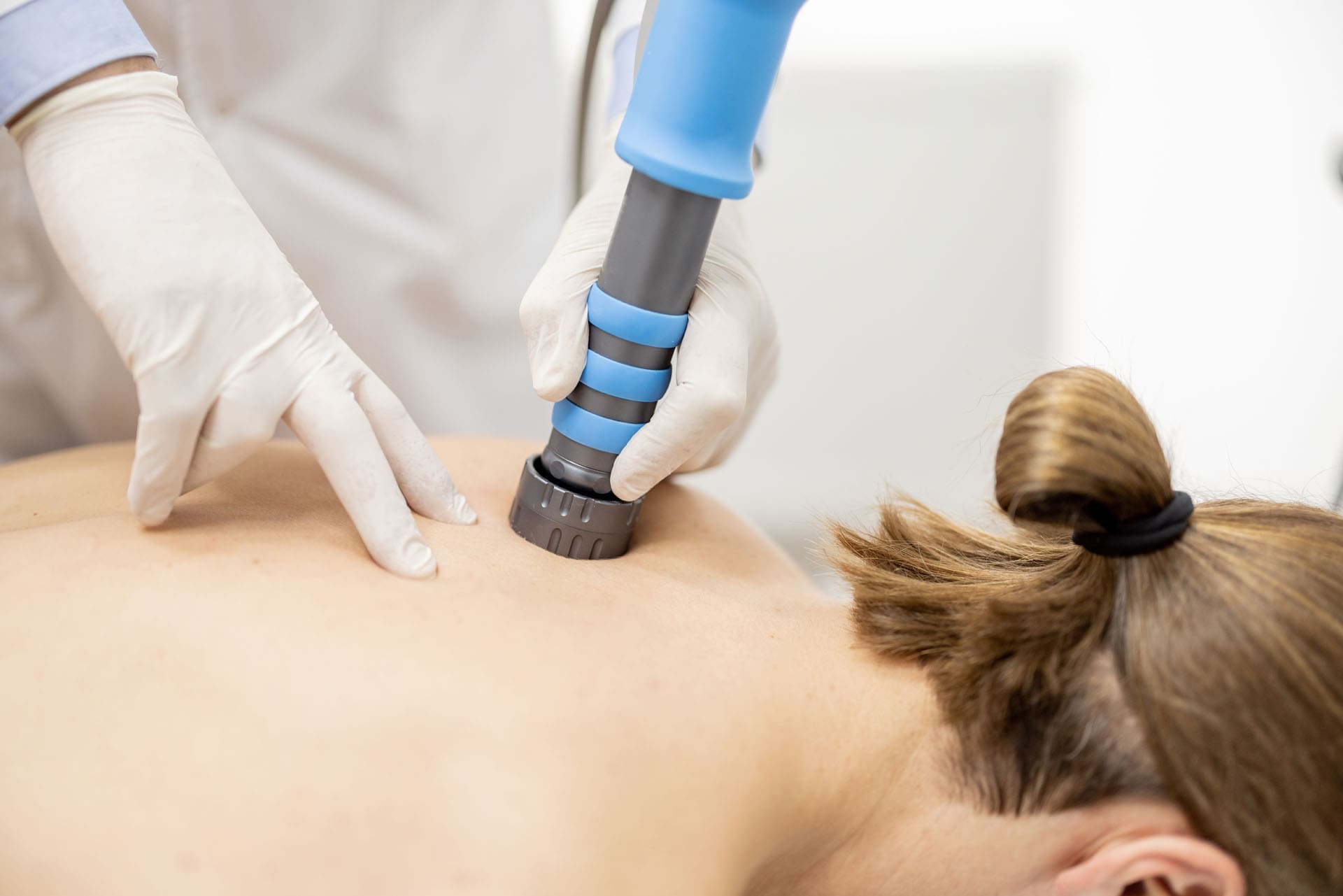
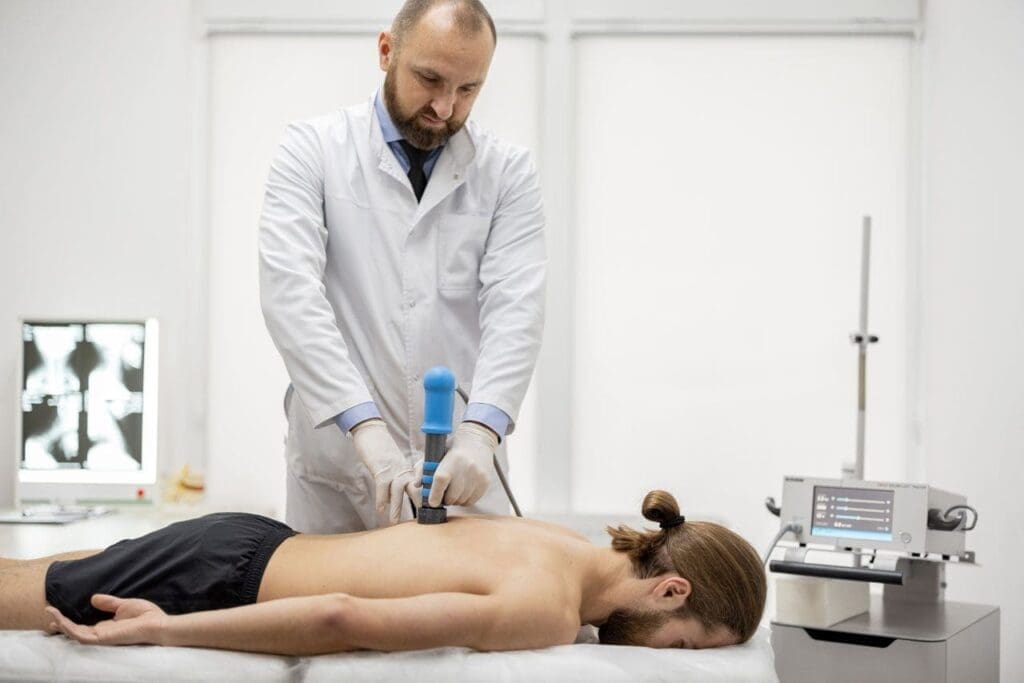
Therapeutic ultrasound is a gentle, drug-free tool that sends sound waves (usually 1 or 3 MHz) deep into muscles, ligaments, and tendons. These waves create a warming effect and tiny bubbles called cavitation that massage cells from the inside. The result? Better blood flow, relaxed tight muscles, reduced swelling, and softer scar tissue that moves more freely.
For whiplash and strains, ultrasound calms inflamed areas so chiropractic adjustments work even better, and rehabilitation exercises feel easier. ChiroMed uses it because it is safe, measurable, and produces clear progress notes documenting improvement. Personal injury attorneys especially appreciate this objective evidence when dealing with insurance companies.
Why Personal Injury Attorneys Seek Evidence-Based Chiropractic Providers
Personal injury (PI) attorneys need clear, trustworthy medical proof to win fair settlements for their clients. They look for clinics that use evidence-based modalities such as therapeutic ultrasound, detailed imaging, and complete progress notes. These records prove the injury was real, the treatment was medically necessary, and recovery is on track.
Many attorneys keep lists of trusted local providers who put patient needs first. Reputable lawyers ensure clients choose care based on what the body actually requires, not just on fast referral relationships. This careful choice protects against insurance challenges and builds the strongest possible case.
How Attorneys and Chiropractors Build Strong, Ethical Partnerships
Professional networks, peer recommendations, and a shared focus on accident-related spinal trauma bring attorneys and ChiroMed together. The clinic supplies clear documentation of spinal trauma, treatment timelines, and functional limitations. Attorneys then use these detailed records to prove damages and negotiate the best compensation.
The partnership works for everyone: patients receive excellent, root-cause care while lawyers get accurate evidence needed for court or settlement talks. Both sides stay focused on honest, necessary treatment that truly helps the injured person get better.
Avoiding Settlement Mills: Choosing Quality Care Over Quick Fixes
Some people worry about “settlement mills”—clinics that push extra visits to raise bills and rush low settlements. Ethical attorneys and doctors at places like ChiroMed warn against these shortcuts. Instead, they carefully choose providers who base every decision on the patient’s real medical needs.
Patients should feel sure their care plan comes from what will help them heal, not from outside pressure. ChiroMed focuses on long-term wellness and evidence-based results rather than short-term financial gains.
Clinical Observations from Dr. Alex Jimenez
In my dual-scope practice as both a chiropractor and advanced practice nurse practitioner, I have witnessed powerful recoveries at ChiroMed. Patients who arrive with severe whiplash after car accidents often regain full neck motion in weeks when adjustments, ultrasound, functional medicine, and nutrition work as a team. Work-injury cases with repetitive strains improve dramatically once we correct underlying inflammation and muscle imbalances.
Our use of advanced imaging and whole-body assessments helps us catch hidden factors that other clinics might miss. People leave our clinic not only pain-free but stronger, with practical tools to prevent future problems. The collaborative model at ChiroMed—linking chiropractic, nurse practitioner services, naturopathy, acupuncture, and rehabilitation—ensures every patient receives exactly the care they need.
Modern Tools and Support Making Recovery Easier
Today’s patients at ChiroMed can continue their care through convenient options that keep progress steady and records complete for legal needs. The clinic’s comfortable environment and multidisciplinary team make the healing journey feel supportive from the very first visit.
Conclusion
Integrative chiropractic care at ChiroMed Integrated Medicine in El Paso offers a clear, science-backed path from injury pain to full, lasting recovery. By combining spinal adjustments, functional medicine, rehabilitation, nutritional counseling, naturopathy, acupuncture, and advanced tools such as therapeutic ultrasound, the clinic treats the whole person and addresses root causes. Whether recovering from whiplash, muscle strains, or work-related falls, patients regain mobility, calm inflammation, and return to life stronger than before. Personal injury attorneys trust ChiroMed because its records are thorough, its care is ethical, and its outcomes are real.
If you or someone you love has been hurt in an accident or at work, consider reaching out to ChiroMed. The road to feeling better starts with understanding your body’s natural healing power—supported by modern, compassionate, evidence-based care. Visit https://chiromed.com/ or call (915) 412-6680 to start your personalized recovery journey today.
References
ChiroMed. (n.d.). ChiroMed – Integrated Medicine Holistic Healthcare in El Paso, TX. https://chiromed.com/ ChiroMed. (n.d.).
Chiropractor El Paso, TX. https://chiromed.com/services/chiropractor-el-paso-tx/
ChiroMed. (2025, August 25). El Paso personal injury chiropractor. https://chiromed.com/tag/el-paso-personal-injury-chiropractor/
ChiroMed. (2025, July 15). El Paso personal injury care. https://chiromed.com/tag/el-paso-personal-injury-care/ ChiroMed. (n.d.).
Chiropractic and nurse practitioner for injury recovery. https://chiromed.com/chiropractic-and-nurse-practitioner-for-injury-recovery/
Personal Injury Doctor Group. (n.d.). Injury specialist. https://personalinjurydoctorgroup.com/ Dr. Alex Jimenez. (n.d.).
Why choose Dr. Jimenez and clinical team. https://dralexjimenez.com/why-choose-dr-jimenez-and-clinical-team/ Cagle Firm. (2024).
Personal injury settlements & chiropractic care in Texas 2024. https://www.caglefirm.com/resources/automobile-accidents/personal-injury-settlements-chiropractic-care-in-texas-2024-cpm-injury-law
Blackwell Attorneys. (n.d.). Should I let a lawyer send me to his chiropractor or doctor? https://blackwell-attorneys.com/blog/should-i-let-a-lawyer-send-me-to-his-chiropractor-or-doctor/
Anderson Personal Injury Chiropractic. (n.d.). Therapeutic ultrasound. https://www.personal-injury-albany.com/therapeutic-ultrasound