Platelet-Rich Plasma (PRP) Therapy for Spinal Care

Integrated Medicine: Natural Healing Without Surgery in El Paso
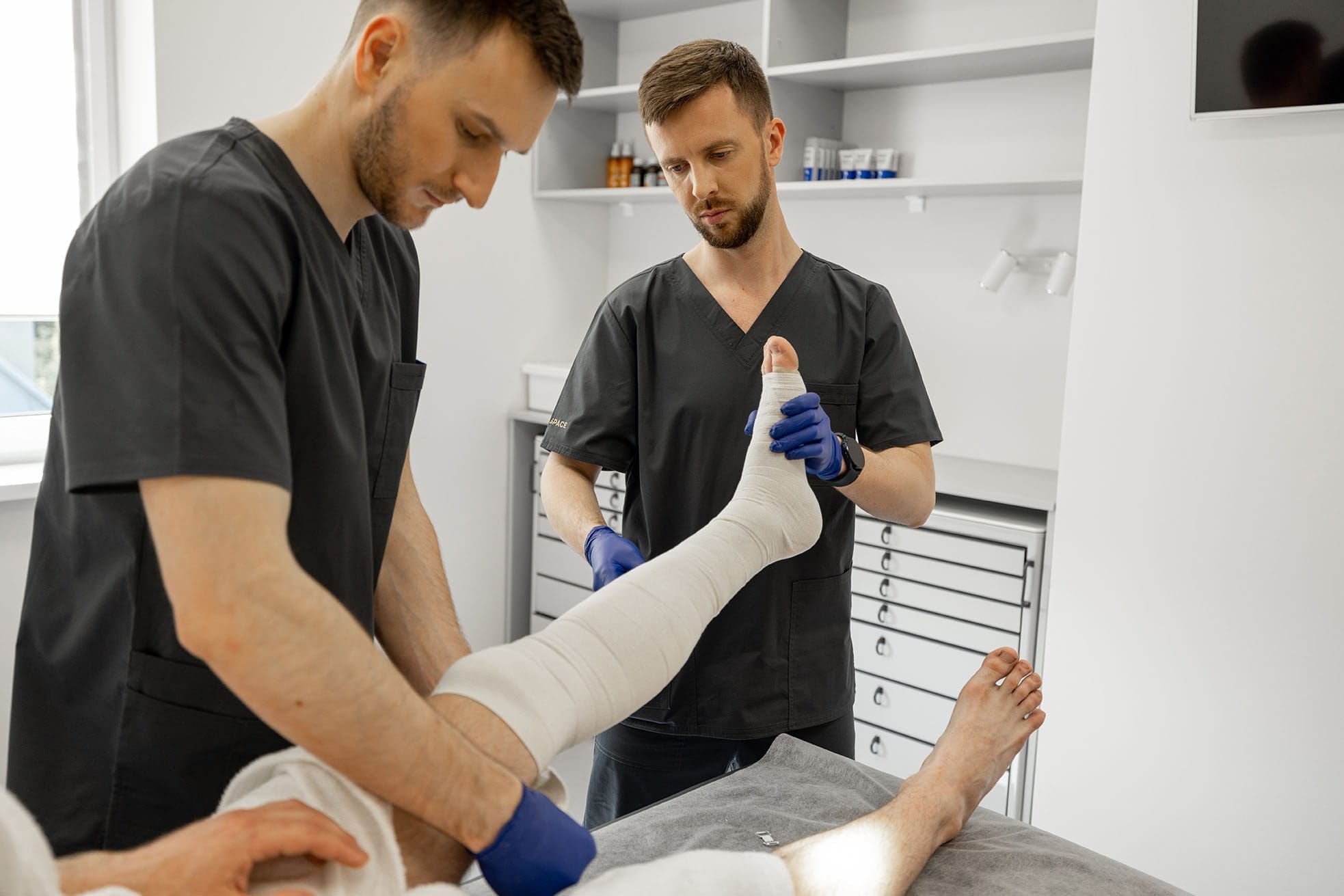
Spinal problems touch the lives of millions every year. Many people deal with ongoing back pain caused by worn discs, irritated facet joints, or weakened ligaments. At ChiroMed Integrated Medicine in El Paso, Texas, Platelet-Rich Plasma (PRP) therapy supports spinal care by using a person’s own platelets to reduce inflammation and promote healing of damaged discs, facet joints, and ligaments. This minimally invasive method releases growth factors that help tissue recover without surgery, thereby decreasing chronic pain and increasing mobility. People with mild to severe spinal degeneration who have not found enough relief from conservative treatments like physical therapy often turn to PRP at ChiroMed. (ChiroMed, n.d.-a)
What Is PRP Therapy and How Does ChiroMed Use It?
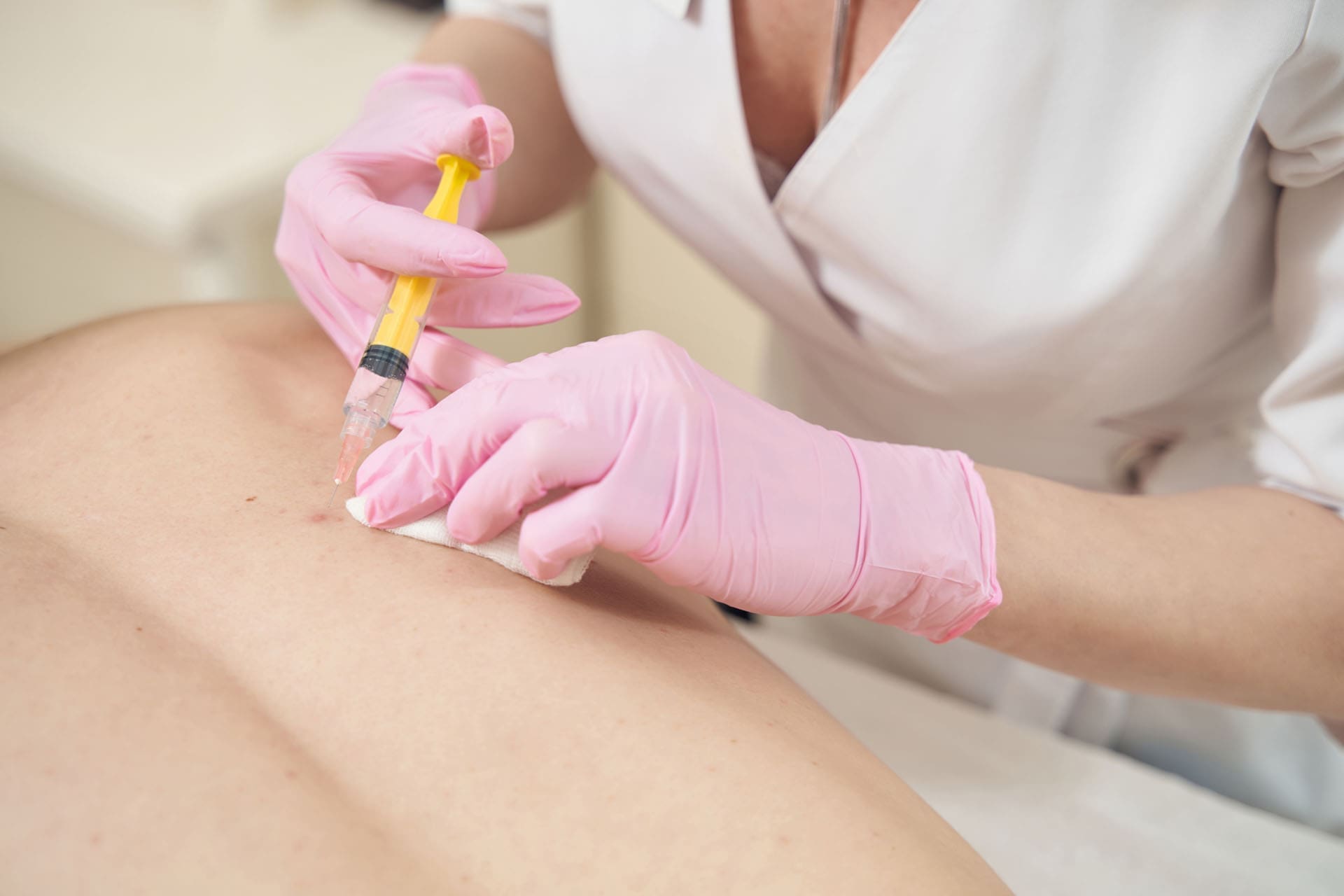
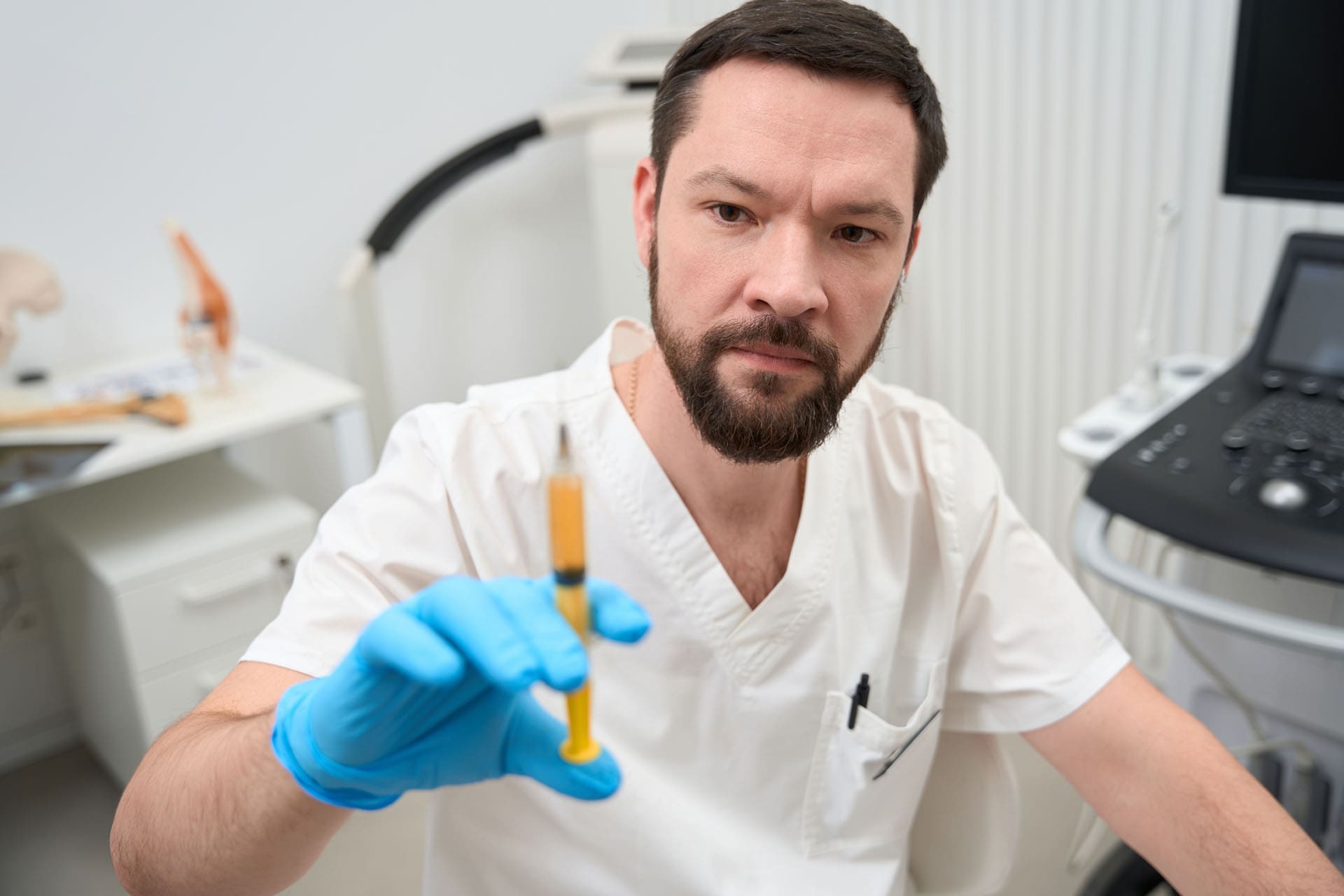
PRP stands for platelet-rich plasma. The team at ChiroMed starts with a simple blood draw from your arm. They place the blood in a special machine called a centrifuge, which spins it rapidly to concentrate the platelets. These platelets carry powerful growth factors that signal the body to repair itself. Doctors then inject this golden PRP liquid exactly where the spine needs help. (ChiroMed, n.d.-b)
At ChiroMed, PRP goes beyond basic shots. The clinic blends regenerative medicine with chiropractic adjustments and functional medicine testing. This whole-person method sets ChiroMed apart from clinics that only treat symptoms. Because the PRP comes from your body, the chance of bad reactions is very low. (Jimenez, n.d.)
How PRP Supports Healing in the Spine
Your spine works hard every day. Discs cushion the bones, facet joints let you twist and bend, and ligaments hold everything steady. Over time, wear, injury, or aging can damage these parts and cause pain.
- PRP delivers growth factors directly to damaged discs, so new cells can grow and the cushioning improves.
- For inflamed facet joints, the injection calms swelling and helps restore smooth motion.
- In stretched ligaments and tendons around the spine, PRP speeds repair and restores stability.
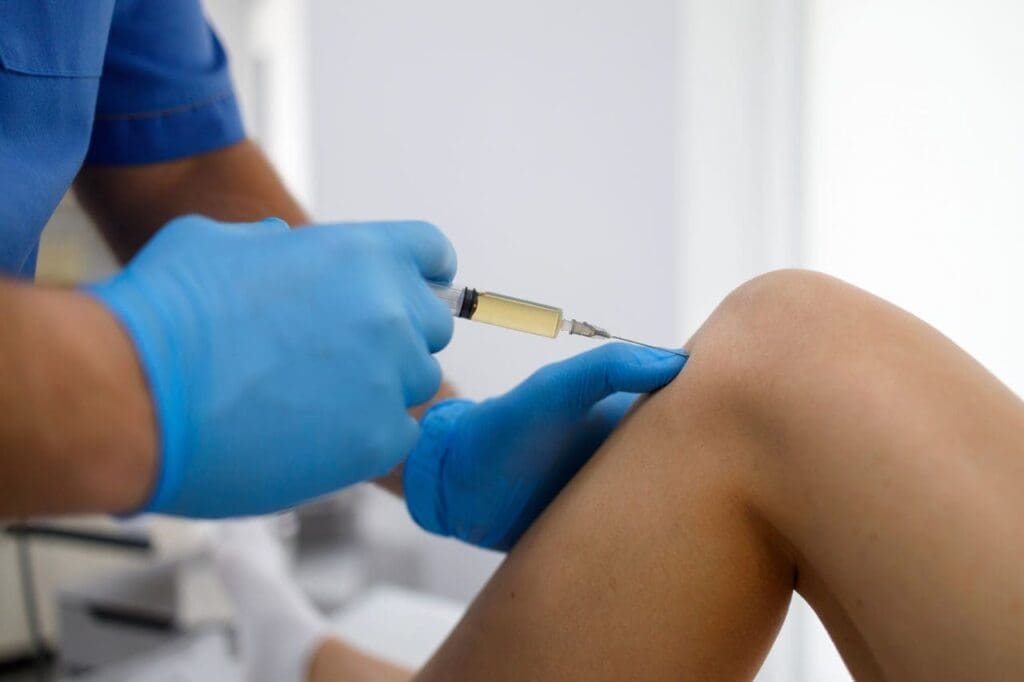
ChiroMed uses ultrasound guidance for every injection to ensure it hits the exact spot. This precision means better results and less discomfort. One review of studies shows PRP also aids nerve repair, which matters when spinal issues press on nerves and send pain down the legs. (Wang et al., 2024)
Key Benefits of PRP Therapy at ChiroMed
Patients at ChiroMed choose PRP because it offers real, lasting relief without major operations. Here are the top advantages they notice:
- Natural pain relief: PRP lowers inflammation right at the source instead of masking it with pills or steroids.
- Improved daily movement: Many regain the ability to walk, bend, and lift with less effort after a few weeks.
- Quick return to normal life: Most people resume light activities within one or two days, much faster than after surgery.
- Longer results: Relief often lasts six months to a year or more, unlike short-term steroid shots.
- Minimal risk: No foreign drugs enter the body, so side effects are rare.
- Tissue rebuilding: PRP helps regenerate new cartilage and strengthen soft tissues, keeping the spine strong. (ChiroMed, n.d.-a; Florida Pain Management Institute, 2025)
Dr. Alexander Jimenez, DC, APRN, FNP-BC, who leads ChiroMed, has over 30 years of experience. His clinical observations show that patients who combine PRP with chiropractic care see faster mobility gains and fewer pain flare-ups. (Jimenez, n.d.; ChiroMed, n.d.-a)
Who Can Benefit from PRP at ChiroMed?
PRP works well for adults facing stubborn spinal issues. Good candidates at ChiroMed often include those with:
- Degenerative disc disease
- Spinal stenosis that squeezes nerves
- Facet joint arthritis
- Herniated or bulging discs
- Chronic low back or neck pain that did not improve with rest or exercises
If physical therapy, ice, or over-the-counter medicine have not helped enough, the team at ChiroMed evaluates you for PRP. They check your full health history first. Most patients qualify, but those with active infections or certain blood conditions may need different plans. The clinic’s integrative approach makes PRP safer and more effective for a wide range of people. (Total Spine Institute, n.d.; Greater Austin Pain Center, 2025)
How Dr. Alexander Jimenez Powers Up PRP Therapy
An Advanced Practice Registered Nurse (APRN/FNP-BC) with functional medicine training (CFMP, IFMCP, ATN, CCST) can enhance PRP therapy by using precise, ultrasound-guided injections, along with structural alignment and nutritional support, to accelerate healing. At ChiroMed, Dr. Alexander Jimenez, DC, APRN, FNP-BC, CFMP, IFMCP, ATN, CCST, brings exactly this dual expertise to every patient.
Dr. Jimenez holds chiropractic and family nurse practitioner licenses across multiple states. His 30-plus years of practice focus on addressing root causes rather than merely covering symptoms. At the ChiroMed clinic at 11860 Vista Del Sol Dr, Suite 128, in El Paso, he pairs PRP injections with gentle chiropractic adjustments to keep the spine aligned. He also orders functional medicine tests that check nutrition, hormones, and hidden inflammation. His clinical observations reveal that patients heal more quickly and remain pain-free longer when PRP is combined with dietary changes and metabolic support. (ChiroMed, n.d.-b; Injury Medical & Chiropractic Clinic, n.d.)
The Power of Combining Regenerative, Functional, and Structural Care at ChiroMed
When you combine regenerative medicine (PRP), functional medicine (metabolic/nutritional support), and structural care (chiropractic), you have a very effective way to restore your spine. ChiroMed built its entire practice around this trio.
- Regenerative step: PRP injections jump-start repair exactly where damage exists in discs, joints, or ligaments.
- Functional step: Blood work guides custom supplements and food plans that lower body-wide inflammation and feed healing cells.
- Structural step: Chiropractic adjustments keep bones aligned so that new tissue forms correctly and nerves remain free of pressure.
Dr. Jimenez often sees patients at ChiroMed return to work or their favorite activities sooner with this team method. They report less need for pain pills and more confidence moving through daily life. The clinic also offers acupuncture, naturopathy, and IV nutrition to further support PRP. (Personal Injury Doctor Group, 2026; ChiroMed, n.d.-c)
What to Expect During and After PRP Treatment at ChiroMed
Your visit to ChiroMed usually takes under an hour. A friendly staff member draws a small tube of blood. While the centrifuge works, you relax in a comfortable room. Dr. Jimenez or a trained team member then uses real-time ultrasound to guide the thin needle to the precise site of the problem. Local numbing keeps discomfort low.
Afterward, you may feel mild soreness for a day or two, like after a tough workout. The staff encourages light walking but asks you to avoid heavy lifting for one to two weeks. Improvements often begin in four to six weeks as growth factors rebuild tissue. Some patients need two or three sessions spaced a few weeks apart for the best outcome. (CalSpine MD, n.d.; PRP Labs, n.d.)
ChiroMed follows up closely. They track your progress with movement tests and adjust nutrition or alignment care as needed. This personal attention helps results last.
Evidence Behind PRP for Spinal Problems
Research supports PRP’s role in spine care. Clinical reviews show it cuts pain and boosts function in degenerative disc disease and facet joint problems. One analysis found PRP helps nerve repair by calming inflammation and growing new cells. While larger studies continue, clinics like ChiroMed report strong real-world success with sciatica and back pain. (Wang et al., 2024; Ohio State Wexner Medical Center, n.d.)
Patients love that PRP uses their body to heal. It matches the natural, drug-free lifestyle many people at ChiroMed seek.
Moving Forward with Spine Health at ChiroMed
PRP therapy offers fresh hope for anyone tired of living with constant back pain. By tapping into your blood’s own healing power, it reduces swelling, rebuilds tissue, and restores movement. At ChiroMed Integrated Medicine in El Paso, Dr. Alexander Jimenez and his team blend PRP with chiropractic and functional medicine for results that last.
If conservative care has not brought enough relief, reach out to ChiroMed. Their integrated approach may help you enjoy a stronger, pain-free back again. Call (915) 412-6680 or visit https://chiromed.com/ to learn more about PRP for spinal care.
References
CalSpine MD. (n.d.). PRP therapy for back & spine problems.
ChiroMed. (n.d.-a). Platelet-rich plasma (PRP) therapy for sciatica.
ChiroMed. (n.d.-b). Platelet-rich plasma therapy supports detoxification.
ChiroMed. (n.d.-c). PRP therapy for sports injuries: Non-surgical healing.
Florida Pain Management Institute. (2025, May 6). 5 reasons to consider PRP therapy for spine repair.
Greater Austin Pain Center. (2025, October 31). PRP injections for joint and spine pain: What you need to know.
Injury Medical & Chiropractic Clinic. (n.d.). Alex Jimenez DC, APRN, FNP-BC, CFMP, IFMCP.
Jimenez, A. (n.d.). Injury specialists.
Miami Spine and Sports Doctor. (n.d.). PRP therapy for the spine: 6 benefits and 5 conditions it can treat.
Morrison Clinic. (n.d.). Platelet-rich plasma therapy for spine.
Ohio State Wexner Medical Center. (n.d.). The benefits of using platelet-rich plasma therapy to treat back pain.
Personal Injury Doctor Group. (2026, March 16). Revitalizing recovery: How PRP therapy works.
PRP Labs. (n.d.). How PRP therapy may relieve spinal stenosis symptoms.
Total Spine Institute. (n.d.). Platelet-rich plasma treatments.
Wang, S., Liu, Z., Wang, J., Cheng, L., Hu, J., & Tang, J. (2024). Platelet-rich plasma (PRP) in nerve repair. Regenerative Therapy, 27, 244–250. https://doi.org/10.1016/j.reth.2024.03.017