Pigeon Toed: Causes and Treatment Options
Children walking with their toes pointed in may be pigeon-toed. What are the causes, conditions associated with it, and treatments?

Pigeon-toed Walking
If a child walks with their feet turned inward at the toes, it is usually described as being pigeon-toed. This pointing inward of the feet occasionally occurs as a child learns to walk and may continue through toddlerhood. It is noticed more often in children than adults, but older individuals can experience it. Pigeon-toed walking is rarely a major orthopedic problem and usually disappears without treatment. However, there are times when it may impact a child’s lower extremities and hips. Bracing or surgery may be necessary in these cases to correct the problem. (Paramanandam V. et al., 2019) This condition is common and typically is caused by abnormal birth positions in utero. Sometimes, slight issues may lead to noticeable functional characteristics. Mild changes in bone shape and positioning usually cause pigeon toes. Often, it subsides in a few years as the child continues to develop.
What Does It Mean?
There is usually no need to worry, as this condition is likely not permanent and will go away in a few years. (Paramanandam V. et al., 2019) However, it is recommended that you check in with your healthcare provider to ensure the child is developing normally. Some adults walk with their toes turned in. This may be due to a birth defect, a weakness, or a rare case of pigeon-toed walking as a youth that was left untreated or did not go away.
Causes
There are various reasons for pigeon-toed walking. To determine the cause, a healthcare provider can assess the child’s condition and make a diagnosis, including:
Metatarsus Adductus
- A condition where the front part of the foot is turned inward.
- The metatarsals are the long bones of the forefoot.
- This is when the bones of the foot point inward, leading to pigeon-toed walking.
- A clinical examination and X-ray can confirm the metatarsus adducts as a cause of pigeon-toed walking.
Tibial Torsion
- A twisted shinbone (tibia) can cause the feet to turn inward in younger children.
- The shinbone/tibia in some children may be slightly twisted.
- The tibia can either turn outward or inward.
- When it twists inward, it may manifest as a pigeon-toed gait.
- Tibial torsion may accompany femoral anteversion.
- It is diagnosed with an X-ray.
- Children with tibial torsion typically grow out of the problem, and the pigeon-toed disappears by age 4. (Uden H., & Kumar S. 2012)
Femoral Anteversion
- A common cause, especially in older children, is when the thighbone/femur is twisted inward.
- If the femur turns inward and forward unnaturally, where the femoral neck meets the body of the femur, it is called femoral anteversion.
- An outward and backward rotation of the femur is called femoral retroversion.
- This occurs in about 10% of children. (Scorcelletti M. et al., 2020)
- Many children with femoral anteversion appear knock-kneed with a large gap between their feet when standing with knees together, and when they walk, they appear pigeon-toed.
- A clinical examination and X-ray diagnose it.
Symptoms
In most cases, the child does not complain of any pain. However, if pain is felt, it can include:
- Tightness in the calf muscles
- Aching on the outer edges of the feet
- Knee pain
Usually, parents will notice pigeon-toes when their child is first learning to walk. Rest assured, the child most likely is not experiencing pain. They have feet and knees that turn inward when they walk and run. (Uden H., & Kumar S., 2012)
A pediatrician or primary care provider can assess the situation and make recommendations. Most pigeon-toed children begin walking and running normally after age 3 or 4, so a watch-and-wait approach is used. Parents may have to take their child to a specialist, like an orthopedic surgeon, if they complain of pain while walking. A specialist may be referred if the child cannot walk due to the inward turn of their feet.
Risk Factors
Pigeon-toed walking is not a preventable condition but rather one that develops during pregnancy. Causes may include: (Scorcelletti M. et al., 2020)
- A pregnancy with twins or multiple births
- Large fetus
- Breech position in utero when the baby is positioned feet first.
- Not enough amniotic fluid
Muscle Weakness in Adults
Adolescents or adults who notice their knees turn in and walk pigeon-toed may have weakness in the hip and leg muscles that control the position of their legs when they walk. Strengthening those muscles can help. (Scorcelletti M. et al., 2020)
Treatment
Typically, a normal gait will appear by the age of 3 or 4. Other treatments may include:
Physical Therapy Exercises and Gait Training
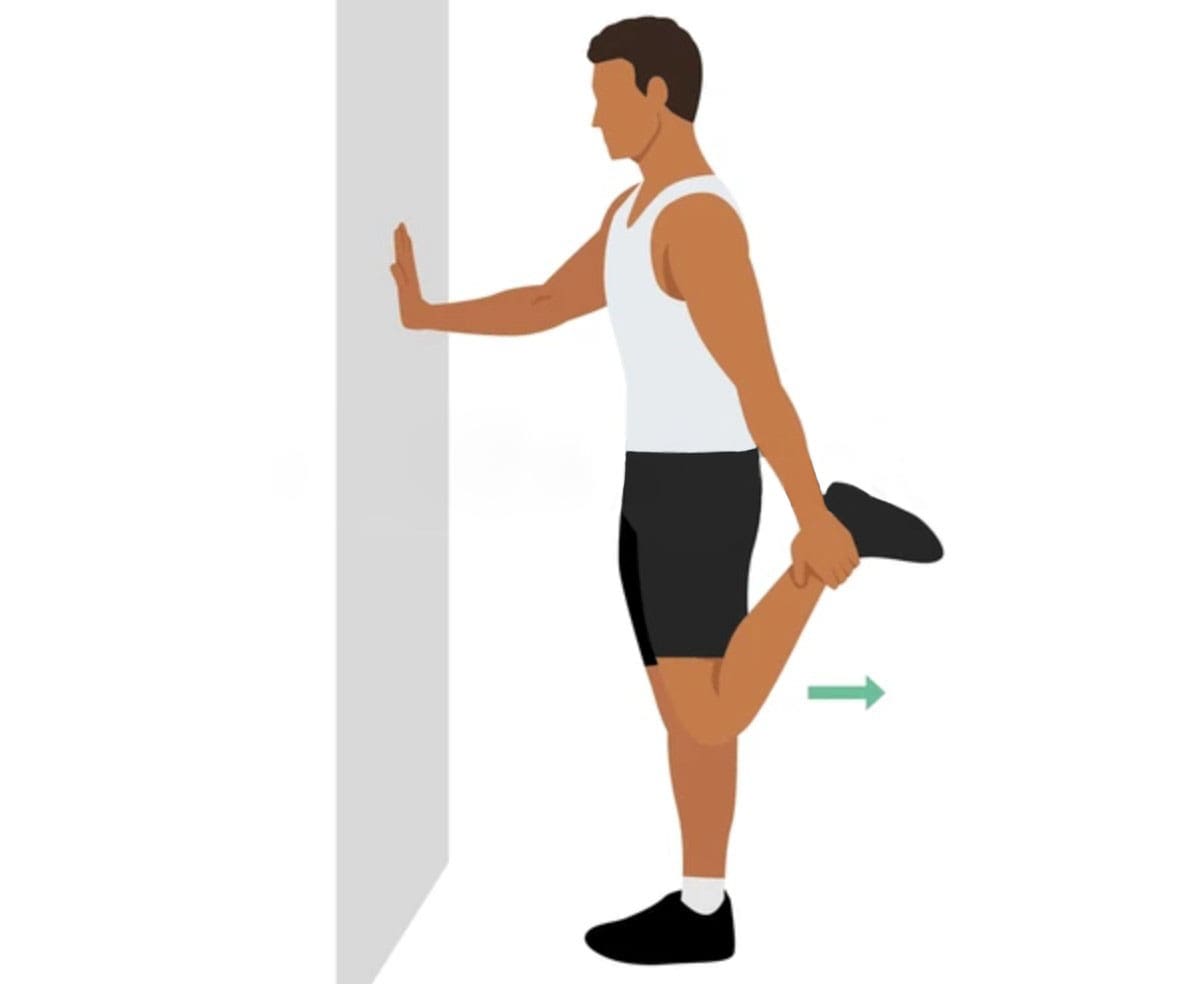
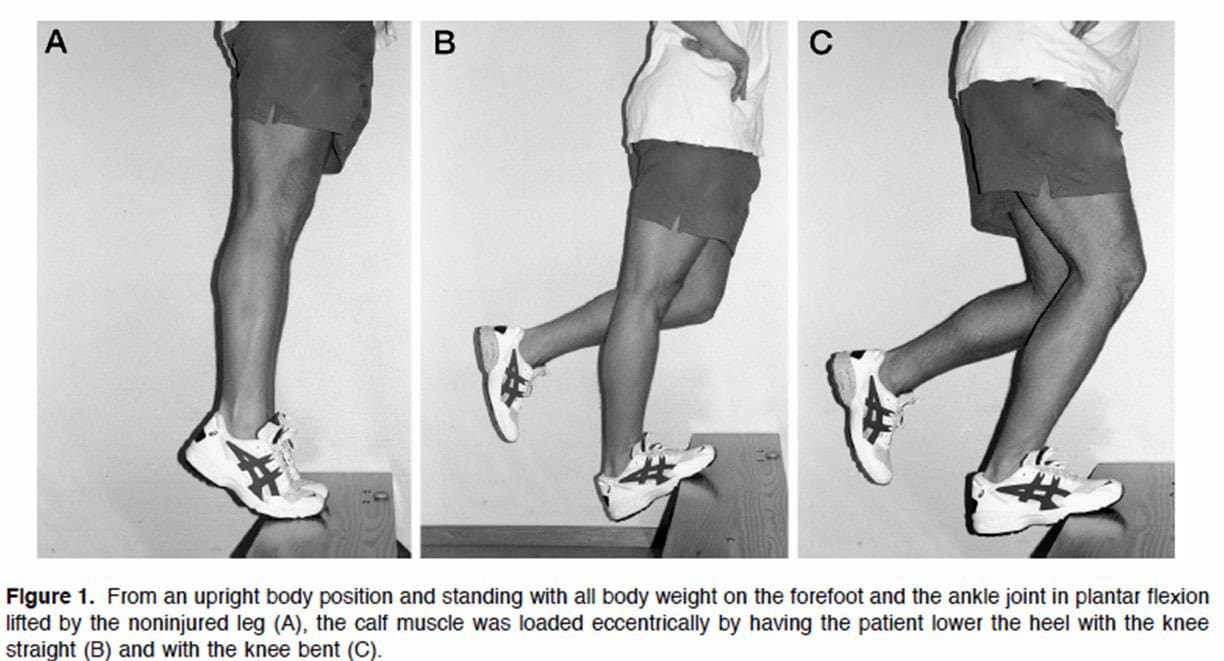
- Exercises to stretch tight lower extremity muscles and strengthen hip and leg muscles can help improve walking gait.
- See a pediatric specialist before starting, as research shows that parental stretching of a newborn with metatarsus adductus offers little benefit. (Eamsobhana P. et al., 2017)
Bracing or Casting
- Braces
- Serial casting is a procedure that helps children improve their range of movement and may be done to place their lower extremities in an optimum position as they develop. (Uden H., & Kumar S., 2012)
Surgery
- For cases in which tibial torsion is the cause, osteotomy surgery, which involves cutting and/or removing bone, may be recommended to correct the structural deformity of the shinbone.
Injury Medical Chiropractic & Functional Medicine Clinic
Injury Medical Chiropractic and Functional Medicine Clinic works with primary healthcare providers and specialists to develop an optimal health and wellness solution. We focus on what works for you to relieve pain, restore function, and prevent injury. Regarding musculoskeletal pain, specialists like chiropractors, acupuncturists, and massage therapists can help mitigate the pain through spinal adjustments that help the body realign itself. They can also work with other medical professionals to integrate a treatment plan to resolve musculoskeletal issues.
Foot Pronation
References
Paramanandam, V., Lizarraga, K. J., Soh, D., Algarni, M., Rohani, M., & Fasano, A. (2019). Unusual gait disorders: a phenomenological approach and classification. Expert review of neurotherapeutics, 19(2), 119–132. https://doi.org/10.1080/14737175.2019.1562337
Uden, H., & Kumar, S. (2012). Non-surgical management of a pediatric “intoed” gait pattern – a systematic review of the current best evidence. Journal of Multidisciplinary Healthcare, 5, 27–35. https://doi.org/10.2147/JMDH.S28669
Scorcelletti, M., Reeves, N. D., Rittweger, J., & Ireland, A. (2020). Femoral anteversion: significance and measurement. Journal of Anatomy, 237(5), 811–826. https://doi.org/10.1111/joa.13249
Eamsobhana, P., Rojjananukulpong, K., Ariyawatkul, T., Chotigavanichaya, C., & Kaewpornsawan, K. (2017). Does the parental stretching programs improve metatarsus adductus in newborns?. Journal of Orthopaedic Surgery (Hong Kong), 25(1), 2309499017690320. https://doi.org/10.1177/2309499017690320