BHRT: What to Expect With Hormones & Pellet Therapy
Understand the impact of BHRT and pellet therapy on your hormonal health and how they can improve your quality of life.
Abstract
Hello, I’m Dr. Alexander Jimenez. Welcome to this educational exploration of hormone health and integrative care. In my practice, which combines chiropractic care with advanced functional and integrative medicine, I have seen firsthand the profound impact hormonal balance has on overall health. This post is designed to guide you through the sophisticated, evidence-based approaches we use to manage hormonal imbalances, particularly those associated with perimenopause, menopause, and andropause. We will begin by outlining the streamlined patient journey in our clinic, from initial contact to follow-up care, highlighting the use of modern tools, such as QR code campaigns, to enhance patient education. Following this, we will dive into detailed case studies of both a female and a male patient. Through these real-world examples, I will break down the interpretation of comprehensive lab work, discussing key biomarkers like ferritin, thyroid-stimulating hormone (TSH), free testosterone, and Estradiol. We’ll explore the physiological significance of these markers and how they inform our treatment decisions, including the use of Bioidentical Hormone Replacement Pellet Therapy (BHRT). I will also detail the precision of the pellet insertion procedure itself and discuss the critical role of integrative chiropractic care in addressing the musculoskeletal and neurological symptoms that often accompany hormonal shifts. Our goal is to present a holistic, patient-centered model that combines cutting-edge research with personalized clinical care to optimize health and well-being.
Revolutionizing the Patient Experience: A Streamlined Clinical Workflow
Over my years in practice, I’ve observed a significant paradigm shift in how we approach patient care, especially in the realm of hormonal health. The journey to wellness must be clear, efficient, and supportive. I want to walk you through the workflow we have refined in our clinics, which serves as a roadmap for both our patients and our providers.
Our process begins the moment a potential patient expresses interest.
- Initial Contact and Lab Initiation: When someone calls our office, we schedule them for an initial provider consultation. Critically, we don’t wait for that first appointment to start gathering information. We immediately initiate a comprehensive lab panel tailored to their likely needs. This proactive step ensures that when I first sit down with a patient, we have objective data to guide our conversation.
- Empowering Through Education: The QR Code Campaign: About 13 years ago, working with a business coach, I had a realization: we were repeating the same foundational information to every new patient. While necessary, it consumed valuable consultation time that could be better spent on a personalized strategy. This led to the creation of our QR code educational campaigns. Before their first visit, patients receive access to a series of short, digestible videos. These videos answer common questions about hormone therapy, explain the process, and demystify the science. By the time they come in to review their labs, they are already educated and empowered, allowing us to have a much deeper and more productive conversation.
- The Comprehensive Consultation: During the consultation, we review several key items together:
- Symptom Checklists: We use validated tools such as the Menopausal Rating Scale (MRS) and our Bioidentical Hormone Replacement Therapy (BHRT) symptom checklist.
- Lab Results: We conduct a thorough, line-by-line review of their comprehensive lab work.
- Treatment Options: We discuss all available treatment modalities. In our office, this includes pellets, injections, and creams. We present the pros and cons of each, allowing the patient to make an informed choice that aligns with their lifestyle and preferences.
Once a treatment plan is decided upon, we schedule the procedure. Before they leave, we also schedule their follow-up lab work. In the early days, we used to tell patients to come back when they “felt” their symptoms returning. This was a mistake. The decline is often so gradual that patients don’t recognize it until they feel significantly unwell again, leading to poor retention and inconsistent results. Now, we pre-schedule follow-up labs—typically at 14 weeks for women and 18 weeks for men—to stay ahead of the curve and maintain optimal levels. This proactive approach is key to long-term success.
The Critical Role of Informed Consent and Patient Education
In medicine, documentation is paramount. The informed consent process is not merely a legal formality to protect the practitioner; it is a cornerstone of ethical care that justifies and explains the entire treatment plan. Our consent forms are comprehensive educational documents. They explicitly detail why we believe in BHRT and reference the scientific literature supporting its use. We are transparent about the off-label nature of custom-compounded hormone pellets. While the hormones themselves (testosterone, estradiol) are FDA-approved, their use in the form of compounded pellets for indications such as improving well-being and mitigating age-related symptoms is considered off-label.
The consent form explains the rationale for using pellets, the specific labs and diagnostic criteria used, potential side effects, and the critical importance of adherence. By having the patient read and sign this detailed document, we ensure they can never say, “I was never told.” This level of transparency builds trust and protects both the patient and the provider.
Case Study 1: Decoding Menopausal Symptoms in a 59-Year-Old Female
Let’s delve into a representative case to see how this process plays out. This patient is a 59-year-old female presenting with common complaints associated with post-menopause.
Her Menopausal Rating Scale (MRS) reveals a significant symptom burden. The scale, which is numerically scored, shows she is experiencing severe symptoms, particularly in the realms of mood (depressive symptoms) and sexual health (diminished desire). Her score is far from the ideal post-treatment goal. This subjective data is our starting point; it’s the patient’s lived experience.
Comprehensive Lab Analysis: Uncovering the Root Causes
Next, we turn to her objective lab data. A full understanding requires looking beyond just the sex hormones.
- Ferritin: Her ferritin level is a point of concern. Ferritin is the body’s primary iron storage protein. A low ferritin level, even if hemoglobin and hematocrit are normal, can mimic and exacerbate symptoms of hormonal imbalance, such as fatigue, hair loss, and brain fog. Before initiating hormone therapy, it is crucial to optimize iron stores. In her case, I would recommend a daily dose of a high-quality iron supplement.
- Vitamin D: Her Vitamin D level is also suboptimal. Vitamin D, a pro-hormone, is essential for immune function, bone health, and mood regulation. Research, such as that highlighted by Holick (2007), underscores its systemic importance. For a patient like this, I would typically start with a dose of 5,000 IU daily to bring her levels into the optimal range, which can also help mitigate inflammatory processes.
- Thyroid Panel:
- Her Thyroid-Stimulating Hormone (TSH) is 3.8 mIU/L. While this may fall within a “normal” lab reference range, the functional and anti-aging medicine communities, supported by a growing body of literature, advocate for a much narrower optimal range, typically below 2.5 mIU/L (Jabbar et al., 2021). A TSH of 3.8 suggests her thyroid is working too hard, a sign of subclinical hypothyroidism.
- Her Free T3 is suboptimal. T3 is the active thyroid hormone that drives metabolism in every cell of the body.
- Her Free T4 is 0.8 ng/dL. This is also on the low end of the optimal range.
My immediate thought is that her thyroid is sluggish. The brain’s pituitary gland is releasing more TSH to “yell” at the thyroid, which is under-responding. This is a classic feedback loop issue that contributes significantly to her fatigue, weight gain, and depressive mood.
- Sex Hormones:
- Her Free Testosterone is functionally zero. This is a critical finding. While often considered a “male” hormone, testosterone is vital for women’s energy, mood, cognitive function, muscle mass, and libido. A level this low is a primary driver of her symptoms.
- Her Estradiol is 18 pg/mL. For a post-menopausal woman, this isn’t dangerously low, but it’s far from optimal for symptom relief and protection against bone loss and cognitive decline. Research by Santoro, Roeca, and Peters (2021) clearly outlines the systemic effects of estrogen decline. The brain is literally starving for these hormones.
The Treatment Plan: BHRT and Integrative Chiropractic Care
Based on these findings, this patient is a clear candidate for Bioidentical Hormone Replacement Pellet Therapy (BHRT). My goal is to restore estradiol and testosterone to levels reminiscent of her pre-menopausal state, where she felt her best. This is not about achieving supra-physiological levels but about restoring physiological balance.
This is also where integrative chiropractic care becomes essential. Hormonal decline, particularly the loss of estrogen and testosterone, directly impacts musculoskeletal integrity.
- Musculoskeletal Support: Patients often report new aches, joint stiffness, and a sense of physical fragility. The “meno-belly” she describes—a sudden accumulation of visceral fat around the midsection despite no changes in diet or exercise—is a classic sign of hormonal shift, driven by cortisol and insulin dysregulation secondary to low estrogen. Chiropractic adjustments help restore proper joint mobility and alleviate pain. We also incorporate specific soft tissue therapies to address muscle tension and fascial restrictions that develop.
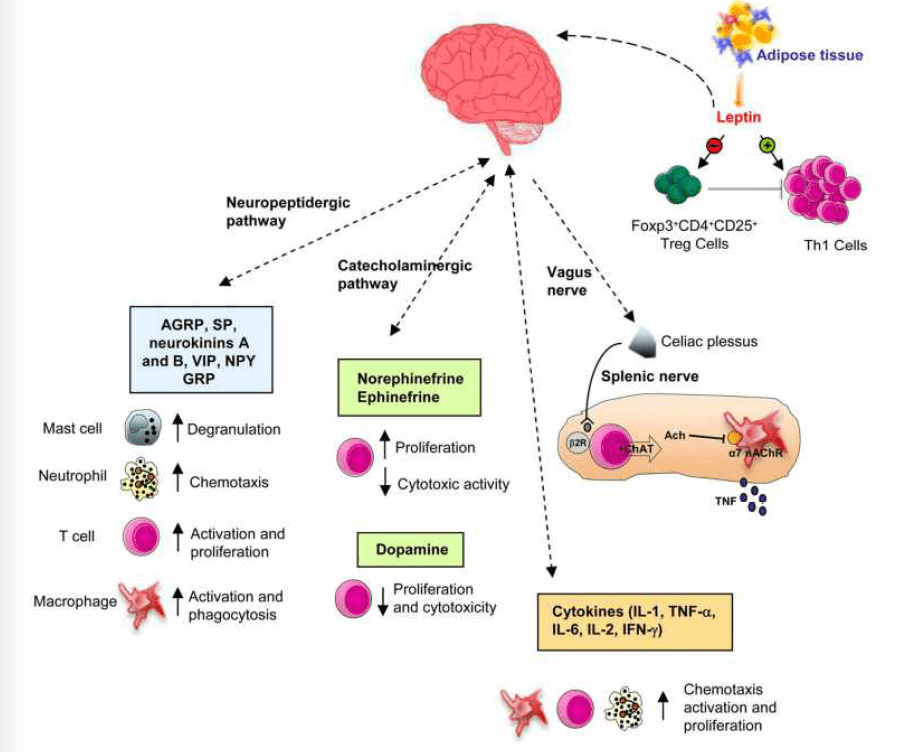
- Neurological Regulation: The nervous system and endocrine system are intricately linked. Spinal misalignments can interfere with the signaling of the hypothalamic-pituitary-adrenal (HPA) axis, which governs our stress response and hormone production. By performing targeted chiropractic adjustments, we can help normalize neurological feedback loops, reduce sympathetic (fight-or-flight) overdrive, and support the body’s overall ability to adapt and heal. This is particularly important for managing the anxiety and sleep disturbances that accompany menopause.
For this patient, the plan is multifaceted: initiate BHRT to address foundational hormonal deficiencies; supplement to correct her vitamin D and ferritin levels; provide nutritional guidance to support her thyroid and manage inflammation; and implement regular chiropractic care to address the structural and neurological consequences of her hormonal state.
Assessing Hormone Therapy- Video
Case Study 2: Addressing Andropause in a Male Patient
Now, let’s consider a male patient presenting with symptoms of andropause, the male equivalent of menopause. He reports a classic constellation of symptoms on the Aging Male Symptoms (AMS) scale: low libido, decreased stamina, loss of morning erections, increased visceral fat (a “pot belly”), and general GI issues.
Interpreting the Male Lab Panel
His lab work paints a stark picture of metabolic and hormonal decline.
- Kidney Function: His elevated creatinine is an immediate flag for impaired kidney function. My first step is to educate him on this finding and ensure he follows up with his primary care provider or a nephrologist. We must work collaboratively and ensure all aspects of a patient’s health are monitored.
- Bone Density: He has signs of osteopenia. I would educate him about the importance of a DEXA scan to get a precise measure of his bone mineral density. Testosterone is crucial for maintaining bone health in men, and its decline is a major risk factor for osteoporosis (Mohamad et al., 2016).
- Metabolic Markers:
- His Hemoglobin A1c indicates prediabetes.
- His C-Reactive Protein (CRP), a marker of systemic inflammation, is elevated.
- He has hypertension and high cholesterol.
- Sex Hormones:
- His Total Testosterone is 122 ng/dL. This is profoundly low. Optimal levels for a man should be in the 700-900 ng/dL range. A level of 122 is not just a quality-of-life issue; it is a medical issue that drives his metabolic disease. Low testosterone is directly linked to an increased risk of diabetes, heart disease, and cognitive decline.
- His Sex Hormone-Binding Globulin (SHBG) is very low. SHBG is a protein that binds to testosterone, making it unavailable to the tissues. While a low SHBG might seem good because it means more “free” testosterone is theoretically available, in the context of his overall metabolic dysfunction, it’s another sign of insulin resistance and inflammation.
The Comprehensive Treatment Protocol for Andropause
This patient is a prime candidate for Testosterone Pellet Therapy. Restoring his testosterone to an optimal physiological range is the single most effective intervention to address the root cause of his myriad symptoms. As with our female patient, integrative chiropractic care is a cornerstone of his treatment. Low testosterone is associated with sarcopenia (age-related muscle loss) and joint pain.
- Biomechanical Optimization: We use chiropractic adjustments to ensure his spine and extremities are functioning optimally, providing a stable foundation for the renewed exercise and physical activity that testosterone therapy will enable.
- Pain Management: We address the chronic aches and pains that have likely made him more sedentary, creating a vicious cycle of inactivity and further decline.
- Lifestyle Coaching: As part of our integrative model, we provide targeted advice on resistance training and nutrition to maximize the benefits of his hormone therapy, helping him rebuild muscle, lose fat, and reclaim his vitality.
By combining cutting-edge BHRT with foundational chiropractic care and lifestyle medicine, we can dramatically alter the trajectory of his health, moving him from a state of metabolic disease and low vitality to one of optimal function and well-being.
The Art and Science of Pellet Insertion Technique
The physical procedure of pellet insertion has evolved significantly. The technique used is just as important as the dosage itself, as it directly impacts hormone absorption, efficacy, and patient comfort. We have moved far beyond outdated methods that caused unnecessary trauma and inconsistent results. Today, we use a much more elegant and effective no-scalpel, micro-tunneling technique that prioritizes precision and minimizes tissue trauma.
- Preparation and Anesthesia: After preparing a sterile field, we use a two-step numbing process to anesthetize the deep fatty layer of the upper gluteal region, well above the muscle.
- The Incision and Trocar: A tiny incision is made parallel to Langer’s lines (natural skin tension lines) to promote better healing and minimize scarring. We then use a specialized blunt-tipped instrument called a trocar to gently separate the fatty tissue and create small, separate tunnels or “tracks”. This avoids cutting through tissue, which reduces trauma and bleeding.
- Layered Pellet Placement: We carefully lay the pellets down in these individual tracks, fanning them out like the spokes of a wheel. This technique is revolutionary because it maximizes the surface area for neovascularization—the formation of new blood vessels. These tiny capillaries grow around each pellet, creating a rich vascular network that ensures slow, steady, and consistent hormone absorption over several months.
- Bandaging for Optimal Healing: We close the small incision with Steri-Strips to approximate the wound edges, then apply a multi-layered dressing. This includes a sterile gauze pad, a protective “T” formation with medical tape to prevent accidental removal, and a final waterproof bandage. This meticulous process is designed to promote rapid healing and prevent complications.
Proper post-procedural care, including keeping the area dry and avoiding strenuous activity for several days, is essential to prevent infection and ensure the best possible outcome.
Follow-Up and Long-Term Management: The Art of Titration
Hormone therapy is a dynamic process, not a one-size-fits-all-for-life solution. The goal of the first round of pellets is to fill the patient’s “empty tank.” Subsequent rounds are about maintenance and fine-tuning. After about four to six weeks, we re-check labs. I often see cases where a patient feels “amazing,” but their lab values haven’t reached our definition of the optimal range. This tells me we can further optimize their dose for even better, longer-lasting results.
Conversely, a patient will not require the same large initial dose for their second round. Continuing to give the same high dose would eventually lead to symptoms of excess. This is where clinical acumen comes into play. We must listen to the patient’s subjective experience and titrate their dose based on a combination of their symptoms and lab values. This is a partnership. By managing expectations and adjusting the course as needed, we can guide our patients toward vibrant health and a dramatically improved quality of life.
References
- Guo, S., & DiPietro, L. A. (2010). Factors affecting wound healing. Journal of Dental Research, 89(3), 219–229.
- Holick, M. F. (2007). Vitamin D deficiency. New England Journal of Medicine, 357(3), 266–281.
- Jabbar, A., Ingoe, L., Pearce, S., Zaman, A., & Razvi, S. (2021). Thyroxine treatment for subclinical hypothyroidism: a clinical practice guideline. European Thyroid Journal, 10(2), 152–162.
- Mohamad, N. V., Soelaiman, I. N., & Chin, K. Y. (2016). A concise review of testosterone and bone health. Clinical Interventions in Aging, 11, 1317–1324.
- Santoro, N., Roeca, C., & Peters, B. A. (2021). The menopause transition: Signs, symptoms, and management options. The Journal of Clinical Endocrinology & Metabolism, 106(1), 1–15.
- Schaffer, C. J., Nanney, L. B., & Stecenko, A. A. W. H. (2016). Wound healing. In Fitzpatrick’s Dermatology in General Medicine (9th ed.). McGraw-Hill.
- Yoo, J. Y., Groer, M., Dutra, S. V. O., & Sarkar, A. (2020). Gut microbiota and immune system interactions. Microorganisms, 8(10), 1587.
SEO Tags: Hormone Replacement Therapy, BHRT, Bioidentical Hormones, Menopause, Andropause, Integrative Chiropractic Care, Functional Medicine, Testosterone, Estradiol, Thyroid Health, Dr. Alex Jimenez, Pellet Therapy, Subclinical Hypothyroidism, Ferritin, Vitamin D, Patient Education, Clinical Workflow, Case Study, Pellet Insertion, Wound Healing, Langer’s Lines, Trocar Technique, Musculoskeletal Health, Inflammation, El Paso Chiropractor