Paraspinal Muscle Tension: Understanding the Impacts
Can a paraspinal muscle spasm in the lower back create a chain reaction leading to hamstring spasms and potential sciatic nerve entrapment?

Paraspinal Muscle Spasm Chain Reaction
A paraspinal muscle spasm in the lower back can cause a cascade of events, including: (Cedars-Sinai, 2025)
- Spasms in other lower back muscles
- Hamstring spasms
- Potential entrapment of the sciatic nerve
Leading to symptoms similar to sciatica:
- Pain
- Sore, achy muscles
- Weak muscles
- Numbness
- Tingling along the back of the leg
Possible Mechanisms
Triggering Muscle Spasms in the Lower Back
- Paraspinal muscles are located along the spine and help to stabilize and support the lower back.
- When these muscles spasm, they can become tense and painful, causing a chain reaction.
- This tension can radiate down and affect other muscles in the lower back. (Noonan A. M., & Brown S. H. M., 2021)
Can Affect Lower Back Muscles and Cause Hamstring Spasms
- Lower back muscles, including those like the quadratus lumborum, can be affected by paraspinal spasms. (Hospital for Special Surgery, 2024)
- The spasms can cause these muscles to tighten or spasm, potentially pulling on the hamstring muscles.
- This can lead to hamstring spasms and tightness, further contributing to pain and potential nerve irritation.
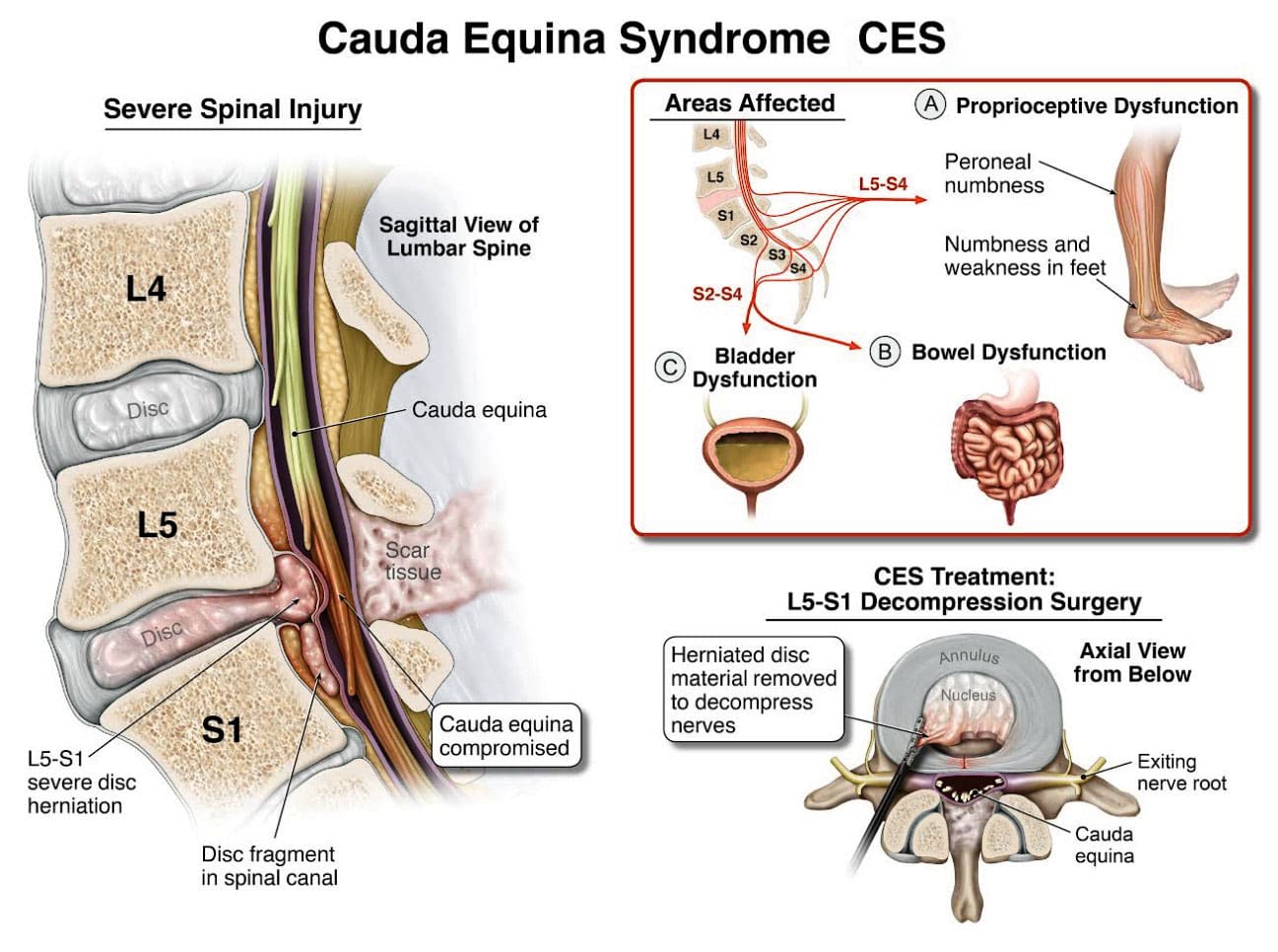
Entrapment of the Sciatic Nerve
- Piriformis syndrome is a common condition where the piriformis muscle (located in the buttock) spasms and compresses the sciatic nerve. (Cedars-Sinai, 2025)
- The sciatic nerve runs from the lower back down the back of the thigh and into the leg, making it vulnerable to compression by surrounding muscles.
- If the paraspinal and hamstring spasms create enough tension on the piriformis muscle or surrounding tissues, it can lead to sciatic nerve entrapment. (Hospital for Special Surgery, 2024)
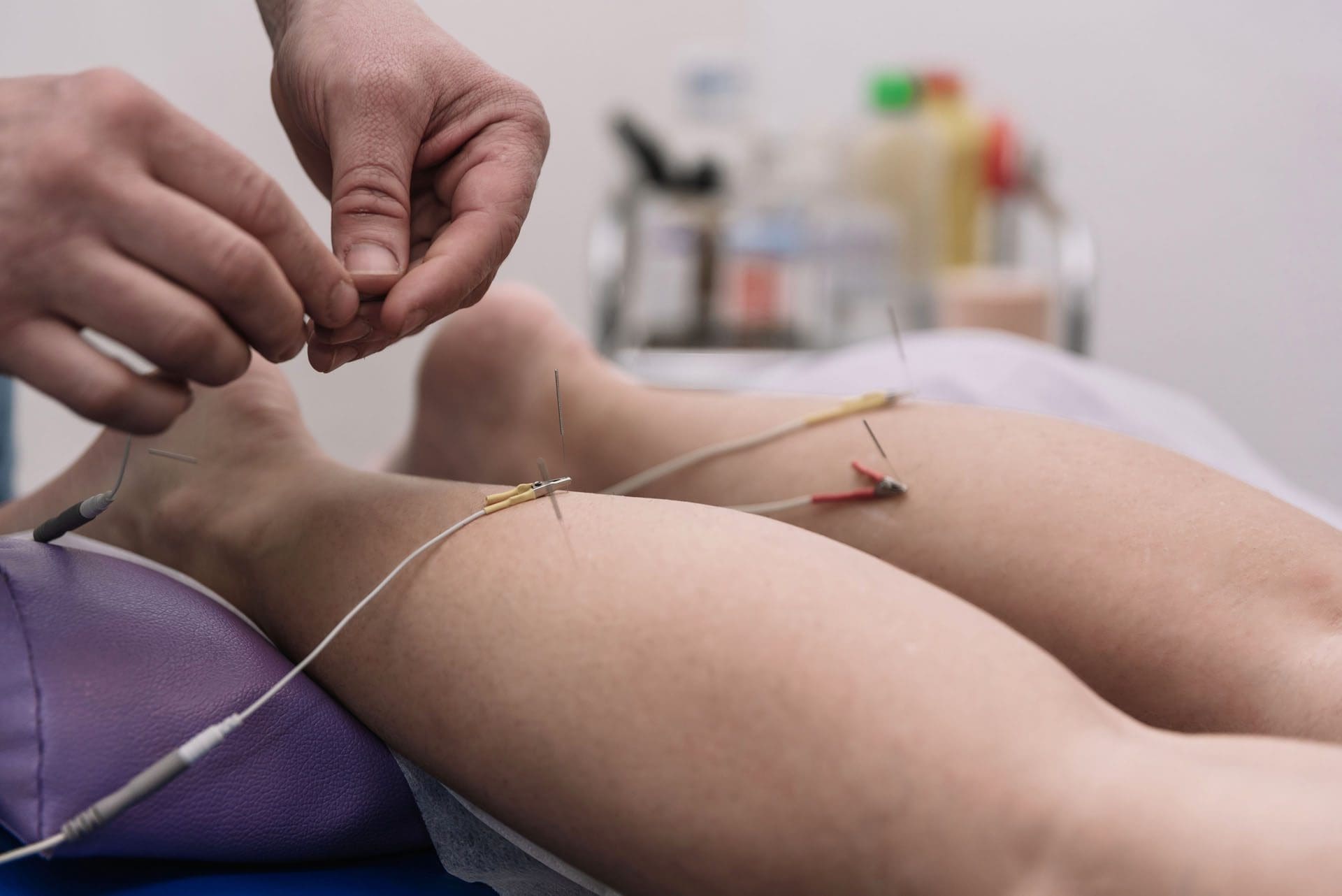
How acupuncture helps relieve sciatica
Acupuncture can help relieve sciatica pain by stimulating specific points on the body, which can trigger the release of endorphins, reduce inflammation, improve blood flow, and relax tight muscles that could be compressing the sciatic nerve. By modulating the nervous system and promoting the body’s natural healing processes, acupuncture can help alleviate pain and improve overall function. (Qin, Z. et al., 2015)
Releases endorphins
- Acupuncture stimulates the nervous system, triggering the release of endorphins, the body’s natural painkillers.
Reduces inflammation
- Acupuncture can help reduce inflammation in the area surrounding the sciatic nerve, which can contribute to pain and nerve irritation. (Natural Care Chiropractic, 2022)
Improves circulation
- By increasing blood flow to the affected area, acupuncture can help deliver nutrients and oxygen to the sciatic nerve and surrounding tissues, promoting faster healing.
Relaxes tight muscles
- Sciatica pain can be exacerbated by tight muscles compressing the nerve. Acupuncture can help relax these muscles, reducing pressure on the sciatic nerve and alleviating pain.
Regulates the nervous system
- Acupuncture can help regulate the nervous system, positively impacting pain perception and overall well-being. (Qin, Z. et al., 2015)
Promotes regeneration
- Some evidence suggests that acupuncture can promote sciatic nerve regeneration, potentially leading to long-term pain relief. (Natural Care Chiropractic, 2022)
Needling Types
Distal needling
- Acupuncture can also involve using points that are further away from the site of pain, which can also help to reduce pain and inflammation.
Local needling
- Points are also selected on or near the sciatic nerve’s path, which can help directly address the source of pain and inflammation. (Qin, Z. et al., 2015)
Holistic approach
- Acupuncture is often viewed as a holistic approach to pain management, addressing the symptoms of sciatica and the underlying causes and imbalances in the body.
Injury Medical Chiropractic and Functional Medicine Clinic
As a Family Practice Nurse Practitioner, Dr. Jimenez combines advanced medical expertise with chiropractic care to address various conditions. Our clinic integrates Functional Medicine, Acupuncture, Electro-Acupuncture, and Sports Medicine to create customized care plans that promote natural healing, mobility, and long-term wellness. By focusing on flexibility, agility, and strength, we empower patients to thrive, regardless of age or health challenges. At El Paso’s Chiropractic Rehabilitation Clinic & Integrated Medicine Center, we passionately focus on treating patients after injuries and chronic pain syndromes. We focus on improving your ability through flexibility, mobility, and agility programs tailored for all age groups and disabilities. We use in-person and virtual health coaching and comprehensive care plans to ensure every patient’s personalized care and wellness outcomes.
Chiropractic and Integrative Healthcare
References
Cedars Sinai. (2025). Piriformis Syndrome. https://www.cedars-sinai.org/health-library/diseases-and-conditions/p/piriformis-syndrome.html#:~:text=Overview,can%20run%20through%20the%20muscle)
Noonan, A. M., & Brown, S. H. M. (2021). Paraspinal muscle pathophysiology associated with low back pain and spine degenerative disorders. JOR spine, 4(3), e1171. https://doi.org/10.1002/jsp2.1171
Hospital for Special Surgery. (2024). Sciatica. https://www.hss.edu/condition-list_sciatica.asp
Qin, Z., Liu, X., Wu, J., Zhai, Y., & Liu, Z. (2015). Effectiveness of Acupuncture for Treating Sciatica: A Systematic Review and Meta-Analysis. Evidence-based complementary and alternative medicine: eCAM, 2015, 425108. https://doi.org/10.1155/2015/425108
Natural Care Chiropractic, D. M. F. (2022). Acupuncture for Sciatica Pain Relief. https://www.naturalcarechiropractic.com/post/acupuncture-for-sciatica-pain-relief