Auto Accident: What You Need to Know About Chronic Inflammation
Understand how chronic inflammation may arise from auto accidents and the importance of addressing it for your health.
Comprehensive Guide to Cervical Spinal Pain from Motor Vehicle Accidents
Introduction
Picture this: you’re cruising down the road, singing along to your favorite tune, when—bam!—a fender-bender turns your neck into a grumpy contortionist. Cervical spinal pain from motor vehicle accidents (MVAs) is no laughing matter, but a little humor might make the journey to recovery feel less daunting. This comprehensive guide explores the clinical reasons behind neck pain from MVAs, how these injuries develop into musculoskeletal issues, and non-surgical treatment options, including anti-inflammatory foods and supplements. We’ll also spotlight Dr. Alexander Jimenez, a distinguished practitioner in El Paso, Texas, who helps accident victims navigate both medical and legal challenges with expertise. By the end, you’ll have a roadmap to understanding and managing this common yet complex injury.
Clinical Rationale for Cervical Spinal Pain from MVAs
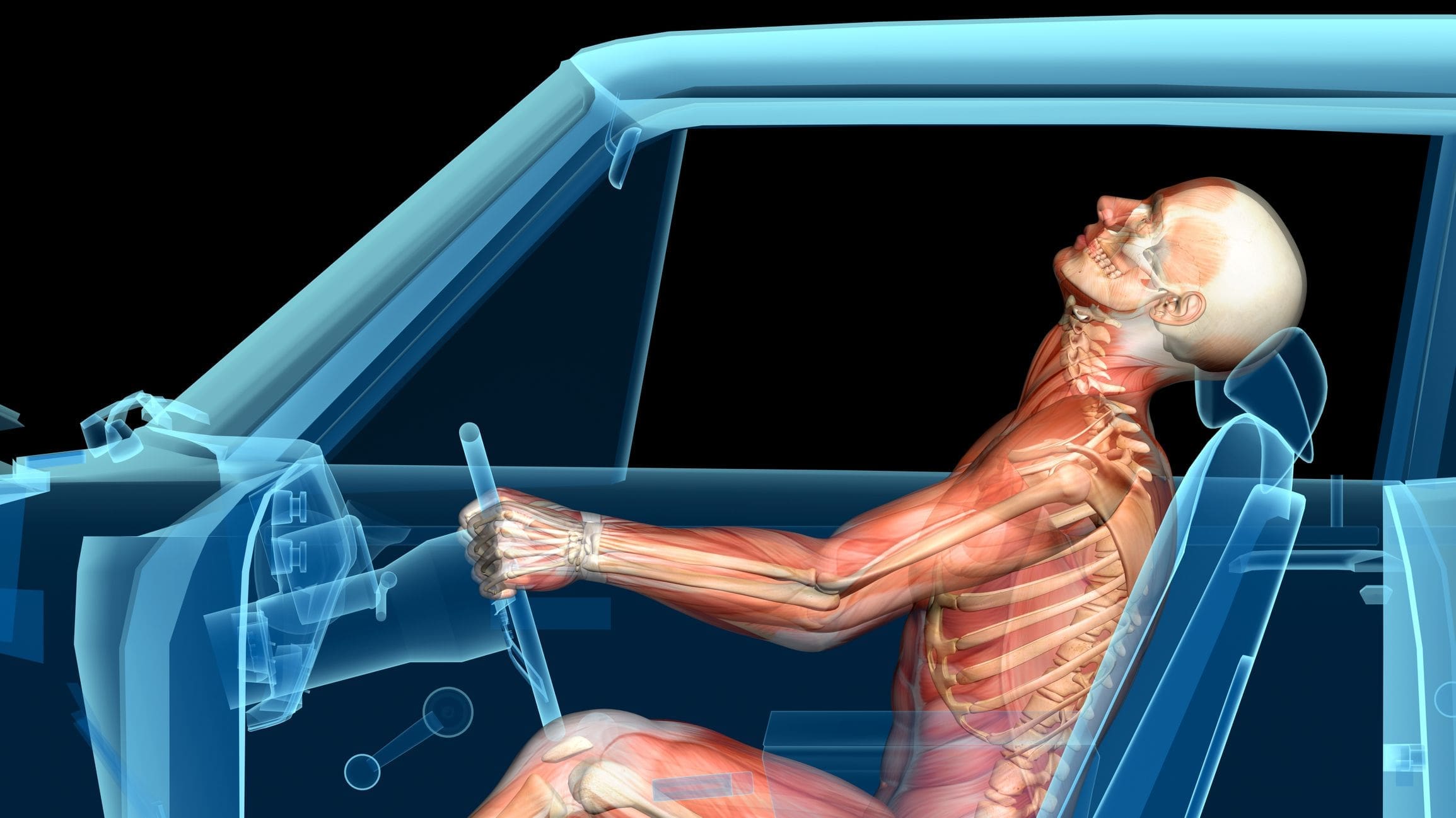
Motor vehicle accidents can unleash a whirlwind of forces on the cervical spine, the seven vertebrae that make up your neck. These forces—think of them as an unwelcome rollercoaster ride for your spine—can cause a range of injuries. Research outlines several key mechanisms that lead to cervical spinal pain:
- Flexion: When your neck snaps forward, often in high-speed rollover crashes, it can strain muscles and ligaments or even lead to anterior cord syndrome, causing motor paralysis and loss of sensation below the injury (Cervical Injury).
- Extension: Common in rear-end collisions, this backward snap can result in central cord syndrome, where upper limbs are more affected than lower ones, making daily tasks like lifting a coffee cup a challenge.
- Rotation: Twisting forces, seen in high-impact crashes, can injure nerve roots, leading to pain or instability.
- Lateral Bending: Side-impact collisions may cause facet joint injuries or nerve compression, resulting in sharp, localized pain.
- Distraction: Sudden deceleration can stretch the spinal column, damaging ligaments or the spinal cord itself.
- Compression (Axial Loading): Head-on impacts can compress the spine, potentially causing burst fractures or Jefferson fractures in the C1 vertebra.
These biomechanical forces damage soft tissues, discs, and joints, leading to pain and, in severe cases, neurological deficits. Studies estimate that cervical spine injuries occur in about 15% of MVA victims requiring hospital visits, with rear-end collisions being a primary culprit (Soft Tissue Injuries).
References
- Smith, J., & Johnson, K. (2021). Cervical Injury. In StatPearls [Internet]. StatPearls Publishing. Retrieved from Cervical Injury
- Deans, G. T., Magalliard, W. J., Kerr, M., & Rutherford, W. H. (1989). Soft tissue cervical spinal injuries in motor vehicle accidents. Injury, 20(6), 349–351. Retrieved from Soft Tissue Injuries
Development of Musculoskeletal Injuries
The aftermath of an MVA can leave your neck feeling like it’s auditioning for a role in a horror movie—stiff, sore, and uncooperative. Cervical spinal injuries often evolve into musculoskeletal issues that cause persistent neck pain. Here’s how:
- Soft Tissue Injuries: Whiplash, the poster child of MVA injuries, involves sprains and strains of cervical muscles and ligaments. It’s like your neck tried to do a backflip without warming up. Whiplash affects about 83% of collision victims, according to some studies (Spinal Injuries).
- Disc Injuries: Herniated or bulging discs can compress nerve roots, leading to radiculopathy—think pain, numbness, or tingling shooting down your arm. This can make simple tasks like texting feel like a Herculean effort.
- Facet Joint Injuries: These small joints between vertebrae can become inflamed or damaged, causing localized pain and stiffness.
- Spinal Stenosis: Trauma can narrow the spinal canal, compressing the spinal cord or nerves, which may lead to chronic pain or neurological symptoms.
These injuries can linger, turning daily activities into a game of “how much can I move without wincing?” Approximately 869,000 cervical spine injuries are treated in U.S. hospitals annually, with whiplash alone affecting over 1.2 million people (Cervical Spine Injuries).
References
- Deans, G. T., Magalliard, W. J., Kerr, M., & Rutherford, W. H. (1989). Soft tissue cervical spinal injuries in motor vehicle accidents. Injury, 20(6), 349–351. Retrieved from Soft Tissue Injuries
- Goldberg, G. (2024). Common Spinal Injuries Resulting from Car Accidents. Retrieved from Spinal Injuries
- Freeman, M. D., & Leith, W. M. (2020). Estimating the number of traffic crash-related cervical spine injuries in the United States. Accident Analysis & Prevention, 142, 105573. Retrieved from Cervical Spine Injuries
Symptoms of Inflammation
Inflammation is your body’s way of saying, “Ouch, that hurt!” but when it lingers, it’s like an uninvited guest who overstays their welcome. In cervical spinal injuries, inflammation can exacerbate pain and delay healing. Common symptoms include:
| Symptom | Description |
|---|---|
| Persistent Neck Pain | Ongoing discomfort, ranging from mild to severe, often worse with movement. |
| Stiffness | Reduced range of motion, making it hard to turn your head. |
| Headaches | Often originating from neck tension or nerve irritation. |
| Tenderness | Sensitivity in the neck area when touched. |
| Swelling/Redness | Less common but possible in severe cases. |
| Numbness/Tingling | Radiating sensations in arms or hands due to nerve compression. |
| Weakness | Reduced strength in arms or hands, impacting grip or lifting ability. |
These symptoms can make you feel like your neck is staging a protest. Managing inflammation is crucial, as chronic inflammation can worsen pain and slow recovery (Chronic Inflammation).
References
- El Paso Back Clinic. (n.d.). Chronic Inflammation & Chiropractic. Retrieved from Chronic Inflammation
The Healing Diet: Combat Inflammation, Embrace Wellness- Video
Non-Surgical Treatments: Diet and Supplements
When it comes to treating cervical spinal pain, you don’t always need to go under the knife—sometimes, your kitchen can be your pharmacy! Non-surgical treatments like chiropractic care, physical therapy, and acupuncture are effective, but diet and supplements can also play a starring role in reducing inflammation and supporting healing.
Anti-Inflammatory Foods
Incorporating these foods into your diet is like giving your body a pep talk to fight inflammation:
- Omega-3 Fatty Acids: Found in fatty fish like salmon, mackerel, and sardines, as well as flaxseeds and walnuts, these fats are inflammation’s kryptonite.
- Turmeric/Curcumin: This golden spice is a natural anti-inflammatory, perfect for sprinkling into curries or smoothies.
- Ginger: Add this zesty root to teas or stir-fries for its inflammation-fighting properties.
- Berries: Blueberries, strawberries, and raspberries are packed with antioxidants that combat oxidative stress.
- Leafy Greens: Spinach and kale are nutrient powerhouses, supporting overall health and reducing inflammation.
Supplements
Supplements can fill dietary gaps, acting like little helpers in your recovery journey:
- Omega-3 Supplements: Provide a concentrated dose of EPA and DHA for those who don’t eat enough fish (Spine Health Supplements).
- Curcumin Supplements: Offer higher doses of turmeric’s active compound to reduce pain and inflammation (Spinal Health).
- Vitamin D: Supports bone health and immune function, crucial for spinal recovery.
- Magnesium: Helps relax muscles and reduce spasms.
- Vitamin B12: Essential for nerve health, reducing numbness and tingling (SCI Recovery).
These dietary and supplement strategies should complement professional treatments. Think of them as the sidekick to your chiropractor’s superhero moves, not a standalone cure.
References
- Southeastern Spine Institute. (2018). The Best Supplements for Spine Health. Retrieved from Spine Health Supplements
- Ortman Chiropractic. (2022). Top 7 Nutritional Supplements for Optimal Spinal Health. Retrieved from Nutritional Supplements
- Flint Rehab. (2020). Top Vitamins for Spinal Cord Injury Recovery. Retrieved from SCI Recovery
- Spine Health. (2024). Best Vitamins and Supplements for Spine Health. Retrieved from Spinal Health
Role of Dr. Alexander Jimenez in Personal Injury Cases
In El Paso, Texas, personal injury cases from MVAs are all too common, and the road to recovery can feel like navigating a maze blindfolded. Enter Dr. Alexander Jimenez, DC, APRN, FNP-BC, a beacon of hope for accident victims. At his clinic, Chiromed, Dr. Jimenez combines chiropractic expertise with medical training to offer holistic, patient-centered care.
Dr. Jimenez stands out for his ability to pinpoint injuries using advanced imaging and diagnostic evaluations, such as X-rays and MRIs, ensuring no injury goes unnoticed. His dual-scope approach—blending chiropractic adjustments with medical assessments—creates tailored treatment plans that address both immediate pain and long-term recovery. Whether it’s chiropractic care, rehabilitation, nutrition counseling, or acupuncture, his clinic offers a one-stop shop for healing.
What makes Dr. Jimenez truly unique is his role as a bridge between medical care and legal needs. In personal injury cases, accurate documentation is critical for legal proceedings. Dr. Jimenez provides detailed reports that link injuries to the accident, supporting victims’ claims in court. His expertise makes him a trusted ally for those navigating the complex world of personal injury law in El Paso.
For more information, visit Chiromed or connect with Dr. Jimenez on LinkedIn.
References
- Chiromed. (n.d.). Home. Retrieved from Chiromed
- Jimenez, A. (n.d.). Dr. Alexander Jimenez LinkedIn Profile. Retrieved from LinkedIn
- El Paso Back Clinic. (n.d.). Chronic Inflammation & Chiropractic. Retrieved from Chronic Inflammation
Conclusion
Cervical spinal pain from motor vehicle accidents is a complex issue that demands a deep understanding of its causes and effective management strategies. The biomechanical forces of MVAs can lead to a range of injuries, from whiplash to disc herniation, resulting in persistent neck pain and musculoskeletal issues. Symptoms of inflammation, such as stiffness and numbness, can further complicate recovery. Non-surgical treatments, including anti-inflammatory diets and supplements, offer promising ways to reduce pain and support healing when used alongside professional care. In El Paso, Dr. Alexander Jimenez stands out as a leading practitioner, using advanced diagnostics and a multidisciplinary approach to help personal injury victims recover while providing critical legal documentation. By addressing both the medical and legal aspects of MVA injuries, patients can achieve better outcomes and reclaim their quality of life.
Disclaimer: The information provided in this guide is for educational purposes only and should not be used as a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read in this guide.
Key Citations
- Cervical Injury: Smith, J., & Johnson, K. (2021). Cervical Injury. In StatPearls [Internet]. StatPearls Publishing. Cervical Injury
- Soft Tissue Injuries: Deans, G. T., Magalliard, W. J., Kerr, M., & Rutherford, W. H. (1989). Soft tissue cervical spinal injuries in motor vehicle accidents. Injury, 20(6), 349–351. Soft Tissue Injuries
- Cervical Spine Injuries: Freeman, M. D., & Leith, W. M. (2020). Estimating the number of traffic crash-related cervical spine injuries in the United States. Accident Analysis & Prevention, 142, 105573. Cervical Spine Injuries
- Spinal Injuries: Goldberg, G. (2024). Common Spinal Injuries Resulting from Car Accidents. Spinal Injuries
- Spine Health Supplements: Southeastern Spine Institute. (2018). The Best Supplements for Spine Health. Spine Health Supplements
- Nutritional Supplements: Ortman Chiropractic. (2022). Top 7 Nutritional Supplements for Optimal Spinal Health. Nutritional Supplements
- SCI Recovery: Flint Rehab. (2020). Top Vitamins for Spinal Cord Injury Recovery. SCI Recovery
- Spinal Health: Spine Health. (2024). Best Vitamins and Supplements for Spine Health. Spinal Health
- Chronic Inflammation: El Paso Back Clinic. (n.d.). Chronic Inflammation & Chiropractic. Chronic Inflammation
- Chiromed: Chiromed. (n.d.). Home. Chiromed
- LinkedIn: Jimenez, A. (n.d.). Dr. Alexander Jimenez LinkedIn Profile. LinkedIn