PRP Therapy for Sports Injuries: Non-Surgical Healing

Sports injuries can slow people down fast. A sore tendon, strained ligament, pulled muscle, or painful joint can make training, work, and daily movement much harder. Many people want relief, but they also want a treatment that does more than cover up pain. That is one reason Platelet-Rich Plasma, or PRP, has gained attention in sports medicine. PRP is made from a person’s own blood and is used to deliver a high concentration of platelets and growth factors to an injured area. Those platelets may help support tissue repair, reduce inflammation, and improve recovery in selected injuries (Johns Hopkins Medicine, n.d.; Yale Medicine, n.d.).
At ChiroMed, the message on regenerative care is clear: the goal is to help the body heal naturally and non-surgically while also considering the bigger picture of movement, structure, inflammation, and long-term function. ChiroMed describes its care model as integrated medicine, combining chiropractic care, nurse practitioner services, rehabilitation, nutrition counseling, acupuncture, and other supportive services to improve recovery and function. The clinic also offers regenerative care as part of a broader plan to address the root cause of pain rather than merely masking symptoms.
What PRP Therapy Is
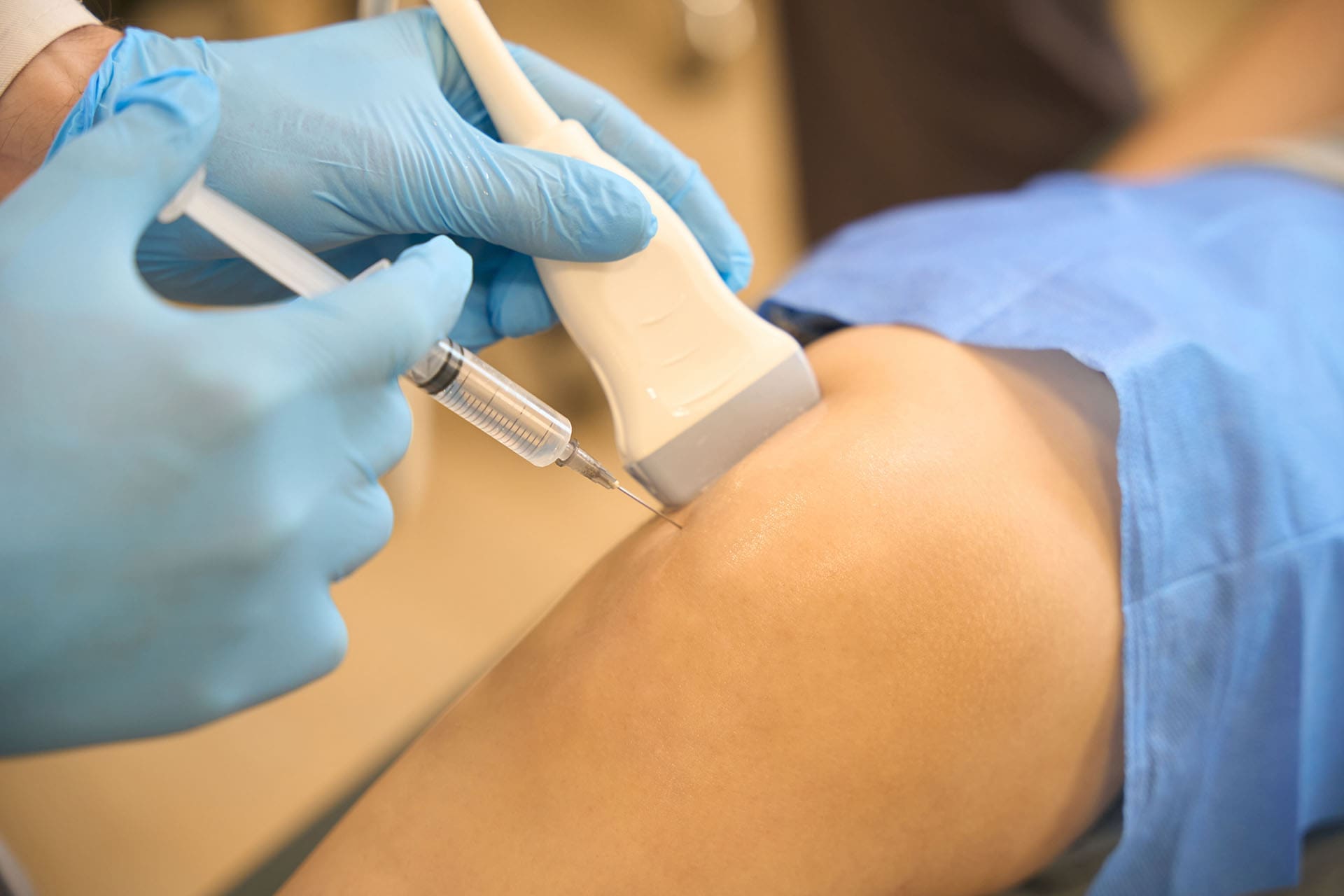
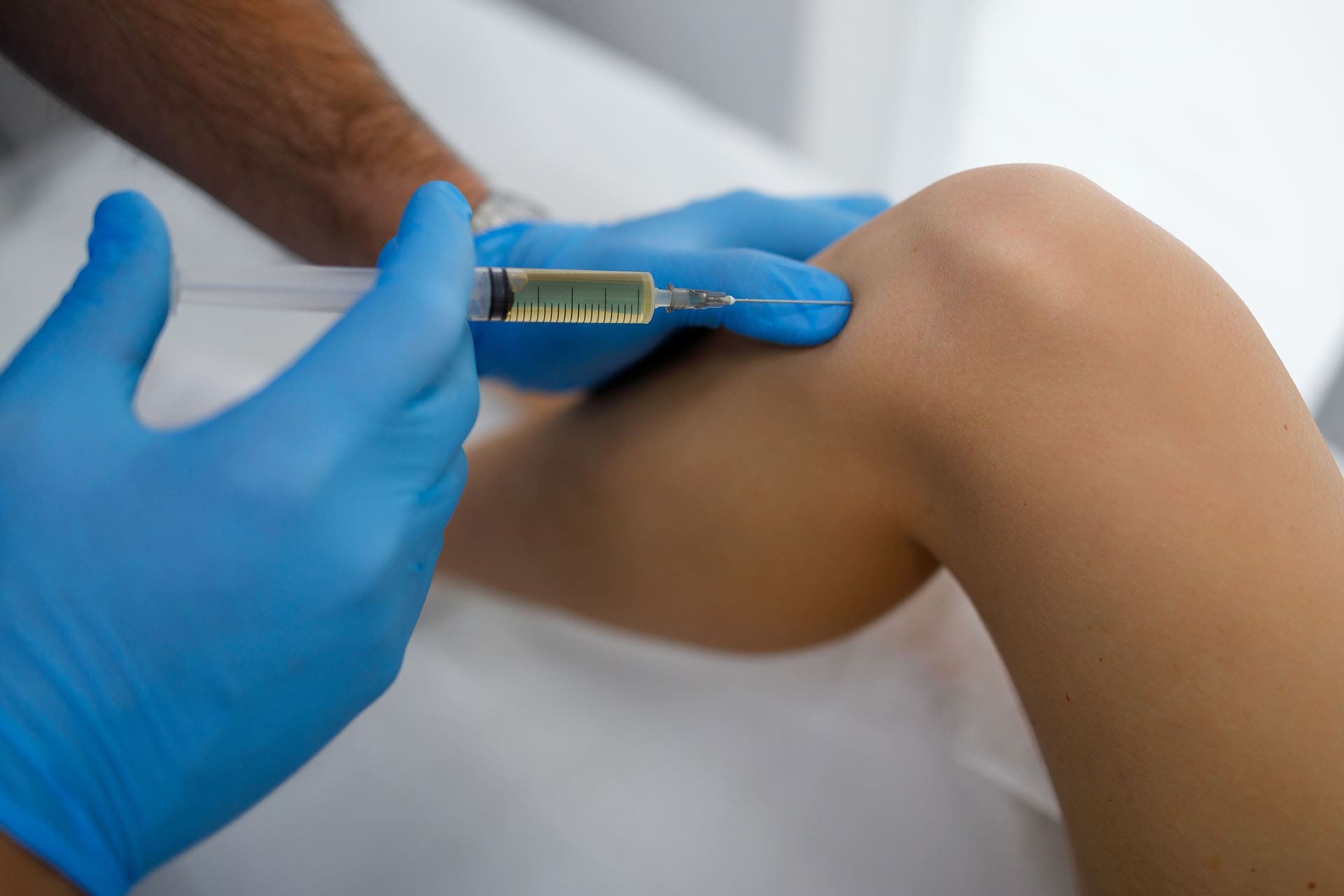
PRP therapy starts with a simple blood draw. The blood is placed in a centrifuge, which spins it to separate and concentrate the platelets. That platelet-rich portion is then placed into the injured area. Yale Medicine explains that PRP is a biologic therapy derived from the patient’s own blood and may stimulate healing and enhance repair in certain orthopedic injuries. Johns Hopkins adds that platelets are known for clotting, but they also contain growth factors that can trigger cell reproduction and support tissue regeneration or healing.
This matters because many sports injuries involve tissues that heal slowly. Tendons, ligaments, cartilage, and some muscle injuries do not always recover quickly, especially when the area has low blood supply or has been irritated for a long time. PRP is designed to concentrate the body’s healing signals and place them where they are needed most. HSS describes PRP as a form of regenerative medicine that amplifies the natural growth factors found in blood cells to promote the healing of damaged tissues.
Injuries PRP Is Commonly Used For
PRP is often discussed for sports and orthopedic injuries involving soft-tissue overload, chronic irritation, or joint wear. Penn Medicine says PRP is often used for sports injuries and arthritis, and it highlights its use in nonsurgical conditions like tennis elbow and tendinitis, as well as in tendon and soft tissue injuries, for people trying to avoid surgery. Yale Medicine also lists tendon, ligament, muscle, and cartilage injury among the problems that may be treated with PRP. HSS includes tendonitis, ligament injuries, and osteoarthritis among conditions commonly treated with PRP.
Common examples include:
- Chronic tendinitis or tendinopathy
- Tennis elbow and golfer’s elbow
- Achilles tendon problems
- Ligament sprains or partial tears
- Muscle strains or tears
- Knee pain related to joint wear
- Mild to moderate osteoarthritis
- Other overuse injuries that have not improved enough with standard care
At ChiroMed, regenerative medicine content also describes PRP as a tool used for joint pain, tendon injuries, and muscle damage. The site presents PRP as part of a larger regenerative care model that may also include PRF, MFAT, and peptide-based support depending on the patient and the clinical plan.
How PRP May Help Sports Injury Recovery
PRP is not a pain pill. It does not simply numb the area or hide symptoms for a few hours. Instead, it is used to support the body’s healing environment. Yale Medicine notes that PRP delivers a high concentration of platelets, growth factors, and cytokines to the injury site to promote healing. Penn Medicine states that PRP may stimulate tissue repair, reduce inflammation, and speed recovery.
For athletes and active adults, that may matter in several ways:
- It may help calm long-term irritation in injured tissue
- It may support tissue repair in tendons, ligaments, muscles, and joints
- It may improve function over time
- It may fit into a plan designed to delay or avoid surgery
- It may support return to activity when paired with proper rehab and load management
Still, PRP is not a shortcut for every injury. Results vary based on the diagnosis, how long the injury has been present, the quality of the tissue, the patient’s overall health, and how well the rest of the recovery plan is followed. That is why careful evaluation matters so much.
What the Procedure Usually Feels Like
Penn Medicine explains that PRP is created by removing a small amount of blood, processing it to isolate platelets, and then injecting the concentrated platelets into the area needing treatment. Johns Hopkins also notes that in some cases, a clinician may use ultrasound to guide the injection so the treatment reaches the target area more accurately.
Most people are also told to expect some short-term soreness. Yale Medicine says the most common side effects are discomfort, pain, and stiffness at the injection site. Johns Hopkins says soreness and bruising at the injection site may happen after the procedure, but major side effects are uncommon. HSS also describes PRP side effects as limited because the injection is made from the person’s own blood.
That means patients should understand two things:
- Temporary soreness after PRP can be normal
- Improvement often happens gradually over several weeks, not overnight
Why ChiroMed’s Integrative Model Fits PRP Well
A sports injury rarely affects only one body part. A painful tendon may also change how a person walks, lifts, throws, runs, or sleeps. Joint pain may lead to compensation patterns, weakness, and poor movement mechanics. That is why PRP often works best as part of a comprehensive recovery plan rather than a stand-alone procedure. ChiroMed’s website repeatedly frames recovery through an integrated model that combines chiropractic care, nurse practitioner services, rehabilitation, nutrition support, and other natural therapies.
ChiroMed also describes regenerative medicine as a natural, non-surgical approach that is often paired with structural chiropractic care. On its regenerative medicine page, the clinic says regenerative care supports tissue repair, reduces inflammation, eases pain, and improves movement. It also states that the best results occur when regenerative medicine works alongside structural chiropractic care, giving the body a more stable foundation for healing.
In practical terms, that kind of clinic model may include the following:
- A careful examination to identify the true pain source
- PRP or other regenerative options when appropriate
- Chiropractic or structural care to improve motion and reduce joint stress
- Rehabilitation to rebuild strength and movement quality
- Nutrition and functional medicine support to improve recovery
- A staged return-to-training plan instead of random guessing
Clinical Observations Linked to Dr. Alexander Jimenez and ChiroMed
ChiroMed identifies Dr. Alexander Jimenez as a dual-licensed clinician with credentials as both a chiropractic doctor and an Advanced Practice Nurse Practitioner. The site says he leads a multidisciplinary team focused on holistic, patient-centered care. In ChiroMed’s regenerative medicine content, Dr. Jimenez is described as emphasizing root-cause care that addresses nutrition, inflammation, movement patterns, and stress, as well as the injury itself. The same page explains that he combines precise chiropractic care with regenerative methods to help rebuild structure, calm irritation, and restore functional movement.
That clinical viewpoint makes sense for athletes and active adults. Many injured patients need more than just pain relief. They need a better movement pattern, improved stability, healthier tissue recovery, and a plan for getting back to work, training, or sport safely. ChiroMed’s athlete care content also supports the idea of “optimal loading,” meaning patients often do better with modified activity rather than complete shutdown. That approach can be important after PRP, as tissue healing still needs to be matched with smart activity progression.
PRP and Return to Activity
One reason PRP is attractive in sports medicine is that it may support healing without surgery in selected cases. But that does not mean someone should rush back to full activity too soon. ChiroMed’s sports injury content stresses modified activity, staged progress, and clear communication about what movements are safe during recovery. That is important because healing tissue still requires time, even with regenerative treatment.
A smart return-to-activity plan often includes:
- Relative rest instead of complete inactivity
- Protection from movements that overload the injured area
- Mobility and stability work that does not increase symptoms
- Gradual loading as pain and function improve
- Ongoing reassessment if pain keeps returning
This is where an integrative setting can help. Instead of treating the injury in isolation, the team can track function, monitor symptoms, adjust training, support nutrition, and improve mechanics simultaneously. That may give patients a more complete recovery process than an injection alone.
A Balanced View of PRP
PRP is promising, but it should be explained honestly. It is not the right answer for every injury, and it does not guarantee a quick return to sports. The best candidates are usually people with the right diagnosis, realistic expectations, and a willingness to follow a full treatment plan. The strongest message from major health systems and from ChiroMed’s own content is that PRP works best as part of a thoughtful, evidence-informed recovery strategy.
For people dealing with chronic tendinitis, ligament strain, muscle injury, or osteoarthritis, PRP may offer a non-surgical option that supports tissue repair and may reduce pain over time. When paired with integrated medical services like those described on Chiromed.com, the goal becomes bigger than short-term symptom relief. The goal is better healing, better movement, and a stronger return to life and activity.
Conclusion
PRP therapy may help sports injuries heal by delivering a concentrated dose of the body’s own platelets and growth factors directly to damaged tissue. It is commonly used for tendon injuries, ligament strains, muscle problems, and osteoarthritis, and it may reduce pain while supporting tissue repair. Temporary soreness at the injection site can happen, but serious side effects are uncommon. At ChiroMed, PRP fits naturally into an integrative, non-surgical model that also includes APRN support, chiropractic care, rehabilitation, nutrition, and a structured return-to-activity plan. For the right patient, that kind of whole-body approach may offer a practical path toward stronger healing and better function.
References
ChiroMed. (2026, March 25). PRP for Meniscus Tears: Integrative Medicine.
ChiroMed. (2026, March 24). Regenerative Medicine: Natural Non-Surgical Healing.
ChiroMed. (2026, March 18). Can Athletes Keep Training During Integrative Care?.
ChiroMed. (n.d.). ChiroMed – Integrated Medicine Holistic Healthcare in El Paso, TX.
Hospital for Special Surgery. (n.d.). Platelet-Rich Plasma (PRP) Injection: How It Works.
Johns Hopkins Medicine. (n.d.). Platelet-Rich Plasma (PRP) Injections.
Penn Medicine. (n.d.). Platelet-Rich Plasma (PRP) Injections.
Yale Medicine. (n.d.). Platelet-Rich Plasma (PRP) Injections in Sports.