Platelet-Rich Plasma (PRP) Therapy for Sciatica

Natural Healing for Lasting Relief in El Paso
Sciatica brings sharp, shooting pain from the lower back down one leg. Many people in El Paso feel numbness, tingling, or weakness that makes walking or sitting difficult. The cause is often a herniated disc or pressure on the sciatic nerve. While pain pills or steroid shots may help for a short time, they do not fix the underlying damage.
At ChiroMed – Integrated Medicine in El Paso, Texas, patients find a better path. Platelet-rich plasma (PRP) therapy uses the body’s own healing power to reduce inflammation, repair discs, and support nerve recovery. This regenerative approach often provides longer-lasting relief without surgery.
This article explains how PRP works for sciatica and why ChiroMed’s integrative team, led by Dr. Alexander Jimenez, DC, APRN, FNP-BC, delivers complete care.
What Is Sciatica and How Does It Affect Daily Life?
Sciatica happens when something presses on the sciatic nerve, the longest nerve in the body. A bulging disc, tight muscles, or spinal misalignment can trigger it. Symptoms include burning pain, electric shocks down the leg, or weakness that reaches the toes.
In El Paso’s active community, sciatica affects people from work injuries, sports, car accidents, or everyday wear and tear. At ChiroMed, the focus is on finding the root cause instead of masking symptoms.
What Is Platelet-Rich Plasma (PRP) Therapy?
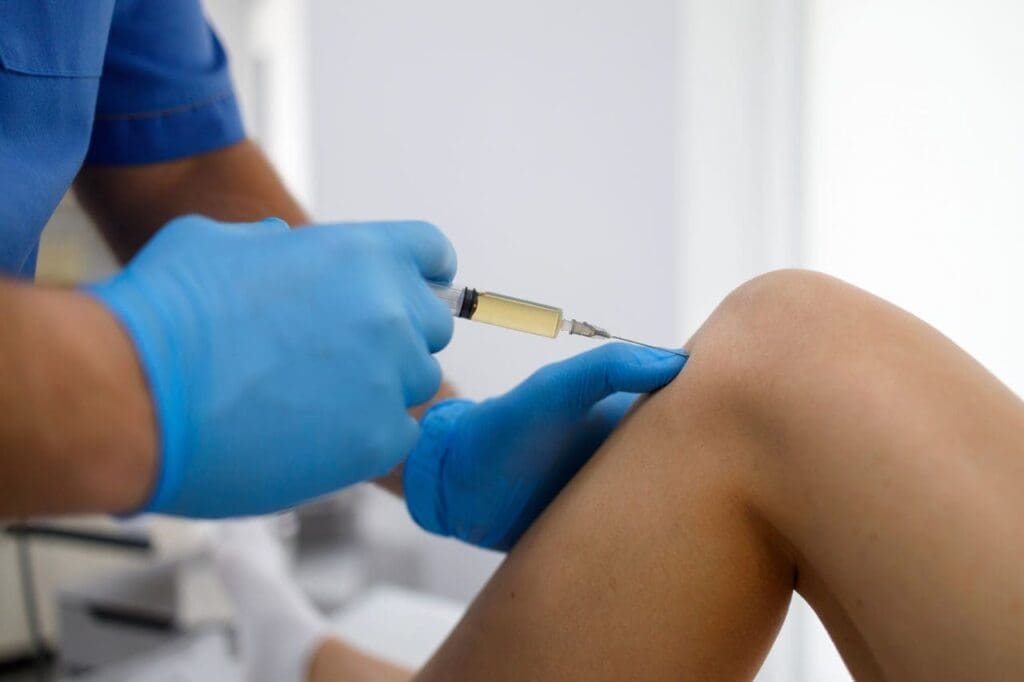
PRP therapy begins with a simple blood draw. The blood spins in a centrifuge to concentrate the platelets. These platelets contain powerful growth factors that signal the body to heal.
Doctors then inject the concentrated PRP into the damaged area. Because it comes from your blood, the risk of reaction is very low. PRP acts as a natural repair treatment, reducing swelling and rebuilding tissue.
At ChiroMed, PRP is part of a broader regenerative medicine program. The clinic uses it alongside chiropractic care and functional medicine for full recovery.
How PRP Therapy Helps Sciatica by Repairing Tissue and Calming Nerves
PRP therapy helps sciatica by injecting the patient’s own concentrated platelets into damaged spinal areas. This reduces inflammation, repairs discs, and supports nerve regeneration.
Instead of just covering pain like steroid injections, PRP stimulates real healing at the nerve root. Growth factors encourage new tissue growth and better blood flow in areas that normally heal slowly, such as spinal discs.
Clinical observations show PRP can ease shooting sensations and numbness. Many patients at ChiroMed report steady improvement over weeks as the body rebuilds damaged structures.
Key benefits include the following:
- Lower inflammation around the irritated sciatic nerve
- Repair of discs, ligaments, and facet joints
- Support for nerve healing and reduced compression
- Stronger spinal stability for long-term relief
This regenerative method often outperforms temporary fixes for lasting results.
PRP Injections vs. Steroid Shots: A Better Choice for Long-Term Sciatica Relief
Steroid injections can reduce swelling quickly, but studies show their benefits often fade after a few months. One systematic review found short-term pain relief but little improvement in nerve function at one year.
PRP offers more. It promotes tissue repair rather than just calming symptoms. Patients frequently experience longer-lasting relief because the treatment addresses the damaged disc or ligament that is causing nerve compression.
At ChiroMed, Dr. Alexander Jimenez notes that combining PRP with chiropractic adjustments leads to better mobility and fewer flare-ups. The approach avoids many steroid side effects and supports the body’s natural healing.
Common PRP Injection Methods for Sciatica at ChiroMed
ChiroMed uses precise, image-guided methods for safety and effectiveness:
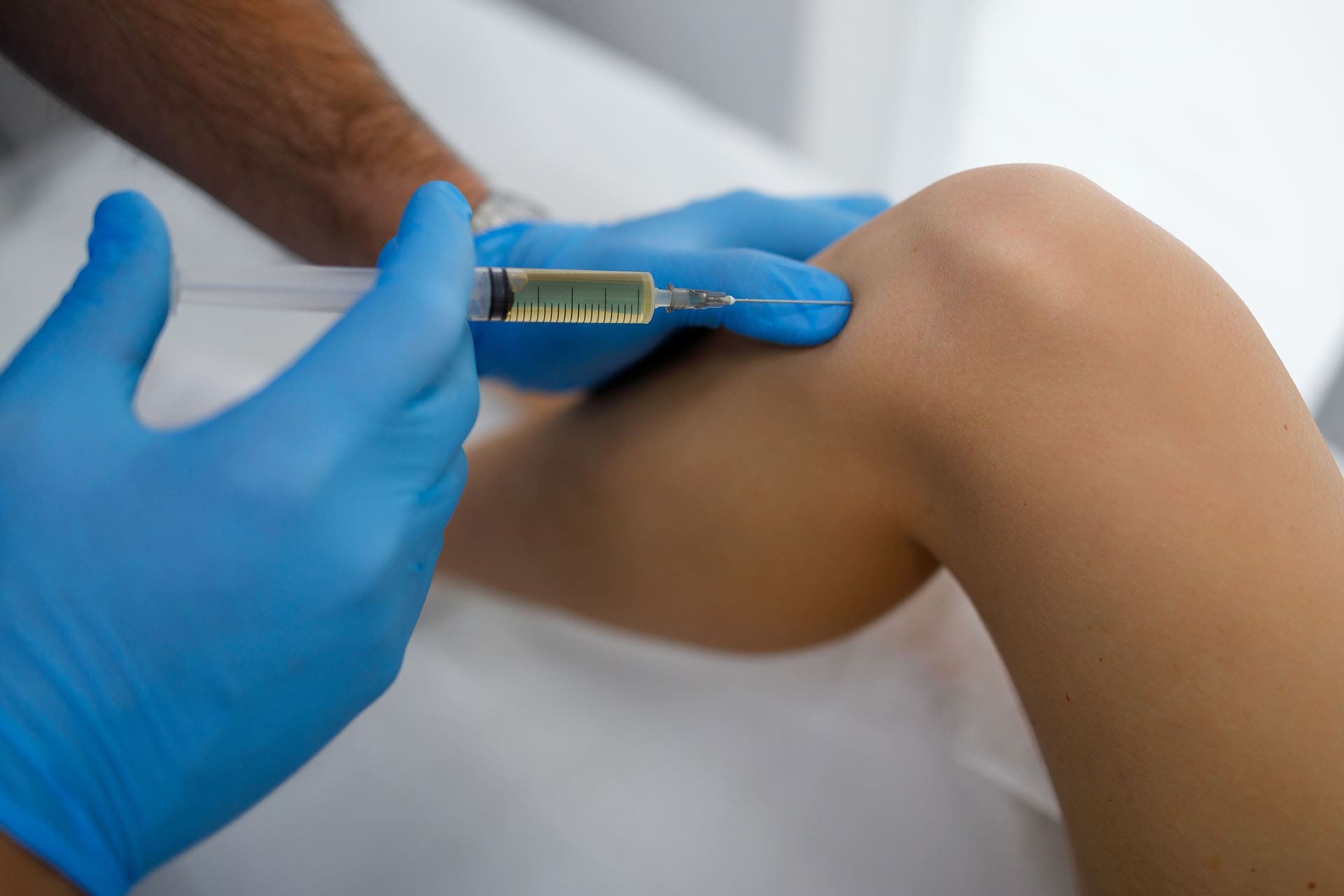
- Epidural PRP injection: Placed in the space around the spinal cord to target nerve root inflammation and promote healing.
- Direct injection into damaged discs or ligaments: Delivers growth factors directly to the injured area to promote disc repair and stability.
These minimally invasive procedures take little time. Most patients return to light activities the same day with only mild soreness.
ChiroMed’s team ensures each injection fits the patient’s specific needs as part of a personalized plan.
The Integrative Approach at ChiroMed: Chiropractic, APRN Care, and Functional Medicine
ChiroMed – Integrated Medicine stands out with its holistic team. Led by Dr. Alexander Jimenez, DC, APRN, FNP-BC, CFMP, IFMCP, the clinic combines chiropractic, advanced nursing practice, and functional medicine.
The team injects concentrated platelets from the patient’s own blood into damaged spinal discs, ligaments, or facet joints. This stimulates tissue repair, reduces inflammation, and heals nerve irritation. Sciatica symptoms like shooting pain and numbness often improve without surgery.
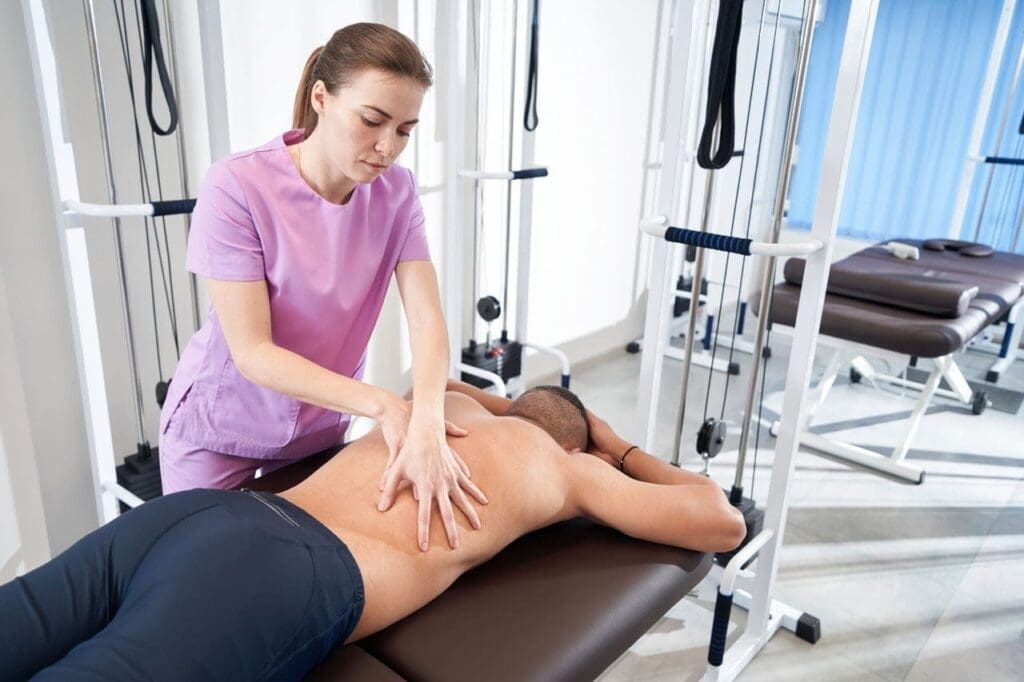
But PRP is only one piece. Chiropractic adjustments correct structural misalignment. Functional medicine optimizes nutrition, hormones, and lifestyle to support biochemical health. Together, these steps create lasting recovery.
Dr. Jimenez’s clinical observations highlight the power of this combined care. Patients with severe sciatica or herniated discs regain function faster when PRP pairs with spinal adjustments and wellness guidance. The goal is root-cause healing for El Paso patients experiencing work-, sports-, or accident-related pain.
What to Expect During PRP Treatment at ChiroMed
Your visit starts with a thorough evaluation. The team reviews your history and imaging to confirm PRP is right for you.
The procedure is straightforward:
- A small blood draw from your arm.
- Centrifuge processing to concentrate platelets.
- Precise, guided injection into the target area.
Most people feel only mild pressure. Afterward, rest and ice help with any soreness. Unlike surgery, there is no long recovery period.
Benefits build gradually. Many notice less pain and improved movement within four to six weeks, with continued gains over the following months.
Evidence and Success Stories with PRP for Sciatica
Research supports PRP for back and nerve pain. Reviews show significant drops in pain scores and improved function. PRP helps create a better healing environment around compressed nerves.
At ChiroMed, the integrative model adds to these results. Dr. Jimenez and the team have helped many local patients avoid surgery through a combination of regenerative and chiropractic care. Their approach addresses both mechanical issues and overall body health for stronger, longer-lasting outcomes.
Why Choose ChiroMed for PRP Therapy and Sciatica Care in El Paso
If sciatica is slowing you down, ChiroMed offers a natural, non-surgical path forward. Located at 11860 Vista Del Sol Dr, Suite 128 in El Paso, the clinic provides personalized integrative care.
Dr. Alexander Jimenez and the multidisciplinary team focus on real healing. PRP therapy, chiropractic adjustments, and functional medicine work together to reduce pain and restore function.
Contact ChiroMed today to learn if PRP and their holistic approach can help you move freely again. Call (915) 412-6680 or visit Contact ChiroMed today to learn if PRP and their holistic approach can help you move freely again. Call (915) 412-6680 or visit https://chiromed.com/ for more information.
References
ChiroMed – Integrated Medicine. (n.d.). Regenerative medicine: Natural non-surgical healing.
Caring Medical. (2024). Platelet rich plasma therapy and lower back pain.
Envista Medical. (n.d.). Treating sciatica with platelet-rich plasma.
Jimenez, A. (n.d.). Injury specialists. https://dralexjimenez.com/
Naples Regenerative Institute. (n.d.). How PRP can treat your sciatica.