Stay Motivated with Easy Strategies for Weight Loss

Workouts for Long-Term Success
Starting a weight-loss workout plan feels exciting at first, but many people lose steam after a few weeks. Life gets busy, muscles get sore, or results seem slow. The good news is that motivation does not have to fade. Simple changes in how you approach workouts can keep you going strong. This guide shares practical tips for beginners and anyone looking to lose weight through exercise. You will learn how to set goals, build habits, make workouts fun, and use support systems. Later, we will explore how integrative chiropractic and functional medicine clinics make the whole process easier by fixing pain and other roadblocks. These steps focus on consistency, not perfection, so you can enjoy steady progress and feel better every day.
A few simple strategies to stay motivated:
- Create objectives that are SMART, or specific, measurable, attainable, relevant, and time-bound.
- Establish a routine and work your way up slowly.
- Make notes on your results to see real progress.
- Enhance the fun factor by picking activities you like.
- Celebrate with non-food rewards.
- Determine accountability with a partner or group.
- Keep your “why” in mind every day.
- Get ready for days with low energy.
Set SMART Goals That Feel Doable
Vague goals like “I want to lose weight” often fail because they are too big and hard to track. Instead, use SMART goals that give clear direction. SMART stands for Specific, Measurable, Attainable, Relevant, and Time-bound. For example, say “I will walk for 20 minutes, four days a week, for the next month” instead of just “exercise more.” This kind of goal tells you exactly what to do, how to measure it, and when to check progress (Hey Life Training, n.d.; Beskur, 2024).
Why does this help with weight-loss workouts? Clear goals keep your brain focused and give small wins that build confidence. Research shows that people who set process goals, such as walking a certain number of days, stick with exercise longer than those who only watch the scale (Pullen, 2026). Start with one or two SMART goals. Write them on your phone or a sticky note. Review them each Sunday. When you hit the goal, you feel proud and ready for the next week. Over time, these small steps add up to real fat loss and stronger muscles without feeling overwhelmed.
Build a Routine Gradually to Avoid Burnout
Jumping into hard workouts every day leads to sore muscles and quitting. The smarter path is to start small and add more over time. Begin with just 10 to 15 minutes of movement most days. Once that feels easy, increase to 20 or 30 minutes. Focus on showing up regularly rather than pushing super hard (HelpGuide.org, 2026; Babauta, n.d.).
Consistency beats intensity for weight loss. Short daily walks or gentle stretching create a habit your body and mind accept. Many people notice better energy and sleep after just two weeks of light routines. On busy days, even five minutes of marching in place counts. This approach prevents burnout and keeps motivation high because you never feel like a failure. Think of it like learning to ride a bike: you start with training wheels and slowly remove them as you get stronger.
Track Your Results and Watch Motivation Grow
Seeing proof that your efforts work is one of the best motivators. Keep a simple log of steps, workout minutes, or how your clothes fit. Draw a quick graph each week to show progress. Zen Habits points out that a visual graph of your steps or workout days can be a powerful motivator because it shows an upward trend over time (Babauta, n.d.).
You do not need fancy apps. A notebook or free phone tracker works fine. Measure your waist once a month or take a progress photo every four weeks. These records remind you how far you have come on tough days. People who track their activity lose more weight and keep it off because the numbers prove the workouts are paying off (Pullen, 2026). Celebrate when you hit new records, like 10,000 steps in a day. The visual wins keep you excited about weight-loss workouts.
Make Workouts Fun So You Actually Look Forward to Them
Exercise should not feel like punishment. Choose activities you enjoy, and motivation stays high. Try dancing to your favorite music for 15 minutes, swimming at the local pool, riding a bike on a scenic trail, or playing active video games like those on Wii or Kinect. These low-impact options burn calories without stressing joints (HelpGuide.org, 2026; Pullen, 2026).
Fun turns workouts into something you want to do, not something you have to do. Listen to podcasts or upbeat playlists while walking. Join a beginner dance class or a cycling class with friends. One study found that people who picked enjoyable activities exercised longer and more often. For weight loss, this matters because consistent movement beats perfect but miserable sessions every time. Experiment until you find two or three activities that make you smile. Rotate them to keep things fresh.
Easy, fun, low-impact exercises to try:
- Brisk walking in a park or around your neighborhood
- Swimming or water aerobics
- Gentle yoga flows at home or in a studio
- Dancing in your living room to your favorite songs
- Leisure cycling on flat paths
- Active video games that get you moving
Reward Yourself for Small Wins
After you complete five workouts in a week, give yourself a non-food treat. Buy new workout socks, watch a movie, or enjoy a long bath. Rewards train your brain to link exercise with positive feelings (Babauta, n.d.; Planet Fitness, n.d.).
Start with frequent small rewards in the beginning. After a month, stretch the time between treats. Non-food rewards work better for weight loss because they do not undo your calorie efforts. Many people report that these little celebrations keep them coming back even when motivation dips. The key is to plan the reward ahead so you have something positive to look forward to after each session.
Find Accountability That Keeps You Honest
Telling a friend or family member about your goals makes it harder to skip workouts. Better yet, find a workout buddy who joins you for walks or classes. Knowing someone expects you creates gentle pressure to follow through (Healthline, 2026; HelpGuide.org, 2026).
Accountability works because humans like to keep their word. Apps that share step counts with friends or group challenges also help. Some people get a dog that needs daily walks—this built-in buddy system adds motivation and extra steps. Whatever method you choose, regular check-ins turn solo weight-loss workouts into a team effort.
Remember Your “Why” on Tough Days
Write down your personal reasons for losing weight. Maybe you want more energy to play with kids, better sleep, or confidence in your favorite clothes. Read your “why” list every morning. Focus on feelings like extra energy or less joint pain rather than just a number on the scale (Planet Fitness, n.d.; Beskur, 2024).
Your “why” acts like an anchor when motivation fades. Studies show people driven by internal reasons stick with exercise longer than those pushed by outside pressure (Pullen, 2026). Keep the list in your phone or on the bathroom mirror. On low days, reading it reminds you why the effort matters. This mental boost often gets you moving even when you feel tired.
Plan Ahead for Low-Energy Days
Everyone has days when workouts feel impossible. Have backup plans ready, like 10 minutes of gentle yoga or a slow stroll around the block. These light sessions still count and keep your streak alive (Beskur, 2024; HelpGuide.org, 2026).
Preparing alternatives stops all-or-nothing thinking that leads to quitting. Rest is important too—muscles repair on off days. Give yourself credit for any movement, even household chores done at a brisk pace. This flexible mindset protects long-term motivation for weight-loss workouts.
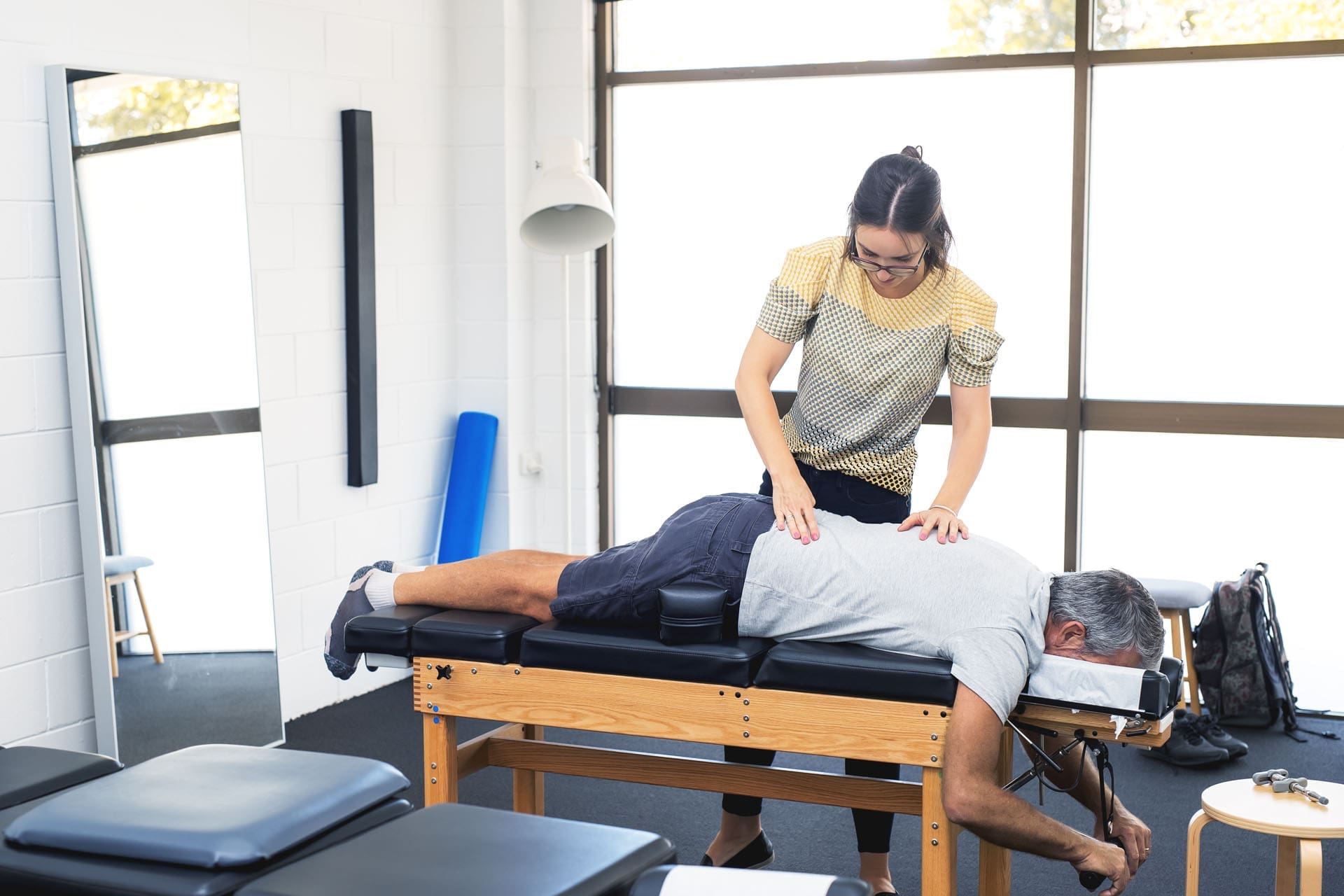
How Integrative Chiropractic and Functional Medicine Clinics Boost Motivation
Pain, stiffness, or low energy can kill workout drive fast. Integrative chiropractic and functional medicine clinics address these root problems so exercise feels possible again. By lowering pain levels, increasing mobility, and removing metabolic roadblocks, these clinics make weight loss more attainable and less scary.
Key ways these clinics help keep you motivated:
- Reduced pain and increased mobility through gentle adjustments
- Individualized low-impact workout plans that fit your body
- Fixing underlying metabolic or hormonal issues
- Stress management that lowers cortisol and improves mood
- Regular check-ins for personalized accountability
- Better posture and confidence that encourage continued movement
Chiropractic adjustments realign the spine and joints, easing chronic back, hip, or knee pain that often stops people from exercising. Patients report they can walk or stretch longer without discomfort after just a few sessions (Krueger, 2010; Adjusted Life Chiropractic, n.d.). Improved mobility means everyday tasks and workouts become easier, creating a positive cycle where movement feels beneficial instead of painful.
Functional medicine looks deeper at hormones, digestion, and nutrition that affect weight. Specialists identify issues such as a sluggish thyroid or inflammation that can slow metabolism. Simple diet tweaks and supplements then support steady fat loss. When the body works better internally, energy rises, and cravings drop, making workouts feel natural.
Stress is a hidden weight-gain villain because it raises cortisol, which stores belly fat and zaps motivation. Chiropractic care calms the nervous system, lowers stress hormones, and improves sleep. Better rest means more energy for morning walks or evening yoga (Adjusted Life Chiropractic, n.d.).
Clinics create personalized accountability through follow-up visits and custom plans. Patients feel supported, not judged, which builds confidence. Improved posture from adjustments also lifts self-image, making people prouder to show up for workouts.
Clinical observations from Dr. Alexander Jimenez, DC, APRN, FNP-BC
In his El Paso practice at Injury Medical Clinic, Dr. Alexander Jimenez combines chiropractic adjustments with functional medicine to help patients overcome pain barriers. He has observed that spinal adjustments restore nerve function, reduce inflammation, and improve mobility, allowing individuals with long-term discomfort to begin low-impact activities such as walking or swimming. Many patients report higher energy, better sleep, and reduced stress after care, which directly supports consistent weight-loss workouts (Jimenez, n.d.). His integrative approach addresses metabolic and hormonal factors through personalized nutrition and lifestyle changes, helping remove roadblocks that traditional programs miss. Testimonials from his clinic highlight restored function after injuries, enabling return to daily movement and exercise without pain. Dr. Jimenez emphasizes natural healing and root-cause solutions, noting that when the nervous system functions optimally, patients feel motivated to maintain active lifestyles and achieve sustainable weight goals.
Clinics like his also suggest practical, low-impact workouts, such as water exercises or light resistance bands, that build strength without strain. These tailored programs fit real life and prevent the overwhelm that causes dropout. By combining chiropractic care, nutritional guidance, and stress management tools, patients see faster gains in energy and mobility, which fuel ongoing motivation.
Putting It All Together for Lasting Results
Staying motivated with weight-loss workouts is a skill you build one day at a time. Use SMART goals, track wins, keep things fun, reward effort, lean on accountability, remember your deeper reasons, and plan for off days. When pain or low energy holds you back, integrative chiropractic and functional medicine offer real solutions. Experts like Dr. Alexander Jimenez show how addressing the body as a whole—spine, metabolism, stress, and movement—makes exercise feel achievable and enjoyable.
Start today with one small change, like a 15-minute walk and a SMART goal. In a few weeks, you will notice more energy, looser clothes, and a stronger drive. The journey gets easier as habits form and support systems grow. You deserve to feel strong, confident, and healthy. Keep moving, celebrate progress, and watch your weight-loss goals become reality.
References
31 Ways to Motivate Yourself to Exercise. (n.d.). Zen Habits. https://zenhabits.net/31-ways-to-motivate-yourself-to-exercise/
5 Ways to Motivate Yourself to Exercise and Lose Weight. (n.d.). Hey Life Training. https://heylifetraining.com/5-ways-to-motivate-yourself-to-exercise-and-lose-weight/
Consistent Gym Motivation. (n.d.). Planet Fitness. https://www.planetfitness.com/blog/articles/consistent-gym-motivation
How to Get Motivated to Workout. Beskur, A. (2024, January 25). Cleveland Clinic. https://health.clevelandclinic.org/how-to-get-motivated-to-workout
How to Start Exercising and Stick to It. (2026, February 18). HelpGuide.org. https://www.helpguide.org/wellness/fitness/how-to-start-exercising-and-stick-to-it
Holistic Approaches to Weight Loss: Combining Chiropractic Care and Lifestyle Changes. (n.d.). Adjusted Life Chiropractic. https://adjusted.life/holistic-approaches-to-weight-loss-combining-chiropractic-care-and-lifestyle-changes/
Chiropractic Care – Who Knew?. Krueger, M. (2010, Spring). Obesity Action Coalition. https://www.obesityaction.org/resources/chiropractic-care-who-knew/
16 Ways to Motivate Yourself to Lose Weight. Pullen, C. (2026, January 21). Healthline. https://www.healthline.com/nutrition/weight-loss-motivation-tips
Injury Specialists – El Paso, TX Chiropractor Dr. Alex Jimenez DC. Jimenez, A. D. (n.d.). Injury Medical Clinic PA. https://dralexjimenez.com/
Weight Loss Journey Tips. (n.d.). Planet Fitness. https://www.planetfitness.com/blog/articles/weight-loss-journey-tips