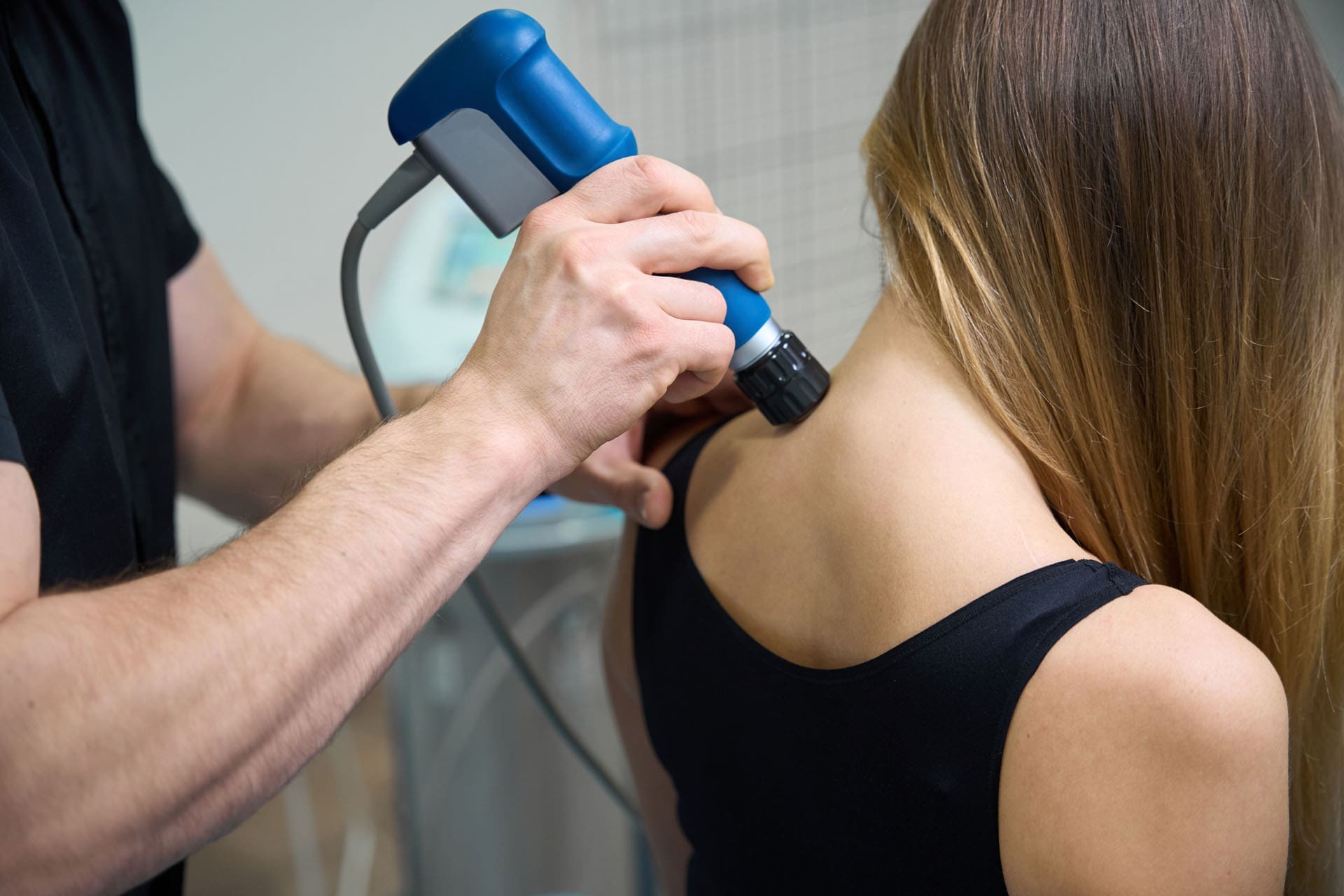
Can Athletes Keep Training During Integrative Care?

Athletes often worry that an injury means they have to stop training completely. In many cases, that is not true. At ChiroMed, the goal is usually not “do nothing” and wait. The goal is to keep the athlete moving in a smart, controlled way while the body heals. ChiroMed describes its approach as integrated medicine, offering chiropractic care, nurse practitioner services, rehabilitation, nutrition counseling, acupuncture, and other supportive services that work together to improve function and recovery. That kind of model fits well with athletes because sports injuries rarely affect just one part of the body. They often involve joints, muscles, nerves, movement patterns, recovery habits, and training load simultaneously.
For many athletes, complete rest is usually not the best long-term answer. A better strategy is often “optimal loading,” which means applying enough movement and stress to help healing without overloading the injured area. Research on athlete rehabilitation shows that injured athletes often do better when they follow a modified activity plan instead of becoming fully inactive. Modified training can reduce stiffness, maintain conditioning, protect skill development, and help athletes feel mentally connected to their sport during recovery.
Why Athletes Often Need Modified Training, Not Full Shutdown
When athletes stop everything for too long, the body can lose strength, coordination, and endurance. Joints can become stiffer, muscles can weaken, and movement patterns can become less efficient. That is why many sports medicine and chiropractic sources recommend relative rest rather than total rest for many non-emergency injuries. Relative rest means reducing activities that worsen symptoms while still performing safe, targeted movements to support recovery.
At ChiroMed, this type of thinking matches the clinic’s broader integrative care model. The practice explains that it combines chiropractic care with rehabilitation, nutrition counseling, acupuncture, and support from a nurse practitioner. For an athlete, that means treatment is not limited to one quick adjustment. It can include movement correction, recovery planning, soft-tissue support, and guidance on returning to training in stages.
For example, an athlete with a low back flare-up may need to pause heavy lifting or contact drills but may still be able to do walking, biking, core stability work, mobility drills, and sport-specific skills at a lower intensity. A runner with knee pain may need to stop hill sprints for a while, but may still be able to use a bike, pool running, or strength exercises that do not irritate the knee. The point is not to ignore pain. The point is to keep progress going without worsening the injury.
How ChiroMed’s Integrative Model Supports Athletes
ChiroMed presents itself as an integrated medicine and holistic healthcare practice in El Paso. The clinic states that it offers chiropractic care, nurse practitioner services, naturopathy, rehabilitation, nutrition counseling, and acupuncture. It also describes Dr. Alex Jimenez as a dual-licensed professional with chiropractic and advanced practice nursing credentials who leads a multidisciplinary, patient-centered team. For athletes, that matters because recovery is often better when multiple forms of care work together rather than in isolation.
This approach is especially helpful in sports because performance depends on more than just pain levels. An athlete may feel less pain after treatment, but that does not always mean the body is ready for full-speed cutting, jumping, sprinting, or heavy lifting. The athlete still needs enough mobility, strength, balance, endurance, and control to perform safely. ChiroMed’s sports and recovery content repeatedly points to a combined model of chiropractic care, soft-tissue support, corrective exercise, rehabilitation, and lifestyle support as the best path to stronger recovery and injury prevention.
What Care May Look Like for an Athlete
At ChiroMed, an athlete’s plan may include several layers of care working together. Based on the clinic’s services and sports-focused content, an athlete may receive:
- Chiropractic adjustments to improve joint motion and support movement quality
- Soft tissue work to reduce tightness and improve tissue function
- Rehabilitation exercises to rebuild stability and coordination
- Mobility drills to improve range of motion
- Nutrition guidance to support tissue repair and lower inflammation
- Acupuncture or other supportive therapies for pain and recovery
- Medical oversight from nurse practitioner services when a broader clinical view is needed
This matters because athletes need more than pain relief. They need a plan that helps them return to performance. ChiroMed’s own sports-related material explains that sport-specific training, combined with chiropractic care, can enhance athletic performance, accelerate recovery, and reduce the risk of future injury by improving biomechanics, joint function, and flexibility.
When Athletes Can Usually Keep Training
In many situations, athletes can continue training while receiving chiropractic and integrative care, as long as their training is modified to match the stage of healing. That may mean reducing load, intensity, volume, or impact. It may also mean changing practice drills, limiting certain motions, or using cross-training to stay conditioned. The goal is to keep the athlete active while respecting tissue healing.
Safe modified training may include:
- Light aerobic work, such as walking, cycling, or swimming
- Gentle stretching and mobility work
- Controlled strengthening with lighter weights
- Non-contact drills
- Technique practice at reduced intensity
- Balance, coordination, or core control work
- Cross-training that avoids aggravating the injury
This kind of plan can help athletes keep important qualities such as conditioning, timing, and confidence. It can also reduce the emotional frustration that often comes with injury. Athletes usually feel better when they know they still have a structured path forward. Instead of feeling stuck, they feel guided.
When Athletes Need to Pull Back More
Even though complete rest is not always necessary, there are times when athletes should reduce training sharply or stop certain activities for a while. Pain that worsens with activity, significant swelling, loss of strength, joint instability, numbness, severe stiffness, or major changes in movement quality should not be ignored. Those signs may mean that the tissue needs more protection or that further evaluation is needed before returning to harder activity. The clinic’s integrated structure is helpful here because it allows athletes to receive broader support when the problem is more complex than simple soreness or mild strain.
Athletes also need a more careful return-to-play plan after more serious conditions, especially head injuries. In those situations, a staged progression is important, and the athlete should not rely solely on post-treatment symptom improvement. A structured, step-by-step return is safer than rushing back, even if the body “feels better” for a day.
ChiroMed’s Role in the Return-to-Play Process
One of the strongest ideas behind the ChiroMed model is that recovery should be personalized. The clinic emphasizes patient-centered care and a combination of specialties rather than a one-size-fits-all approach. That is precisely what athletes need. A high school sprinter, a college volleyball player, a weightlifter, a golfer, and a weekend runner all place different demands on the body. Their return-to-play plans should not look the same.
A staged recovery plan often moves through these steps:
- Calm pain and reduce irritation
- Restore basic mobility
- Improve stability and control
- Build strength and endurance
- Add sport-specific movement
- Progress toward full-speed practice
- Return to competition when the function is ready
This kind of progression is helpful because pain alone is not the only measure of readiness. An athlete may say, “It does not hurt much anymore,” but still lack good balance, trunk control, hip strength, or reaction timing. ChiroMed’s rehabilitation and sports content suggests that the best results come from combining hands-on care with corrective exercise and function-based progressions.
Clinical Observations of Dr. Alexander Jimenez
Dr. Alexander Jimenez, DC, APRN, FNP-BC, is presented on ChiroMed as a dual-licensed chiropractor and nurse practitioner who leads a multidisciplinary team. The site describes his work as blending chiropractic care with broader medical and rehabilitation support. ChiroMed’s content also notes that integrative care can include spinal adjustments, soft tissue therapies, mobility work, corrective exercises, and guidance on lifestyle factors that affect healing. These observations align well with athletes’ needs during recovery, as sports injuries often affect multiple systems simultaneously.
From a practical standpoint, Dr. Jimenez’s integrative model supports the idea that athletes should not view recovery as either “all rest” or “full go.” Instead, they should see treatment as a structured partnership. The chiropractor and care team help decide what to protect, what to retrain, and when to progress. That mindset can help athletes return to training faster and more safely.
Smart Advice for Athletes Receiving Care at ChiroMed
Athletes usually do best when they communicate clearly and follow a plan instead of guessing. Helpful questions include:
- What movements should I avoid right now?
- What activities are safe this week?
- How hard can I train today?
- What signs mean I need to stop?
- What recovery work should I do between visits?
- When can I add speed, impact, or heavier loading back in?
A positive recovery mindset includes:
- Being honest about symptoms
- Following load limits
- Staying consistent with rehab exercises
- Focusing on sleep, hydration, and nutrition
- Progressing in stages instead of rushing
- Thinking long term, not just day to day
Conclusion
Yes, athletes can often continue training while receiving care at ChiroMed, but the training usually needs to be modified. The safest and most effective path is usually neither a total shutdown nor reckless pushing. It is controlled, guided, personalized training built around healing. ChiroMed’s integrated model, which combines chiropractic care, nurse practitioner services, rehabilitation, nutrition counseling, acupuncture, and other supportive care, is well-suited for that kind of athlete-centered recovery.
The bigger message is simple: injured athletes do not always need to stop moving. They need the right movement, the right timing, and the right plan. With a structured return-to-play strategy and a collaborative care team, athletes can protect healing tissues, maintain conditioning, and work their way back to full, pain-free performance with more confidence.
References
ChiroMed. (n.d.). About Us.
ChiroMed. (n.d.). ChiroMed – Integrated Medicine Holistic Healthcare in El Paso.
ChiroMed. (n.d.). Contact Us.
ChiroMed. (n.d.). Enhance Recovery: Chiropractic Sport-Specific Care.
ChiroMed. (n.d.). Integrated Medicine Services El Paso TX.
ChiroMed. (n.d.). Posture Improves Athletic Performance: Key to Success.
ChiroMed. (n.d.). Sleep, Athletic Recovery, and Integrative Chiropractic.
ChiroMed. (n.d.). Tag: chiropractic athletic performance care.
ChiroMed. (n.d.). Tag: chiropractic wellness programs.
ChiroMed. (n.d.). Tag: Dr Alex Jimenez ChiroMed.
ChiroMed. (n.d.). ChiroMed’s Integrative Path to Diet and Injury Healing.